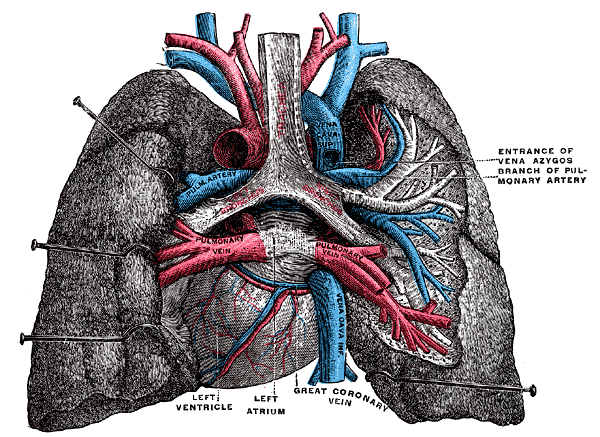
O coração é um órgão muscular presente nos humanos e em outros animais que bombeia o sangue através dos vasos sanguíneos do sistema circulatório. O sangue fornece ao corpo oxigénio e nutrientes e ajuda a eliminar resíduos metabólicos. Nos humanos, o coração situa-se na cavidade torácica entre os pulmões, num espaço denominado mediastino.
Introdução
O que você precisa saber de cara
Condição rara caracterizada pelo estreitamento das veias pulmonares sem causa aparente, dificultando o fluxo sanguíneo do pulmão para o coração. Pode levar à hipertensão pulmonar e insuficiência cardíaca.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Estenose primária da veia pulmonar
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
0 ensaios clínicos encontrados.
Publicações mais relevantes
Catheter and echocardiographic-focused management of primary pulmonary vein stenosis in premature infants: a single center 5-year experience.
We describe the outcomes of pulmonary vein stenosis treatment in a cohort of premature infants using an assertive percutaneous management strategy with echocardiography as the primary method of surveillance. This retrospective study included fifteen premature infants (median 24 weeks gestational age) that underwent pulmonary vein intervention from 2018-2023. The primary outcome was patient survival rate, and the secondary outcome was pulmonary vein preservation rate. The estimated patient survival was 100% and 89% at 1 and 2 years after diagnosis. The pulmonary vein preservation rate was 88% and 83% at 1 and 2 years. Patients received a median of 4 echocardiograms between each cardiac catheterization and an average of 1 CT scan for every 1.5 years of observation. Pulmonary vein stenosis can be successfully managed with a percutaneous approach to pulmonary vein rehabilitation using echocardiography for surveillance, even in extremely premature infants.
A Case of Incidentally Discovered Primary Pulmonary Vein Stenosis in an Adult.
Primary pulmonary vein stenosis (PPVS) in adults is rare and often incidentally detected on imaging. A 60-year-old man underwent chest CT for respiratory symptoms, revealing a localized reticulonodular opacity in the right upper lung field near the pulmonary hilum. Coronal and sagittal reconstructions demonstrated tortuous collateral veins bridging the right superior and inferior pulmonary veins. Mediastinal-window images confirmed severe stenosis of the proximal right superior pulmonary vein without evidence of external compression or congenital anomaly. As symptoms resolved spontaneously, conservative management was chosen. This case demonstrates that axial reticulonodular opacities can raise suspicion of PPVS, with multiplanar and mediastinal-window imaging enabling accurate diagnosis of this rare condition.
Insights into the molecular mechanism of pulmonary vein stenosis in pediatric patients with congenital heart disease.
Pediatric pulmonary vein stenosis (PVS) is associated with substantial morbidity and mortality for the subset of patients with recurrent or progressive disease. The molecular mechanisms underlying the development and trajectory of PVS remain unclear. This study characterizes the transcriptome of clinical and phenotypic subtypes of PVS. Bulk RNA sequencing analysis was performed on human pulmonary vein tissue samples obtained from surgical interventions for pediatric patients with PVS. Transcriptomic profiles were compared for primary versus postrepair PVS as well as aggressive versus nonaggressive clinical phenotypes. Principal component analysis was performed, the differential gene expression quantified, and pathway analysis conducted on the basis of Gene Ontology, Kyoto Encyclopedia of Genes and Genomes, and Reactome. When we compared aggressive (Agg) primary pulmonary vein stenosis (PPVS) versus nonaggressive (NonAgg) PPVS, differences were noted in the genes associated in extracellular matrix regulation and PIEZO1, a mechanosensitive receptor present in endothelial cells. In addition, there were notable changes in cardiac muscle contractility, calcium handling, respiratory and energy metabolism. These results point to a potential mechanism for aggressive PPVS phenotype, attributable to an overexpression of PIEOZ1 in response to elevated shear stress, subsequent activation of intracellular signaling pathways, and leading to reduced contractility and intracellular calcium transients within cardiomyocytes. These results suggests that aggressive PPVS phenotype may be driven by an increase in PIEZO1 expression and subsequent changes in extracellular matrix production. The clinical and therapeutic relevance of PIEZO1 warrant further investigation.
Long-term outcomes of individualised repair in patients with primary pulmonary vein stenosis.
Primary pulmonary vein stenosis is a rare congenital heart condition and carries a poor prognosis. Various surgical techniques have been introduced to treat primary pulmonary vein stenosis. However, there is no consensus on the optimal approach. This study aimed to evaluate the outcomes of surgical treatment of primary pulmonary vein stenosis, identify the risk factors for pulmonary vein restenosis and reintervention, and determine the optimal strategy for primary pulmonary vein stenosis repair. From December 2008 to December 2023, 64 patients with primary pulmonary vein stenosis undergoing surgical repair in our institution were included [non-sutureless group, n = 42; sutureless group, n = 22]. The Cox proportional hazard model was used to identify risk factors for pulmonary vein restenosis and pulmonary vein restenosis-related reintervention. There were three in-hospital deaths and one late death. The survival rates at 1, 5, and 15 years were 91.9%, 84.2%, and 69.8%, respectively, in the whole cohort. Compared with the non-sutureless group, the sutureless group did not significantly improve the long-term survival of primary pulmonary vein stenosis patients (P = 0.484). Pulmonary vein restenosis occurred in 15 patients. Multivariable analysis showed that Involvement of the left inferior pulmonary vein (P < 0.001) was the only independent risk factor for pulmonary vein restenosis, while sutureless repair (P = 0.037) was a protective factor. Pulmonary vein restenosis-related reintervention occurred in 12 patients. On multivariate analysis, three or four pulmonary veins involvement (P = 0.001) and preoperative severity score exceeding 5 (P = 0.050) were found to be independent risk factors associated with pulmonary vein restenosis-related reintervention; however, sutureless repair (P = 0.021) was a protective factor. Management of infants with primary pulmonary vein stenosis is challenging. Surgical repair of primary pulmonary vein stenosis can be safely achieved using different techniques, with similar long-term mortality. Compared with non-sutureless repair, sutureless repair was significantly associated with decreased pulmonary vein restenosis and decreased pulmonary vein restenosis-related reintervention, respectively. Preoperative severity score exceeding 5, 3, or 4 pulmonary veins involvement, and left inferior pulmonary vein involvement are independent risk factors for adverse outcomes.
Patient-specific 3D in vitro modeling and fluid dynamic analysis of primary pulmonary vein stenosis.
Primary pulmonary vein stenosis (PVS) is a rare congenital heart disease that proves to be a clinical challenge due to the rapidly progressive disease course and high rates of treatment complications. PVS intervention is frequently faced with in-stent restenosis and persistent disease progression despite initial venous recanalization with balloon angioplasty or stenting. Alterations in wall shear stress (WSS) have been previously associated with neointimal hyperplasia and venous stenosis underlying PVS progression. Thus, the development of patient-specific three-dimensional (3D) in vitro models is needed to further investigate the biomechanical outcomes of endovascular and surgical interventions. In this study, deidentified computed tomography images from three patients were segmented to generate perfusable phantom models of pulmonary veins before and after catheterization. These 3D reconstructions were 3D printed using a clear resin ink and used in a benchtop experimental setup. Computational fluid dynamic (CFD) analysis was performed on models in silico utilizing Doppler echocardiography data to represent the in vivo flow conditions at the inlets. Particle image velocimetry was conducted using the benchtop perfusion setup to analyze WSS and velocity profiles and the results were compared with those predicted by the CFD model. Our findings indicated areas of undesirable alterations in WSS before and after catheterization, in comparison with the published baseline levels in the healthy in vivo tissues that may lead to regional disease progression. The established patient-specific 3D in vitro models and the developed in vitro-in silico platform demonstrate great promise to refine interventional approaches and mitigate complications in treating patients with primary PVS.
Publicações recentes
Catheter and echocardiographic-focused management of primary pulmonary vein stenosis in premature infants: a single center 5-year experience.
A Case of Incidentally Discovered Primary Pulmonary Vein Stenosis in an Adult.
Insights into the molecular mechanism of pulmonary vein stenosis in pediatric patients with congenital heart disease.
Long-term outcomes of individualised repair in patients with primary pulmonary vein stenosis.
Patient-specific 3D in vitro modeling and fluid dynamic analysis of primary pulmonary vein stenosis.
📚 EuropePMC24 artigos no totalmostrando 22
Catheter and echocardiographic-focused management of primary pulmonary vein stenosis in premature infants: a single center 5-year experience.
Journal of perinatology : official journal of the California Perinatal AssociationA Case of Incidentally Discovered Primary Pulmonary Vein Stenosis in an Adult.
Journal of thoracic imagingInsights into the molecular mechanism of pulmonary vein stenosis in pediatric patients with congenital heart disease.
JTCVS openLong-term outcomes of individualised repair in patients with primary pulmonary vein stenosis.
Cardiology in the youngPatient-specific 3D in vitro modeling and fluid dynamic analysis of primary pulmonary vein stenosis.
Frontiers in cardiovascular medicineCombination Chemotherapy in Severe Pulmonary Vein Stenosis-A Case Series.
Children (Basel, Switzerland)Pulmonary vein stenosis: Anatomic considerations, surgical management, and outcomes.
The Journal of thoracic and cardiovascular surgeryRole of 3D reconstructed images in primary pulmonary vein stenosis.
Indian journal of thoracic and cardiovascular surgeryThoracic Multidetector Computed Tomography Angiography of Primary Pulmonary Vein Stenosis in Children: Evaluation of Characteristic Extravascular Findings.
Journal of thoracic imagingPrimary Pulmonary Vein Stenosis: A New Look at a Rare but Challenging Disease.
NeoReviewsClinical Outcomes, Predictors, and Surgical Management of Primary Pulmonary Vein Stenosis.
The Annals of thoracic surgeryPrimary pulmonary vein stenosis during infancy: state of the art review.
Journal of perinatology : official journal of the California Perinatal AssociationPrimary pulmonary vein stenosis among premature infants with single-vessel disease.
Journal of perinatology : official journal of the California Perinatal AssociationDouble-Orifice Mitral Valve Associated with Bicuspid Aortic Valve and Primary Pulmonary Vein Stenosis.
CASE (Philadelphia, Pa.)Commentary: Management outcomes of primary pulmonary vein stenosis: What we know now and what we can expect in the future.
The Journal of thoracic and cardiovascular surgeryManagement outcomes of primary pulmonary vein stenosis.
The Journal of thoracic and cardiovascular surgery[Primary Pulmonary Vein Stenosis Developed after Bidirectional Glenn Procedure;Report of Two Cases].
Kyobu geka. The Japanese journal of thoracic surgeryPrimary Pulmonary Vein Stenosis: Outcomes, Risk Factors, and Severity Score in a Multicentric Study.
The Annals of thoracic surgeryPulmonary Vein Stenosis in a Newborn: A Commonly Overlooked Diagnosis.
Case reports in cardiologyEvaluation of Primary Pulmonary Vein Stenosis in Children: Comparison of Radionuclide Perfusion Lung Scan and Angiography.
AJR. American journal of roentgenologyPrimary pulmonary vein stenosis: Can we expect different results?
The Journal of thoracic and cardiovascular surgerySurgical repair for primary pulmonary vein stenosis: Single-institution, midterm follow-up.
The Journal of thoracic and cardiovascular surgeryAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Estenose primária da veia pulmonar.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Estenose primária da veia pulmonar
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Catheter and echocardiographic-focused management of primary pulmonary vein stenosis in premature infants: a single center 5-year experience.Journal of perinatology : official journal of the California Perinatal Association· 2026· PMID 41862593mais citado
- A Case of Incidentally Discovered Primary Pulmonary Vein Stenosis in an Adult.
- Insights into the molecular mechanism of pulmonary vein stenosis in pediatric patients with congenital heart disease.
- Long-term outcomes of individualised repair in patients with primary pulmonary vein stenosis.
- Patient-specific 3D in vitro modeling and fluid dynamic analysis of primary pulmonary vein stenosis.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:642071(Orphanet)
- MONDO:0957433(MONDO)
- Busca completa no PubMed(PubMed)
- Artigo Wikipedia(Wikipedia)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar