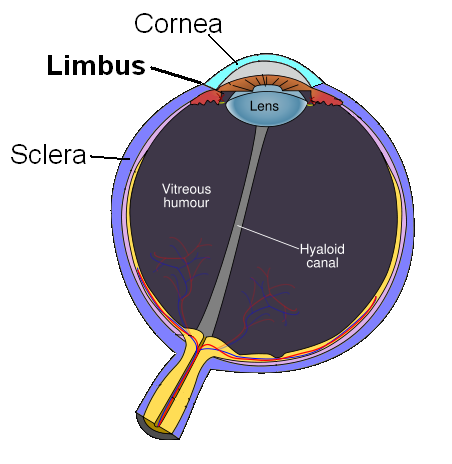
Uma lente de contato (português brasileiro) ou lente de contacto (português europeu) é uma lente oftálmica corretiva, cosmética, corretivo-cosmética ou terapêutica utilizada sobre a córnea do olho. As lentes de contato modernas foram inventadas pelo químico checo Otto Wichterle, que também inventou o primeiro gel usado para a produção das lentes.
Introdução
O que você precisa saber de cara
Inflamação crônica da conjuntiva e córnea superior, com dor, sensação de corpo estranho e visão turva. Caracteriza-se por lesões epiteliais em "ponto de interrogação" no limbo e conjuntiva.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Ceratoconjuntivite límbica superior
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
3 ensaios clínicos encontrados.
Publicações mais relevantes
Superior Limbic Keratoconjunctivitis: Pathophysiology, Diagnosis, and Advances in Therapeutic Strategies.
Superior limbic keratoconjunctivitis (SLK) is a chronic inflammatory disorder of the ocular surface, primarily affecting the superior bulbar and palpebral conjunctiva. It predominantly occurs in middle-aged women and is associated with conditions, such as dry eye disease, thyroid eye disease, and ocular graft-versus-host disease. Although its exact etiology remains unclear, mechanical microtrauma and tear film instability are key contributing factors. Given its relapsing-remitting nature, early diagnosis and appropriate management are essential to prevent chronic ocular discomfort and visual disturbances. To provide a comprehensive review of the pathophysiology, clinical presentation, diagnosis, and management strategies for SLK, emphasizing the latest advances in medical and surgical treatment. A literature review was conducted to analyze current evidence on the mechanisms, diagnosis, and treatment of SLK. The therapeutic approaches were categorized into medical, mechanical, and surgical interventions, highlighting their indications, efficacy, and limitations. Emerging treatments and their potential role in SLK management were also evaluated. SLK is an often underdiagnosed yet significant ocular surface disorder that requires a customized treatment approach. The management of SLK focuses on minimizing mechanical friction and controlling inflammation. In mild cases, patients typically respond well to ocular lubricants and mast cell stabilizers. For moderate cases, treatment may involve punctal occlusion and immunomodulatory therapy. Severe or refractory cases can benefit from supratarsal corticosteroid injections, scleral lenses, or surgical interventions such as conjunctival resection or thermal cauterization. While the overall prognosis is generally favorable, recurrence is common. Therefore, long-term follow-up is essential to optimize treatment outcomes and reduce the likelihood of relapses.
Differential Tear Lipid Metabolomics Signatures Discriminate Superior Limbic Keratoconjunctivitis From Dry Eye Disease.
Superior limbic keratoconjunctivitis (SLK) and dry eye disease (DED) exhibit similar clinical manifestations, complicating diagnosis. We aimed to compare tear metabolomic profiles and secretory phospholipase A2 (sPLA2) levels in patients with SLK versus patients with DED. We established a cross-sectional study involving 56 subjects: 20 patients with SLK, 21 patients with DED, and 15 matched healthy controls (solely for measuring sPLA2). Tear fluids collected via Schirmer strips underwent liquid chromatography with tandem mass spectrometry metabolomic analysis. Metabolites were quantitatively analyzed and matched to metabolic pathways and biomarkers. Metabolic differences between patients with SLK and patients with DED were identified through multivariate statistical analysis. Western blot measured the content of sPLA2 in tears of the three groups. Tear analysis annotated 274 metabolites. Twenty-three metabolites showed significant differences (P < 0.05) between the 2 groups, comprising 20 increased and 3 decreased in SLK. Top differential metabolic pathways were glycerophospholipid, alpha-linolenic acid, and linoleic acid metabolism. Receiver operating characteristic (ROC) analysis showed that five metabolites could be considered as potential biomarkers for distinguishing SLK from DED. Tears PLA2 was significantly higher in SLK than healthy controls (p < 0.05), but without difference between SLK and DED. The study revealed distinct metabolomic profiles in SLK versus DED tears, with notable changes in glycerophospholipid metabolism and elevated sPLA2 levels in SLK. Tear metabolomics distinguishes SLK from DED at the molecular level through dysregulated glycerophospholipid metabolism. In SLK, compared with controls, this dysregulation coincides with elevated sPLA2, an enzyme hydrolyzing glycerophospholipids, indicating lipid-driven inflammation.
Neuromodulation with Botulinum Toxin in Eyelid-Associated Ocular Surface Disease.
Ocular surface disease (OSD) encompasses a range of conditions that not only include the well-described dry eye disease (DED) components - such as hyperosmolarity, inflammation, ocular surface damage, and neurosensory compromise - but also eyelid-related disorders. These can stem from anatomical abnormalities or as consequences of DED, leading to various mechanical and inflammatory issues. These may include friction between the eyelids and the globe; irregular blink mechanics; and incomplete protection or even frank exposure of the ocular surface. Eyelid-associated ocular surface disease (EAOSD) includes conditions such as superior limbic keratoconjunctivitis, orbicularis oculi spasm (Jumping Orbicularis Sign), lid wiper epitheliopathy, and tight eyelid syndrome. Botulinum toxin, produced by the bacterium Clostridium botulinum, works by blocking the release of acetylcholine at the neuromuscular junction, leading to temporary muscle weakening. When mindfully injected into the orbicularis oculi, frontalis, or tarsal plate, botulinum toxin may reduce muscle tension around the eyelids, which improves eyelid tone and anatomic apposition between the eyelid and ocular surface tissues. Botulinum toxin can also be used to address abnormal blink patterns, incomplete blinking, nocturnal lid seal insufficiency, and lagophthalmos. Such interventions may alleviate symptoms associated with EAOSD. This paper examines the applications of botulinum toxin in the treatment of EAOSD. Other applications of botulinum toxin for addressing photophobia and excess trigeminal nerve tone are separately addressable topics.
Insights Into the Pathophysiology of Superior Limbic Keratoconjunctivitis in Chronic Ocular Graft-Versus-Host Disease.
Superior limbic keratoconjunctivitis (SLK) is a chronic inflammatory ocular surface disorder affecting the superior conjunctiva and limbus. Its pathogenesis entails a vicious cycle of microtrauma and inflammation. Besides its well-known association with thyroid disorders, SLK has also been associated with systemic conditions involving severe ocular surface disease. One condition that can secondarily develop SLK is ocular graft-versus-host disease (oGVHD). Ocular graft-versus-host disease, a complication of allogeneic hematopoietic stem-cell transplantation, is a pan-ocular surface disease that can lead to severe ocular complications and vision loss. Importantly, the occurrence of SLK in the setting of oGVHD is a marker of an augmented ocular surface distress that requires immediate aggressive management to prevent irreversible ocular surface damage, notably limbal stem-cell deficiency. Treatment of SLK in oGVHD includes aggressive lubrication, anti-inflammatory drops, serum/plasma drops, and large diameter contact lenses. In particular, scleral contact lenses are currently the most effective long-term treatment for SLK in oGVHD and can significantly reduce the risk of irreversible loss of vision. Of note, conjunctival resection or destruction (e.g., cauterization) is not recommended for treatment of SLK in ocular graft-versus-host disease. This review examines the pathophysiology and treatment modalities for SLK in oGVHD aimed at improving long-term outcomes.
A novel large diameter rigid gas-permeable corneal contact lens design for keratoconus.
To assess the fitting process and clinical feasibility of a novel large diameter rigid gas-permeable (RGP) corneal contact lens (CL) presenting regular or reverse geometry for managing keratoconus (KC). The lens was designed to rest on the peripheral cornea and vault over the cone, aiming to enhance visual quality, comfort, and corneal physiology. 32 KC patients across all severity stages, including central, paracentral and peripheral cones enrolled. Lens parameters were customized from corneal measurements obtained via Oculus Pentacam HR tomography, mainly based on sagittal height and accounting for adequate tear film clearance. Visual acuity (VA), contrast sensitivity (CS), ocular complications, and user satisfaction were evaluated at baseline, and at one week and three months of lens wear. Twenty-four patients (41 eyes) were fitted and completed the 3-month follow-up (median age of 28.5 years, 9 females). A median of 2 trial lenses per eye (interquartile range of 4.5) were needed during the fitting process. Significant improvements in median VA (baseline: 0.32 logMAR; three months: 0.01 logMAR; p = 0.002) and CS (p < 0.001 at all frequencies) were observed compared to baseline values. Ocular complications remained below clinical significance, with superior limbic keratoconjunctivitis showing significant reduction over time (p < 0.001). Patient satisfaction was high, with a median daily lens wear of 9.5 h. Most users (79.2%) reported consistent comfort with their CLs. The novel large diameter RGP corneal CL demonstrated comparable efficacy to existing RGP CL designs, offering high levels of comfort and improved vision with minimal ocular complications. The conjunctiva is a transparent, thin mucous membrane covering the sclera. This structure extends from the limbus, or the perimeter of the cornea, and covers both the sclera, where it is termed the "bulbar conjunctiva," and the posterior eyelid surfaces, where it is called the "palpebral conjunctiva." Keratoconjunctivitis is an inflammatory condition that affects both the superficial cornea and the conjunctiva. The term is derived from the words "keratitis," which refers to superficial corneal inflammation, and "conjunctivitis," which denotes conjunctival involvement. This ocular condition can arise from an expansive list of etiologies, including viral, bacterial, autoimmune, toxic, or allergic causes. Keratoconjunctivitis often results in significant discomfort and potential vision impairment. Viruses, particularly adenoviruses, are among the most common culprits, followed by bacterial and fungal pathogens in certain cases. Allergic keratoconjunctivitis, often associated with environmental allergens, as well as dry eye-related forms linked to tear film dysfunction, also contributes significantly to the condition. Autoimmune diseases such as Sjögren syndrome can further complicate the clinical spectrum of this disease by disrupting the ocular surface. Epidemiologically, keratoconjunctivitis is widespread, with varying prevalence depending on the subtype and geographic location. Viral keratoconjunctivitis, for instance, tends to occur in outbreaks, especially in crowded environments like schools or workplaces. Conversely, dry eye-related keratoconjunctivitis predominantly affects older populations, particularly postmenopausal women, due to hormonal changes affecting tear production. Patients with keratoconjunctivitis often present with a constellation of symptoms, including redness, photophobia, blurred vision, excessive tearing or dryness, and a gritty or foreign body sensation in the eye. In more severe cases, patients may report sharp pain, mucopurulent discharge, or difficulty keeping the eye open due to irritation. On examination, clinicians may note conjunctival hyperemia, corneal epithelial defects, lid swelling, or papillary reactions on the tarsal conjunctiva. These signs, combined with the patient's history, aid in differentiating the various subtypes of keratoconjunctivitis. A thorough investigation is essential to establish a definitive diagnosis. Evaluation typically includes a detailed clinical history, slit-lamp biomicroscopy, and, where indicated, laboratory tests such as viral cultures, polymerase chain reaction (PCR) testing for adenoviruses, or conjunctival scrapings for cytology and bacterial cultures. Tear film assessments, including the Schirmer test and tear break-up time (TBUT), are valuable in diagnosing dry eye-associated keratoconjunctivitis. Advanced imaging techniques, such as anterior segment optical coherence tomography (AS-OCT) and confocal microscopy, can provide further insights into the structural integrity of the cornea and conjunctiva. Management of keratoconjunctivitis highly depends on the underlying etiology. Viral keratoconjunctivitis typically requires supportive care, including artificial tears and cold compresses, as antiviral medications are rarely indicated. In contrast, bacterial keratoconjunctivitis demands prompt antibiotic therapy to prevent complications, such as corneal ulcers. Allergic keratoconjunctivitis often responds well to antihistamines, mast cell stabilizers, and allergen avoidance strategies. For dry eye-related cases, artificial tears, punctal plugs, and, in severe cases, immunomodulatory agents like cyclosporine can provide significant relief. Corticosteroids may be cautiously used in autoimmune-related keratoconjunctivitis, but their prolonged use must be carefully monitored due to the risk of cataracts and glaucoma. Looking to the future, advancements in the understanding of ocular surface inflammation and tear film dynamics are paving the way for more targeted therapies. Emerging treatments, such as biologic agents targeting specific inflammatory pathways, alongside gene therapies, hold promise in addressing refractory cases. Additionally, innovations in diagnostic tools, including point-of-care tests for tear biomarkers and artificial intelligence-driven imaging technologies, are expected to enhance early detection and personalized management of keratoconjunctivitis. Overall, keratoconjunctivitis is a complex and multifaceted condition requiring a nuanced approach to diagnosis and management. By integrating current evidence-based practices with emerging therapeutic and diagnostic advancements, healthcare providers can significantly improve outcomes for individuals affected by this debilitating condition. This activity will focus on more well-known entities causing combined keratoconjunctivitis. Specifically, this activity will discuss the entities known as epidemic keratoconjunctivitis (EKC), vernal keratoconjunctivitis (VKC), superior limbic keratoconjunctivitis (SLK), and keratoconjunctivitis sicca.
Publicações recentes
Differential Tear Lipid Metabolomics Signatures Discriminate Superior Limbic Keratoconjunctivitis From Dry Eye Disease.
Neuromodulation with Botulinum Toxin in Eyelid-Associated Ocular Surface Disease.
Insights Into the Pathophysiology of Superior Limbic Keratoconjunctivitis in Chronic Ocular Graft-Versus-Host Disease.
Superior Limbic Keratoconjunctivitis: Pathophysiology, Diagnosis, and Advances in Therapeutic Strategies.
A novel large diameter rigid gas-permeable corneal contact lens design for keratoconus.
📚 EuropePMC81 artigos no totalmostrando 35
Differential Tear Lipid Metabolomics Signatures Discriminate Superior Limbic Keratoconjunctivitis From Dry Eye Disease.
Translational vision science & technologyNeuromodulation with Botulinum Toxin in Eyelid-Associated Ocular Surface Disease.
Journal of visualized experiments : JoVEInsights Into the Pathophysiology of Superior Limbic Keratoconjunctivitis in Chronic Ocular Graft-Versus-Host Disease.
Eye & contact lensSuperior Limbic Keratoconjunctivitis: Pathophysiology, Diagnosis, and Advances in Therapeutic Strategies.
Seminars in ophthalmologyA novel large diameter rigid gas-permeable corneal contact lens design for keratoconus.
Journal of optometryTargeted metabolomic analysis of serum free fatty acids: Lipidomics disturbance in patients with superior limbic keratoconjunctivitis.
Experimental eye researchConjunctival Chalasis Should Not be Overlooked: Investigation Into Postoperative Ocular Surface Changes in Involutional Blepharoptosis.
The Journal of craniofacial surgeryEffect of Punctal Occlusion on Blinks in Eyes with Severe Aqueous Deficient Dry Eye.
Diagnostics (Basel, Switzerland)Combination of Bandage Contact Lens and Autologous Serum Eye Drop for the Treatment of Superior Limbic Keratoconjunctivitis.
Clinical optometrySuperior limbic keratoconjunctivitis: Update on pathophysiology and management.
The ocular surfaceRisk factors for development of superior limbic keratoconjunctivitis in thyroid eye disease in Japanese.
Graefe's archive for clinical and experimental ophthalmology = Albrecht von Graefes Archiv fur klinische und experimentelle OphthalmologieChanges in Dry Eye Status after Steroid Pulse and Orbital Radiation Therapies in Active Thyroid Eye Disease.
Journal of clinical medicineFinite Element Analysis of Cornea and Lid Wiper during Blink, with and without Contact Lens.
Journal of ophthalmologyEffects of meibomian gland dysfunction and aqueous deficiency on friction-related disease.
The ocular surfaceSuperior limbic keratoconjunctivitis following ptosis repair.
Canadian journal of ophthalmology. Journal canadien d'ophtalmologieMetabolomic Alterations in the Tear Fluids of Patients With Superior Limbic Keratoconjunctivitis.
Frontiers in medicineRecharacterization of superior limbic keratoconjunctivitis via a subdividing grading method in 236 Chinese patients.
Graefe's archive for clinical and experimental ophthalmology = Albrecht von Graefes Archiv fur klinische und experimentelle OphthalmologieTopical steroids to the superior bulbar conjunctiva for the treatment of superior limbic keratoconjunctivitis (SLK).
The ocular surfaceChanges in Eyelid Pressure and Dry Eye Status after Orbital Decompression in Thyroid Eye Disease.
Journal of clinical medicineSuperior limbic keratoconjunctivitis: a comprehensive review.
Survey of ophthalmologyTear film break-up patterns in thyroid eye disease.
Scientific reportsNocardia keratitis mimicking superior limbic keratoconjunctivitis and herpes simplex virus.
American journal of ophthalmology case reportsNatural history of inflammatory and non-inflammatory dry eye in thyroid eye disease.
Orbit (Amsterdam, Netherlands)[Complications associated with the use of soft contact lenses].
SemergenTear cytokine profiling in patients with superior limbic keratoconjunctivitis who underwent medical treatment or in conjunction with surgical management.
The British journal of ophthalmologyEyelid metrics assessment in patients with chronic ocular graft versus-host disease.
The ocular surfaceInfluence of Meibomian Gland Dysfunction and Friction-Related Disease on the Severity of Dry Eye.
OphthalmologyHigh Inflammatory Infiltrate Correlates With Poor Symptomatic Improvement After Surgical Treatment for Superior Limbic Keratoconjunctivitis.
CorneaClinical Severity Classification using Automated Conjunctival Hyperemia Analysis Software in Patients with Superior Limbic Keratoconjunctivitis.
Current eye researchTFOS DEWS II pathophysiology report.
The ocular surfaceEfficacy and safety of 0.1% lodoxamide for the long-term treatment of superior limbic keratoconjunctivitis.
International ophthalmologySuperior Limbic Keratoconjunctivitis-like Inflammation in Patients with Chronic Graft-Versus-Host Disease.
The ocular surfaceStem Cell Factor and Thymic Stromal Lymphopoietin Overexpression With Correlation to Mast Cells in Superior Limbic Keratoconjunctivitis.
CorneaExtensive superior limbic keratoconjunctivitis in Graves' disease: case report and mini-review of the literature.
Clinical ophthalmology (Auckland, N.Z.)Autologous serum eye drops for the treatment of ocular surface disease.
Eye & contact lensAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Ceratoconjuntivite límbica superior.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Ceratoconjuntivite límbica superior
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Superior Limbic Keratoconjunctivitis: Pathophysiology, Diagnosis, and Advances in Therapeutic Strategies.
- Differential Tear Lipid Metabolomics Signatures Discriminate Superior Limbic Keratoconjunctivitis From Dry Eye Disease.
- Neuromodulation with Botulinum Toxin in Eyelid-Associated Ocular Surface Disease.
- Insights Into the Pathophysiology of Superior Limbic Keratoconjunctivitis in Chronic Ocular Graft-Versus-Host Disease.
- A novel large diameter rigid gas-permeable corneal contact lens design for keratoconus.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:88633(Orphanet)
- MONDO:0019504(MONDO)
- GARD:10940(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Q7643645(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar