Epilepsia é um grupo de doenças neurológicas não transmissíveis caracterizadas por uma predisposição a crises epilépticas recorrentes e não provocadas. Uma crise epiléptica é uma descarga súbita e anormal de atividade elétrica no cérebro, que pode provocar sintomas variados, desde lapsos breves de consciência até convulsões prolongadas. Esses episódios podem resultar em lesões físicas, tanto diretamente quanto por acidentes. O diagnóstico de epilepsia geralmente requer ao menos duas crises não provocadas com intervalo superior a 24 horas, embora, em alguns casos, possa ser estabelecido após um único episódio se houver evidências clínicas de alto risco de recorrência. Crises isoladas, sem risco de recorrência ou provocadas por causas identificáveis, não configuram epilepsia.
Introdução
O que você precisa saber de cara
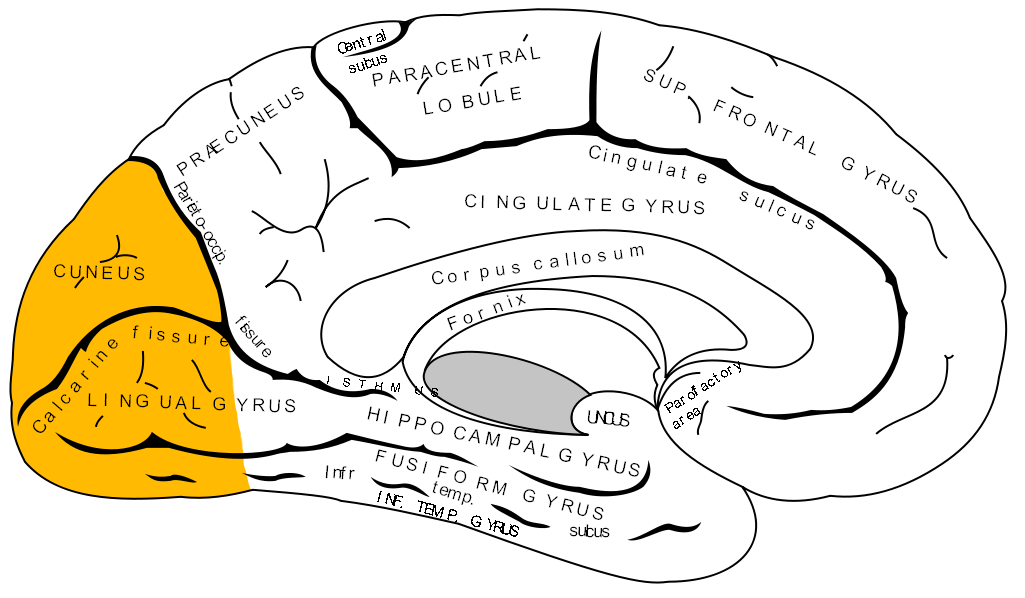
Epilepsia rara da infância com crises focais manifestadas por distúrbios visuais, como alucinações ou cegueira transitória, originadas no lobo occipital. Pode apresentar-se com ou sem generalização secundária.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Epilepsia visual occipital da infância
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Evolution into spike-and-wave activation in sleep in patients with self-limited focal epilepsies.
Self-limited focal epilepsies of childhood (SeLFE), while predominantly considered benign, are known to potentially manifest with spike-and-wave activation in sleep (SWAS) in a minority of patients METHODS: The medical records of individuals diagnosed with one of the SeLFE syndromes according to the ILAE 2022 diagnostic criteria, who were followed in our center between 1989-2023, were retrospectively analyzed. At least two awake and sleep EEGs were performed during a minimum 2-year follow-up. SWAS is considered as spike and wave discharges occupying ≥50% of NREM sleep with symmetrical or mildly asymmetrical bilateral or unilateral hemispheric distribution. Among 144 patients with SeLFE, 57(39.6%) were diagnosed with self-limited epilepsy with centrotemporal spikes (SeLECTS); 65(45.1%) with self-limited epilepsy with autonomic seizures (SeLEAS); and 22 (15.3%) with childhood occipital visual epilepsy (COVE). The mean age of seizure onset was 7.6, 5.6, and 8.5 years, respectively. Twelve (8.3%) evolved into SWAS (5 from SeLECTS, 6 from SeLEAS, 1 from COVE). Time elapsed between onset of first seizure and evolution into SWAS ranged from 5.2 to 75 months (mean: 26.8±19.8), 6.2-42.8 months (mean: 20.1±14.7 for patients with SeLECTS; 5.2-75.0 months (mean: 32.7±24.5) with SeLEAS, and 25.0 months with COVE). All except two patients had also cognitive or behavioral regression and were diagnosed as epileptic encephalopathy with spike-wave activation in sleep(EE-SWAS) and one patient was diagnosed with Landau-Kleffner syndrome. The most recent definition of ILAE highlights that SeLFEs are no longer recognized as "benign" epilepsies. Even with a low incidence rate, clinicians should always be cautious about the risk of SWAS development in these syndromes.
Clinical and Electrophysiological Characteristics and Prognosis of Childhood Occipital Visual Epilepsy in Light of Current ILAE Criteria.
ObjectivesChildhood Occipital Visual Epilepsy (COVE) is a self-limited epileptic syndrome that typically begins in late childhood or adolescence characterized by brief visual seizures. The recent 2022 International League Against Epilepsy (ILAE) classification distinguishes COVE from photosensitive occipital lobe epilepsy (POLE), emphasizing the absence of photic-induced seizures in COVE. In this study, we aimed to describe the clinical and electrophysiological features of patients with COVE diagnosed according to the new ILAE criteria.MethodsThis retrospective cohort study analyzed 30 patients diagnosed with COVE at a tertiary epilepsy center between 1988 and 2023. Patients were selected based on ILAE 2022 criteria, and all cases with intermittent photic stimulation (IPS)-induced seizures were excluded.ResultsMost patients (93%) presented with elementary visual hallucinations, such as colorful lights. Orofacial seizures occurred in 7%, and 37% had nocturnal seizures. EEG abnormalities were primarily occipital and resolved in 85% of cases over time. Generalized spike-wave discharges (GSWDs) were rare (5%), and only one patient developed juvenile myoclonic epilepsy during follow-up. At final follow-up, 77% of patients achieved seizure freedom, and 47% discontinued medication.ConclusionCOVE is an epileptic syndrome associated with a favorable prognosis. By excluding photosensitivity in light of the newly proposed diagnostic criteria from the ILAE, future research should focus on a more homogenous group of COVE patients to enhance understanding of this syndrome. Accurate classification using updated ILAE criteria allows for clearer clinical delineation and more reliable outcome predictions.
Effectiveness and tolerability of perampanel monotherapy in children with newly diagnosed focal epilepsy.
To examine the clinical effectiveness and tolerability of perampanel (PER) as initial monotherapy in pediatric patients with newly diagnosed focal epilepsy. A retrospective analysis was conducted on 62 children with newly diagnosed focal epilepsy who were treated with PER at the Epilepsy Center of Jinan Children's Hospital from July 2021 to July 2022. The treatment status, prognosis, and adverse reactions were followed up for a minimum of 6 months after the initiation of PER monotherapy. The effectiveness of the patients was estimated by the PER effective rate at 3-, 6-, and 12-month follow-up evaluations and adverse reactions were also recorded. The effective rates of PER in different etiologies and epilepsy syndromes were also statistically analyzed. The effective rates of PER treatment at the different time points of evaluation were 88.7% (3 months), 79.1% (6 months), and 80.4% (12 months). With PER treatment, seizure freedom varied over time, with 61.3%, 71.0%, and 71.7% of patients at the 3-, 6-, and 12-month follow-ups, respectively. Among the etiologies of epilepsy, the effective rates of genetic etiology, structural etiology, and unknown etiology were generally above 50% at the 3-, 6-, and 12-month follow-ups. Among the epilepsy syndromes, the categories with higher treatment efficacy were self-limiting epilepsy with centrotemporal spikes (SeLECTs), self-limited epilepsy with autonomic seizures (SeLEAS), and childhood occipital visual epilepsy (COVE), with an effective rate of above 80%. Adverse events were documented in 22 patients (35.5%), but they were mild and tolerable. The most common adverse events comprised irritability, drowsiness, dizziness, and increased appetite. PER has favorable effectiveness and tolerability as initial monotherapy for children with newly diagnosed focal epilepsy, which could be a potential option for long-term medication in the treatment of focal epilepsy in children. The current study provided potential evidence for PER as initial monotherapy in children with focal epilepsy in clinical practice.
[Self-limited focal epilepsies of childhood].
Self-limited Focal Epilepsies of Childhood (SELFEs) are the most prevalent electroclinical syndromes in pediatric age, whose typical evolution, with age-dependent onset and remission, has allowed the ILAE Nosology and Definitions Working Group (2022) to define them as "Selflimited Focal Epilepsies of Childhood", thus establishing alert and exclusion criteria to standardize their diagnosis. These syndromes include: Self-limited Epilepsy with Centrotemporal Spikes (previously Rolandic Epilepsy), Self-limited Epilepsy with Autonomic Seizures (previously Panayiotopoulos Syndrome), Childhood Occipital Visual Epilepsy, (previously Gastaut Syndrome), and Photosensitive Occipital Lobe Epilepsy. Using the term "benign" to refer to them is no longer recommended, as this would ignore the comorbidities some individuals suffer. Also, the term "idiopathic" is now only used to refer to the syndromes classified as Idiopathic Generalized Epilepsies. Las Epilepsias Focales Autolimitadas de la Infancia (SELFEs - siglas en inglés) son los síndromes electroclínicos más prevalentes en edad pediátrica, cuya evolución típica, con inicio y remisión dependientes de la edad, ha permitido que el Grupo de Trabajo de Nosología y Definiciones de la ILAE (2022) las defina como "Epilepsias focales autolimitadas de la infancia", estableciendo así, criterios de alerta y exclusión para estandarizar su diagnóstico. Dentro de estos síndromes se incluyen: la Epilepsia Autolimitada con Espigas Centrotemporales (previamente Epilepsia Rolándica), Epilepsia Autolimitada con Crisis Autonómicas. (previamente Síndrome de Panayiotopoulos), Epilepsia Visual Occipital Infantil (previamente Síndrome de Gastaut), y Epilepsia Fotosensible del Lóbulo occipital. Ya no se recomienda utilizar el término "benignas" para referirse a ellas, ya que esto haría caso omiso de las comorbilidades que padecen algunos individuos. Asimismo, el término "idiopático" sólo se utiliza ahora para denominar a los síndromes clasificados como Epilepsias Generalizadas Idiopáticas.
Familial occipital lobe epilepsy associated with GABAA receptor variants.
Publicações recentes
Evolution into spike-and-wave activation in sleep in patients with self-limited focal epilepsies.
Clinical and Electrophysiological Characteristics and Prognosis of Childhood Occipital Visual Epilepsy in Light of Current ILAE Criteria.
Familial occipital lobe epilepsy associated with GABA(A) receptor variants.
[Self-limited focal epilepsies of childhood].
Effectiveness and tolerability of perampanel monotherapy in children with newly diagnosed focal epilepsy.
📚 EuropePMC1 artigos no totalmostrando 6
Evolution into spike-and-wave activation in sleep in patients with self-limited focal epilepsies.
SeizureClinical and Electrophysiological Characteristics and Prognosis of Childhood Occipital Visual Epilepsy in Light of Current ILAE Criteria.
Clinical EEG and neuroscienceFamilial occipital lobe epilepsy associated with GABAA receptor variants.
Seizure[Self-limited focal epilepsies of childhood].
MedicinaEffectiveness and tolerability of perampanel monotherapy in children with newly diagnosed focal epilepsy.
Frontiers in neurologyInternational League Against Epilepsy classification and definition of epilepsy syndromes with onset in childhood: Position paper by the ILAE Task Force on Nosology and Definitions.
EpilepsiaAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Epilepsia visual occipital da infância.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Epilepsia visual occipital da infância
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Evolution into spike-and-wave activation in sleep in patients with self-limited focal epilepsies.
- Clinical and Electrophysiological Characteristics and Prognosis of Childhood Occipital Visual Epilepsy in Light of Current ILAE Criteria.
- Effectiveness and tolerability of perampanel monotherapy in children with newly diagnosed focal epilepsy.
- [Self-limited focal epilepsies of childhood].
- Familial occipital lobe epilepsy associated with GABAA receptor variants.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:98816(Orphanet)
- MONDO:0020308(MONDO)
- Epilepsia(PCDT · Ministério da Saúde)
- GARD:19582(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Q5988868(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar