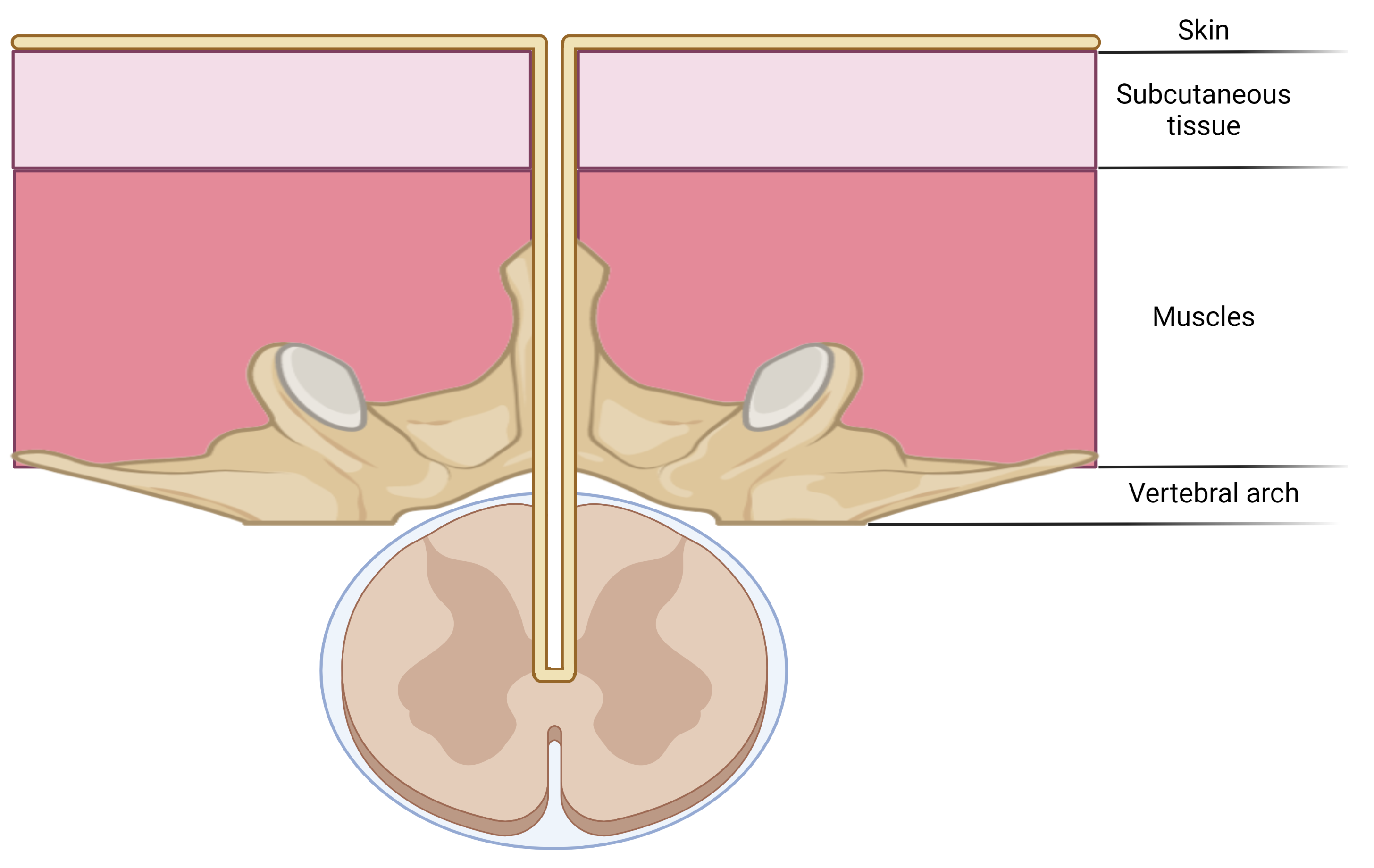
Malformação disráfica lipomatosa rara, caracterizada por fixação à superfície dorsal da medula espinal, mas sem se estender ao cone. Pode estar associada a outras caraterísticas, como um pedúnculo e anomalias ósseas vertebrais.
Introdução
O que você precisa saber de cara
Seio dérmico congênito é uma forma incomum de disrafismo craniano ou espinhal. Ocorre em 1 a cada 2500 nascidos vivos. Apresenta-se como uma indentação dérmica, localizada na linha média do neuroeixo e frequentemente se manifesta juntamente com infecção e déficit neurológico. O seio dérmico congênito forma-se devido a uma falha focal na disjunção entre o ectoderma cutâneo e o neuroectoderma durante a terceira à oitava semana de gestação. Tipicamente observado nas regiões lombar e lombossacra, o seio dérmico congênito pode ocorrer desde a região do násio e do occipital para baixo.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Lipoma espinhal dorsal
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Surgical treatment of a combined split cord malformation and spinal cord lipoma: illustrative case.
Split cord malformations (SCMs) are uncommon congenital anomalies that are usually detected in children, but can present in adulthood with signs and symptoms of spinal cord tethering. SCMs rarely occur in association with a lipoma and a defect in the posterior elements. A 37-year-old man presented with 6 months of new-onset leg weakness, urinary urgency, and reduced sensation in his feet. He developed pain radiating from his low back into his legs, worsened by bending forward and walking. Prior to this presentation, he had not noticed any symptoms. MRI revealed a congenital fusion from L2 to L4 with a type I SCM and a lipoma extending through a dorsal bony defect and terminating at the duplicated spinal cord. A posterior L2-4 lumbar laminectomy was performed to excise the bony spur, resect the spinal cord lipoma, and section the fatty filum terminale. Removal of the bony or fibrous septum and intradural lipoma and sectioning of the fatty filum terminale are required for effective detethering. Careful lipoma debulking, which can be facilitated with a CO2 laser, must be performed while developing surgical planes and minimizing tension on the tethered cord. https://thejns.org/doi/10.3171/CASE25691.
Prenatal Diagnosis to Postnatal Outcomes of Saccular Forms of Closed Spina Dysraphism: A Single Center Retrospective Study.
To describe prenatal imaging findings and postnatal outcomes in fetuses diagnosed with saccular forms of closed spinal dysraphism (CSD). This retrospective single-centre study included fetuses diagnosed with non-genetic, non-syndromic CSD between January 2018 and June 2023. Prenatal ultrasound and MRI findings were reviewed, with postnatal outcomes assessed in those managed expectantly, focusing on neurosurgical interventions, motor function, and urologic and bowel outcomes. Eighteen cases were identified; twelve opted for expectant management and had postnatal follow-up. The most common lesion was dysraphic spinal cord lipoma (10/18, 55.6%), followed by limited dorsal myeloschisis (3/18, 16.7%), myelocystocele (3/18, 16.7%) and meningocele (2/18, 11.0%). Chiari malformation and related brain abnormalities were absent at the time of diagnosis in all cases. Most fetuses (88.9%, 16/18) had a low-lying conus medullaris, and 70.6% (12/17) had a sac wall thickness ≥ 2 mm. Postnatally, 75% (9/12) underwent surgical detethering. At ≥ 30 months, all children could walk independently with or without orthoses. However, urologic complications were common in children age ≥ 48 months: 80% (4/5) required clean intermittent catheterization (CIC), 60% (3/5) had urinary incontinence, and 40% (2/5) experienced bowel incontinence. Prenatal imaging features at the lesion level are key for diagnosing CSD. While motor outcomes are favorable, urologic and bowel dysfunctions are frequent in postnatal life.
Posterior Extradural Spinal Tumor Extending From T3 to T6 Presenting With Paraplegia.
Extradural spinal tumors represent a large proportion of all spinal tumors and commonly present with spinal cord or nerve root compression. Although metastatic lesions are the most frequent, benign and less common entities may also occur. Prompt recognition is essential to prevent irreversible neurological compromise. We report the case of a 55-year-old male patient with diabetes mellitus who presented with paraplegia following three months of progressive dorsal pain and lower limb paresthesias. Neurological examination revealed flaccid paralysis of the lower limbs, sensory loss below the T5 dermatome, and sphincter dysfunction. Thoracic spine MRI demonstrated a posterior extradural mass extending from T3 to T6, compressing the spinal cord and associated with hematomyelia. The patient underwent urgent posterior decompression with wide laminectomy, complete tumor resection, and instrumented stabilization using transpedicular screws and titanium rods. Vancomycin powder was applied intraoperatively for infection prophylaxis. Postoperatively, the patient regained superficial sensation in the lower limbs and sphincter control within two months. At six months, neurological function improved to American Spinal Injury Association (ASIA) grade C, with muscle strength graded 3/5 at the hips and knees and 2/5 at the ankles according to the Medical Research Council (MRC) scale, allowing assisted ambulation through intensive physiotherapy. Histopathological examination confirmed a fibrolipoma with secondary ischemic and inflammatory changes and partial bone necrosis, without evidence of malignancy. Reporting such cases contributes to the understanding of the clinical spectrum of extradural spinal tumors and reinforces the need for prompt recognition and intervention.
Adult Type II diastematomyelia with tethered cord and associated spinal anomalies: A case report.
Spinal dysraphism consists a group of congenital anomalies due to defective neural tube closure, among which diastematomyelia or split cord malformation is rare. Split cord malformation is classified into Type I and Type II, with Type II being less common and often asymptomatic. These anomalies may coexist with various spinal anomalies, as tethered cord, neural lipoma, hemimyelocele, and dorsal dermal sinus, forming a complex spectrum. Adult presentations are particularly uncommon and usually incidental. We herein report a 23-year-old male with chronic low back pain and a congenital midline lumbar swelling. Neurological examination and routine investigations were unremarkable. Magnetic resonance imaging revealed Type II diastematomyelia with two hemicords within a single dural sac from L4 to L5, low-lying conus medullaris, hemimyelocele with neural lipoma at L5-S1, tethered cord with filum terminale lipoma extending to S3-S4, and a dorsal dermal sinus tract. Despite the radiological complexity, the patient remained neurologically intact. Neurosurgical intervention was advised; however, the patient chose conservative management with close follow-up. This case highlights a rare adult presentation of complex spinal dysraphism with minimal symptoms. While diastematomyelia Type II is typically diagnosed in childhood, adult cases are infrequent and often delayed. Magnetic resonance imaging is crucial for diagnosis, particularly in asymptomatic individuals with cutaneous markers. Though surgery is generally recommended to prevent neurological decline, conservative management may be appropriate in selected stable cases. This case emphasizes the need to consider spinal anomalies in adults with chronic back pain and the importance of multidisciplinary evaluation.
Are dorsal column deficits inevitable in intramedullary spine tumor resection?
The rate of dorsal column deficit after intramedullary spine tumor resection remains unknown. In a cohort of patients undergoing posterior intramedullary spinal tumor resection, the authors sought to 1) report the rate of dorsal column deficits, 2) report the rate of new motor deficits, and 3) determine risk factors and recovery characteristics for both deficits. A single-institution, retrospective cohort study of patients undergoing posterior intramedullary spinal cord tumor resection was performed from 2010 to 2020. Primary and metastatic cord tumors were included; cauda equina tumors and patients not undergoing midline myelotomy were excluded. Exposure variables included posterior midline myelotomy, tumor location within the spinal cord, spinal segment, tumor size, presence of cord edema on preoperative imaging, and complete/partial resection. The primary outcome was dorsal column deficit (new numbness/tingling, diminished fine touch, vibration, or 2-point discrimination, or balance/proprioceptive problems). Descriptive statistics were performed. Of 34 patients undergoing intramedullary tumor resection, the mean ± SD age was 44.4 ± 12.1 years and 55.9% were male. Histological analysis showed that 22 (64.7%) patients had ependymoma, 3 (8.8%) astrocytoma, 2 (5.9%) glioblastoma, 2 (5.9%) low-grade glioma, 2 (5.9%) lung adenocarcinoma, and 1 (2.9%) each of hemangioblastoma, lipoma, and necrosis possible neoplasm. Tumor locations were cervical in 17 (50.0%) patients, thoracic in 15 (44.1%), and thoracolumbar/conus in 2 (5.9%). Complete resection was achieved in 19 (55.9%) patients. At presentation, 26 (76.5%) patients had dorsal column deficits and 17 (50%) had motor deficits. Deficits worsened in 17/26 patients with preoperative motor deficits, remained the same in 9, and improved in 0. In 8 patients without preoperative dorsal column deficits, 7 had new dorsal column deficit and 1 had none. A postoperative dorsal column deficit was seen in 33/34 (97%) patients. At the most recent follow-up, 6/33 (18%) patients had improvement in dorsal column deficits and 27/33 (82%) had stable deficits. Postoperative dorsal column deficits occurred in 97% patients who underwent midline myelotomy for intramedullary tumor resection. Dorsal column deficits improved in 18% yet remained stable in the remaining 82%. Motor deficits improved in only 12% and remained stable/worsened in 88%. These results highlight the high rate of dorsal column deficits in patients requiring midline myelotomy for resection of intramedullary tumors.
Publicações recentes
Top-down descending modulation of dorsal spinal excitatory transmission from the insular cortex.
Characterisation of MRI Appearance of the Spinal Cord Syrinx in the Whole Spectrum of Chiari Malformation.
Nanoscale magnesium hydride alleviates hypoxia-induced myelination deficits in zebrafish.
High-Grade Pancreatic Neuroendocrine Carcinoma Presenting as Dorsal Spinal Cord Compression: A Diagnostic and Surgical Challenge for the Orthopedic Oncologist.
FL/FLT3 signaling enhances mechanical pain hypersensitivity through Interleukin-1 beta (IL-1β) in male mice.
📚 EuropePMCmostrando 56
Surgical treatment of a combined split cord malformation and spinal cord lipoma: illustrative case.
Journal of neurosurgery. Case lessonsPrenatal Diagnosis to Postnatal Outcomes of Saccular Forms of Closed Spina Dysraphism: A Single Center Retrospective Study.
Prenatal diagnosisPosterior Extradural Spinal Tumor Extending From T3 to T6 Presenting With Paraplegia.
CureusAdult Type II diastematomyelia with tethered cord and associated spinal anomalies: A case report.
Radiology case reportsAre dorsal column deficits inevitable in intramedullary spine tumor resection?
Journal of neurosurgery. SpineNeurosurgical Management and Follow-up of Pediatric Lumbosacral Lipomas: A Single-Center Experience with 28 Patients.
Turkish neurosurgeryEffectiveness of conus lipoma surgery-a case series.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgerySaccular Limited Dorsal Myeloschisis: A Distinct Prenatal Entity.
Fetal diagnosis and therapyA Case of Surgically Treated Adult Split Cord Malformation Type 2 with Tethered Cord Syndrome.
NMC case report journalNeurosurgical strategy based on the type of occult spinal dysraphism in omphalocele-exstrophy-imperforate anus-spinal defects complex: A review of 10 cases.
Surgical neurology internationalA rare coexistence of a non-dysraphic intradural lipoma and a cyst in the lumbar spine - A case report and literature review.
International journal of surgery case reportsComplex lumbosacral spinal cord lipomas: A longitudinal study on outcomes from a Singapore children's hospital.
Journal of clinical neuroscience : official journal of the Neurosurgical Society of AustralasiaPreoperative interactive virtual simulation applying three-dimensional multifusion images using a haptic device for lumbosacral lipoma.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryLumbosacral lipoma in childhood, how strong is the evidence base? A systematic review.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgerySpinal Dysraphism Presenting as Neuropathic Ulcers: A Case Report of a Delayed Diagnosis.
Case reports in dermatologyThe Current Status of the Surgical Management of Complex Spinal Cord Lipomas: Still Navigating the Labyrinth?
Advances and technical standards in neurosurgeryA Presenile Patient with Filar Lipoma Who Developed Tethered Spinal Cord Syndrome Triggered by Lumbar Canal Stenosis.
NMC case report journalNon Dysraphic Intramedullary Spinal Cord Lipoma.
Neurology IndiaLimited dorsal myeloschisis without extradural stalk continuity to coexisting congenital dermal sinus.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryLimited dorsal myeloschisis involving one hemicord of a split cord malformation - a "hemi-LDM".
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgerySelective dorsal rhizotomy for spasticity associated with spinal cord injury sustained during surgery for spinal lipomatous malformation: A case report.
Journal of pediatric rehabilitation medicineUnusual presentation of a giant thoracic spinal cord lipoma.
Spinal cord series and casesRadical resection of lumbosacral lipomas in children: the Great Ormond Street Hospital experience.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryPreventive Surgery for Asymptomatic Spinal Lipomas in Children.
Turkish neurosurgerySurgical histopathology of a filar anomaly as an additional tethering element associated with closed spinal dysraphism of primary neurulation failure.
Surgical neurology internationalNon-dysraphic extramedullary intradural spinal lipoma with neurocutaneous melanocytosis.
British journal of neurosurgeryPatterns of spinal cord malformation in cloacal exstrophy.
Journal of neurosurgery. PediatricsDoes conus morphology have implications for outcome in lumbosacral lipoma?
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryUsefulness of external anal sphincter EMG recording for intraoperative neuromonitoring of the sacral roots-a prospective study in dorsal rhizotomy.
Acta neurochirurgicaNeurocutaneous melanocytosis (melanosis).
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryEarly de-tethering: analysis of urological and clinical consequences in a series of 40 children.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryLimited dorsal myeloschisis with a contiguous stalk to human tail-like cutaneous appendage, associated with a lipoma of conus medullaris: A case report.
International journal of surgery case reportsSacral Extradural Angiolipoma Associated with Tight Filum Terminale and Spina Bifida Coexisting with Spinal Arteriovenous Fistula.
World neurosurgeryPerspectives on Spinal Dysraphism : Past, Present, and Future.
Journal of Korean Neurosurgical SocietySurgical Management of Complex Spinal Cord Lipomas : A New Perspective.
Journal of Korean Neurosurgical SocietyLong-term urological outcomes of spinal lipoma after prophylactic untethering in infancy: real-world outcomes by lipoma anatomy.
Spinal cordIntradural Lipoma at the Craniocervical Junction Presenting with Progressing Hemiparesis: A Case Report.
Case reports in neurologyAcute presentations of intradural lipomas: case reports and a review of the literature.
BMC neurologyRadical excision of lumbosacral lipoma: an early experience of "followers".
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgerySurgical management of complex spinal cord lipomas: how, why, and when to operate. A review.
Journal of neurosurgery. PediatricsComplex spinal dysraphism: myelomenigocele associated with dorsal bony spur, split cord malformation type I, syringomyelia, lipoma and tethered cord.
British journal of neurosurgeryEpendyma-Lined Canal with Surrounding Neuroglial Tissues in Lumbosacral Lipomatous Malformations: Relationship with Retained Medullary Cord.
Pediatric neurosurgeryBony and Cartilaginous Tissues in Lumbosacral Lipomas.
Pediatric neurosurgerySurgical Outcomes of Pediatric Patients with Asymptomatic Tethered Cord Syndrome.
Asian spine journalSplit cord malformation type 1 with two hemicord lesions.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryA case of junctional neural tube defect associated with a lipoma of the filum terminale: a new subtype of junctional neural tube defect?
Journal of neurosurgery. PediatricsNeurosurgical pathology of limited dorsal myeloschisis.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryNondysraphic cervicomedullary intramedullary lipoma.
Journal of craniovertebral junction & spinePrenatal sonographic diagnosis of nondysraphic intramedullary lipomas: A case report.
Journal of clinical ultrasound : JCULipomyelomeningocele for the urologist: Should we view it the same as myelomeningocele?
Journal of pediatric urologyNoncontiguous Double Spinal Lipoma with Tethered Cord and Polydactyly: Two Different Embryological Events in One Patient.
Journal of pediatric neurosciencesThe Rare Association of Spina Bifida and Extrarenal Wilms Tumor: A Case Report and Review of the Literature.
World neurosurgeryDuplicated filum terminale in non-split cord malformations: An underrecognized cause for treatment failure in tethered cord syndrome.
The journal of spinal cord medicineNondysraphic Intramedullary Cervical Cord Lipoma with Exophytic Component: Case Report.
Journal of neurological surgery reports[Human tail: rare lesion with occult spinal dysraphism].
Cirugia pediatrica : organo oficial de la Sociedad Espanola de Cirugia PediatricaSpinal cord detethering procedures in children: a 5 year retrospective cohort study of the early post-operative course.
Journal of clinical neuroscience : official journal of the Neurosurgical Society of AustralasiaAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Lipoma espinhal dorsal.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Lipoma espinhal dorsal
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Surgical treatment of a combined split cord malformation and spinal cord lipoma: illustrative case.
- Prenatal Diagnosis to Postnatal Outcomes of Saccular Forms of Closed Spina Dysraphism: A Single Center Retrospective Study.
- Posterior Extradural Spinal Tumor Extending From T3 to T6 Presenting With Paraplegia.
- Adult Type II diastematomyelia with tethered cord and associated spinal anomalies: A case report.
- Are dorsal column deficits inevitable in intramedullary spine tumor resection?
- Top-down descending modulation of dorsal spinal excitatory transmission from the insular cortex.
- Characterisation of MRI Appearance of the Spinal Cord Syrinx in the Whole Spectrum of Chiari Malformation.
- Nanoscale magnesium hydride alleviates hypoxia-induced myelination deficits in zebrafish.
- High-Grade Pancreatic Neuroendocrine Carcinoma Presenting as Dorsal Spinal Cord Compression: A Diagnostic and Surgical Challenge for the Orthopedic Oncologist.
- FL/FLT3 signaling enhances mechanical pain hypersensitivity through Interleukin-1 beta (IL-1β) in male mice.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:645362(Orphanet)
- MONDO:0958349(MONDO)
- Busca completa no PubMed(PubMed)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar