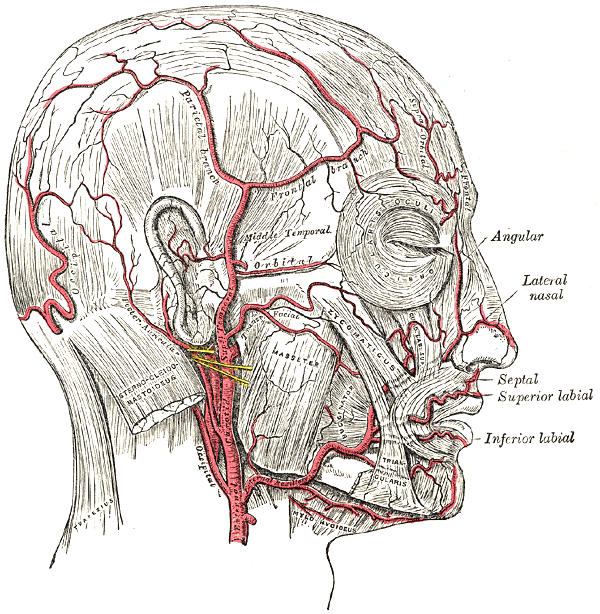
É uma inflamação dos vasos sanguíneos grandes, que atinge principalmente as artérias que saem do arco da aorta e, em especial, os ramos das artérias carótidas que ficam fora do crânio.
Introdução
O que você precisa saber de cara
É uma inflamação dos vasos sanguíneos grandes, que atinge principalmente as artérias que saem do arco da aorta e, em especial, os ramos das artérias carótidas que ficam fora do crânio.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 29 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 72 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
4 genes identificados com associação a esta condição. Padrão de herança: Multigenic/multifactorial.
Antigen-presenting major histocompatibility complex class I (MHCI) molecule. In complex with B2M/beta 2 microglobulin displays primarily viral and tumor-derived peptides on antigen-presenting cells for recognition by alpha-beta T cell receptor (TCR) on HLA-B-restricted CD8-positive T cells, guiding antigen-specific T cell immune response to eliminate infected or transformed cells (PubMed:23209413, PubMed:25808313, PubMed:29531227, PubMed:9620674). May also present self-peptides derived from the
Cell membraneEndoplasmic reticulum membrane
Stevens-Johnson syndrome
A rare blistering mucocutaneous disease that share clinical and histopathologic features with toxic epidermal necrolysis. Both disorders are characterized by high fever, malaise, and a rapidly developing blistering exanthema of macules and target-like lesions accompanied by mucosal involvement. Stevens-Johnson syndrome is a milder disease characterized by destruction and detachment of the skin epithelium and mucous membranes involving less than 10% of the body surface area. Ocular symptoms include ulcerative conjunctivitis, keratitis, iritis, uveitis and sometimes blindness. It can be caused by a severe adverse reaction to particular types of medication, although Mycoplasma infections may induce some cases.
Catalyzes the post-translational formation of 4-hydroxyproline in -Xaa-Pro-Gly- sequences in collagens and other proteins
Endoplasmic reticulum lumen
Myopia 25, autosomal dominant
A refractive error of the eye, in which parallel rays from a distant object come to focus in front of the retina, vision being better for near objects than for far.
A beta chain of antigen-presenting major histocompatibility complex class II (MHCII) molecule. In complex with the alpha chain HLA-DRA, displays antigenic peptides on professional antigen presenting cells (APCs) for recognition by alpha-beta T cell receptor (TCR) on HLA-DRB1-restricted CD4-positive T cells. This guides antigen-specific T-helper effector functions, both antibody-mediated immune response and macrophage activation, to ultimately eliminate the infectious agents and transformed cells
Cell membraneEndoplasmic reticulum membraneLysosome membraneLate endosome membraneAutolysosome membrane
Acts as a negative regulator of T-cell receptor (TCR) signaling by direct dephosphorylation of the Src family kinases LCK and FYN, ITAMs of the TCRz/CD3 complex, as well as ZAP70, VAV, VCP and other key signaling molecules (PubMed:16461343, PubMed:18056643). Associates with and probably dephosphorylates CBL. Dephosphorylates LCK at its activating 'Tyr-394' residue (PubMed:21719704). Dephosphorylates ZAP70 at its activating 'Tyr-493' residue (PubMed:16461343). Dephosphorylates the immune system a
Cytoplasm
Systemic lupus erythematosus
A chronic, relapsing, inflammatory, and often febrile multisystemic disorder of connective tissue, characterized principally by involvement of the skin, joints, kidneys and serosal membranes. It is of unknown etiology, but is thought to represent a failure of the regulatory mechanisms of the autoimmune system. The disease is marked by a wide range of system dysfunctions, an elevated erythrocyte sedimentation rate, and the formation of LE cells in the blood or bone marrow.
Medicamentos aprovados (FDA)
2 medicamentos encontrados nos registros da FDA americana.
Variantes genéticas (ClinVar)
74 variantes patogênicas registradas no ClinVar.
Vias biológicas (Reactome)
17 vias biológicas associadas aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Arterite de células gigantes
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
🟢 Recrutando agora
17 pesquisas recrutando participantes. Converse com seu médico sobre a possibilidade de participar.
Outros ensaios clínicos
185 ensaios clínicos encontrados, 25 ativos.
Publicações mais relevantes
Mostrando amostra de 200 publicações de um total de 3.680
Polymyalgia Rheumatica.
Polymyalgia rheumatica is an inflammatory condition that affects persons older than 50 years of age and is characterized by pain in both shoulders with or without hip or neck pain (or both) and with pronounced morning stiffness. The condition is typically diagnosed on the basis of these hallmark symptoms along with elevated inflammation markers (erythrocyte sedimentation rate and C-reactive protein level) and the ruling out of other conditions including giant-cell arteritis. Glucocorticoids are the primary treatment, which provide rapid symptom relief. The initial dose, usually 12.5 to 25 mg of prednisone equivalent daily, is gradually reduced, ideally over 12 months or less, although the disease course varies and polymyalgia rheumatica may persist for a longer duration. Relapses are common and sometimes warrant the use of interleukin-6 receptor inhibitors or methotrexate to minimize glucocorticoid exposure.
Systematic Review and Meta-Analysis for JCS 2026 Guideline on Management of Large-Vessel Vasculitis.
To provide evidence from randomized controlled trials (RCTs) for large-vessel vasculitis (LVV), including Takayasu arteritis (TAK) and giant cell arteritis (GCA), to inform the forthcoming 2026 Japanese Circulation Society (JCS) clinical practice guideline. We drafted 4 and 7 clinical questions for TAK and GCA, respectively. A systematic review (SR) of RCTs was conducted using PubMed, CENTRAL, EMBASE, and the Japan Medical Abstracts Society through March 2024. Assessed with the GRADE approach, the certainty of evidence was very low for the most critical outcomes, low for some outcomes, and moderate for only 1 outcome. Evidence for TAK was limited. Tocilizumab (TCZ) resulted in a numerically lower relapse rate vs. placebo (risk ratio (RR) 0.73, 95% confidence interval (CI) 0.39-1.37) and was similar to adalimumab. No clear difference between mycophenolate mofetil (MMF) and methotrexate (MTX), or between abatacept (ABA) and placebo was observed. In GCA, TCZ reduced relapse (RR 0.29, 95% CI 0.09-0.98) and increased remission (RR 3.56, 95% CI 2.29-5.54) over placebo at 52 weeks. Tumor necrosis factor inhibitor, ABA, and MTX showed no benefit in cranial GCA. Serious adverse events were comparable between treatment groups. Geographic variation and differences in entry criteria were noted. This SR was comprehensive synthesis of evidence from RCTs for LVV therapies to support the 2026 JCS guideline.
Hydrocortisone replacement therapy in patients with glucocorticoid withdrawal syndrome after cessation of glucocorticoid treatment: REPLACE, a multicentre, randomised, double-blinded, placebo-controlled, 16-week study protocol.
Glucocorticoid therapy is prescribed for a variety of inflammatory conditions and is associated with severe adverse effects. A glucocorticoid withdrawal syndrome (GWS) may occur after prolonged glucocorticoid treatment-with or without biochemical glucocorticoid-induced adrenal insufficiency (GIAI). Previously, GWS was not considered an entity, probably due to the overlap between symptoms of GWS and GIAI. The Addison's disease-specific quality of life questionnaire (AddiQoL-30) is a validated tool for quantifying symptoms of adrenal insufficiency resembling GWS. In the present study, we test the hypothesis that patients with a low AddiQoL-30 score and/or low cortisol response to a short Synacthen test (SST), after cessation of prednisolone treatment, may benefit from low-dose hydrocortisone therapy without increasing the risk of metabolic and cardiovascular disease during prolonged cortisol exposure. REPLACE is a multi-centre, double-blinded, placebo-controlled randomised controlled trial in patients with polymyalgia rheumatica or giant cell arteritis after cessation of prednisolone treatment. Criteria for randomisation are an AddiQoL-30 score ≤85 and/or plasma cortisol response to SST, 30-min p-cortisol >100 and <420 nmol/L. Patients will be randomised to oral hydrocortisone (10 mg two times a day) or placebo for 16 weeks. Baseline and follow-up examinations comprise AddiQoL-30 questionnaire, SST, blood samples, standardised blood pressure, physical function tests and assessment of bone quality and body composition. At baseline, two comparator groups include: (1) patients with a SST-stimulated cortisol ≥420 nmol/L and AddiQoL-30 score >85; and (2) patients with a SST-stimulated cortisol ≤100 nmol/L. The study is conducted in accordance with the Declaration of Helsinki, registered at the Clinical Trials Information System (CTIS: 2024-513822-53-00) and Clinicaltrials.gov (NCT05193396), and publications will be in accordance with the recommendations of the International Committee of Medical Journal Editors. The trial is monitored by local independent Good Clinical Practice units and overseen by the Danish Data Protection Agency (journal no. 21/27119), the Regional Committees on Health Research Ethics for Southern Denmark (project ID: S-20210076), the Danish Patient Safety Authority and the Danish Medicines Agency. NCT05193396.
Pulmonary artery aneurysm as a rare manifestation of giant cell arteritis.
A female patient in her 70s with a remote history of vocal cord paralysis was incidentally found to have a pulmonary artery aneurysm on a chest CT. Serial imaging performed over 3 years noted enlargement beyond 5.5 cm, prompting surgical repair. Histopathological examination revealed granulomatous arteritis with multinucleated giant cells and disruption of the elastic lamina, consistent with large-vessel giant cell arteritis (GCA). The patient was treated with corticosteroids and subsequently transitioned to subcutaneous tocilizumab, achieving postoperative stability on imaging and normalisation of inflammatory markers.This case highlights an unusual presentation of GCA with isolated pulmonary artery involvement, underscoring the diagnostic value of surgical tissue biopsy and the importance of considering vasculitis in aneurysmal disease, even in the absence of systemic manifestations.
Scalp necrosis and visual loss in giant cell arteritis: the importance of recognising atypical cutaneous clues.
A 70-year-old woman had presented with electric shock-like left hemifacial pain, with bilateral forehead skin plaques, diagnosed as shingles. 2 weeks later, she suddenly lost vision in the left eye. She had left optic disc oedema and bilateral necrotic-looking scalp lesions. Temporal artery biopsy was consistent with active temporal arteritis. Giant cell arteritis (GCA) may rarely present with scalp necrosis due to vasculitis of the facial arteries; the resulting hemifacial pain and atypical scalp rash may be misinterpreted as varicella zoster infection, delaying urgent intervention for GCA.
Publicações recentes
Clonal hematopoiesis of indeterminate potential and relapses in patients with giant cell arteritis.
Diagnostic accuracy of ultrasound versus cranial MRI for giant cell arteritis: dependence on cardiovascular risk for ultrasound only.
A Delphi exercise informing the development of criteria to measure response to treatment in giant cell arteritis.
Recognition of giant cell arteritis and calcified carotid artery atheromas in dental practice: systematic review and meta-analysis.
📚 EuropePMC5.037 artigos no totalmostrando 195
Racial and Ethnic Disparities in Severe Ischemic Manifestations and Tocilizumab Use Among Patients With Giant Cell Arteritis: A Nationwide Retrospective Cohort Study Using TriNetX.
Journal of neuro-ophthalmology : the official journal of the North American Neuro-Ophthalmology SocietyAdvances in the management of giant cell arteritis-aortitis: biologic therapies and beyond - a narrative review.
Expert opinion on biological therapyTakayasu and Giant Cell Arteritis Unmasked by Vedolizumab as Paradoxical Reactions: Two Case Reports.
ACR open rheumatologyAdded value of [⁶⁸Ga]Ga-FAPI-46 PET/CT in cranial giant cell arteritis missed by [¹⁸F]FDG PET/CT.
European journal of nuclear medicine and molecular imagingMethylprednisolone pulses are associated with faster remission in Giant Cell Arteritis: a multicentre inception cohort study.
Arthritis research & therapyGiant cell arteritis-associated temporomandibular joint arthritis confirmed by imaging.
Rheumatology advances in practiceRegarding the Prognostic Value of the HALP Score in Giant Cell Arteritis and Polymyalgia Rheumatica.
International journal of rheumatic diseasesAdvances in the use of Janus kinase inhibitors.
Current opinion in rheumatologyGiant cell arteritis and atherosclerosis: coexistence or causality?
Clinical and experimental rheumatologyGiant cell arteritis, neuralgia, dental pain.
British dental journalLarge-Vessel Vasculitis With Autoimmune Myelodysplastic Syndrome: An Uncommon Case of Large-Vessel Vasculitis With Cytopenia That Is Vacuoles, E1 Enzyme, X-linked, Autoinflammatory, Somatic Syndrome (VEXAS) Negative.
CureusIntracranial Giant Cell Arteritis Progressing despite Treatment with High Doses of Corticosteroids: Case Report.
Case reports in ophthalmologyEchoes of Inflammation: Cardiovascular Risk in Giant Cell Arteritis.
European journal of preventive cardiologySystemic Conditions Associated with Primary Open-Angle Glaucoma and Normal Tension Glaucoma in a Large US Adult Cohort.
Ophthalmic epidemiologyJanus Kinase inhibitors in the treatment of large vessel vasculitis: a systematic review and meta-analysis.
Open medicine (Warsaw, Poland)Giant Cell Arteritis With Medin-Derived Amyloid (AMed) Deposition in a Patient With COVID-19: An Autopsy Case.
Pathology internationalAssociation of Autoimmune Diseases With Pancreatic Cancer: A Nationwide Follow-Up Study From Sweden.
Cancer medicineAlternating Amaurosis Fugax: A Critical Warning Sign of Giant Cell Arteritis.
The American journal of medicineHalo sign is not always due to giant cell arteritis.
Internal medicine journalUltrasound, PET/CT or temporal artery biopsy for giant cell arteritis? A prospective diagnostic accuracy study (the GAME-study).
Acta ophthalmologicaChanging Trends in Temporal Artery Biopsy Rates in Australia: A Nationwide Study Over 31 Years.
ANZ journal of surgerySafety of Immune Checkpoint Inhibitors in Cancer Patients With Preexisting Autoimmune Vasculitis.
ACR open rheumatologyTreatment-resistant arterial hypertension revealing giant cell arteritis: A case report.
The American journal of medicineA case of large-vessel giant cell arteritis onset in a patient over 90 years old: Diagnostic challenge in differentiating from an infectious aneurysm.
Journal of cardiology casesGiant cell arteritis-polymyalgia rheumatica spectrum disease (GPSD): Relation with neoplasms and possible role as a paraneoplastic syndrome.
Reumatologia clinicaA Five-Step Approach to Acute Vision Loss: A Practical Narrative Review for Clinicians.
Clinical ophthalmology (Auckland, N.Z.)Calprotectin and serum amyloid A for disease activity assessment in giant cell arteritis and polymyalgia rheumatica: results from a prospective single-centre cohort study.
Rheumatology internationalRisk factors for acute coronary syndrome in patients with giant cell arteritis: a scoping review.
Therapeutic advances in musculoskeletal diseaseRisk factors of serious infections in patients with large-vessel vasculitis after the approval of tocilizumab in 2017: a retrospective nested case-control study using the Japanese health insurance database.
Arthritis research & therapy[Autoimmune hearing loss in giant cell arteritis: a clinical case].
Vestnik otorinolaringologiiAn aneurysm without a headache: large-vessel giant cell arteritis presenting solely as aortic aneurysm.
Journal of cardiothoracic surgeryAbsolute quantification of microRNA miR-875-5p in temporal artery biopsies and its biomarker potential for giant cell arteritis.
Frontiers in immunologyCrowned Dens Syndrome Mimicking Atlantoaxial Infection in a Patient With Systemic Sclerosis: A Case Report.
Case reports in rheumatologyOrbital MRI for diagnosing giant cell arteritis in cases of anterior ischaemic optic neuropathy.
RMD openPrognosis and long term outcome of stenotic large vessel involvement in giant cell arteritis.
Arthritis & rheumatology (Hoboken, N.J.)Large Vessel Vasculitis Primarily Affecting the Lower Extremities: A Case Series and Literature Review.
Journal of clinical rheumatology : practical reports on rheumatic & musculoskeletal diseasesIs there a seasonal pattern in giant cell arteritis? Revisiting the evidence in a large monocentric cohort over 30 years.
Seminars in arthritis and rheumatismSwitching from Originator Tocilizumab to Biosimilar in Giant Cell Arteritis: Evaluation of Effectiveness and Safety in a Multicenter Cohort of 38 Patients.
Drugs & agingClinical characteristics of giant cell arteritis with ocular involvement: A single-centre retrospective study.
Modern rheumatology[The retinal artery occlusion].
Klinische Monatsblatter fur AugenheilkundeStroke characteristics in giant cell arteritis and Takayasu arteritis: A multicenter retrospective cohort study of 108 patients.
Seminars in arthritis and rheumatismIFNL4 genotype is associated with hepatitis A virus infection findings from a focused phenotype study in the UK Biobank Cohort.
International journal of infectious diseases : IJID : official publication of the International Society for Infectious DiseasesSystemic Amyloidosis Masquerading as Giant Cell Arteritis.
OphthalmologyUnderstanding the patient experience of newly diagnosed giant cell arteritis.
Rheumatology advances in practiceSystematic Review and Meta-Analysis for JCS 2026 Guideline on Management of Large-Vessel Vasculitis.
Circulation journal : official journal of the Japanese Circulation SocietyA phase 2, randomised, placebo-controlled study of guselkumab in adults with new-onset or relapsing giant cell arteritis.
Annals of the rheumatic diseasesDiagnostic Challenges and Modern Therapeutic Strategies in Giant Cell Arteritis.
Diagnostics (Basel, Switzerland)Long-Term Follow-Up in Patients with Large-Vessel Vasculitis Applying Extracranial and Transcranial Duplex Sonography.
Diagnostics (Basel, Switzerland)Extracranial subcutaneous nodules in giant cell arteritis: response to baricitinib.
Clinical and experimental rheumatologyRe: Chauhan et al.: Risk of giant cell arteritis among patients presenting with undifferentiated noninfectious uveitis (Ophthalmology. 2025;132:1180-1182).
OphthalmologySalvage therapy with JAK inhibitors in refractory Takayasu arteritis: a multicentre experience.
RMD openAutoantibodies and B Cells in Takayasu Arteritis and Giant Cell Arteritis: Comparative Insights into Large-Vessel Vasculitis.
The Tohoku journal of experimental medicinePatient experiences of PMR: a qualitative narrative literature review.
Rheumatology advances in practiceEstablishing C-X-C motif chemokine receptor 4 as a novel imaging target in giant cell arteritis.
Arthritis research & therapyColor Doppler Ultrasound Versus Magnetic Resonance Imaging for Diagnosing Giant Cell Arteritis: A Systematic Review and Meta-Analysis.
CureusA corona-like distribution and patchy pattern of cerebellar infarcts identify patients with giant cell arteritis.
Therapeutic advances in neurological disorders[Large vessel vasculitis without aortitis in giant cell arteritis: About 4 cases].
La Revue de medecine interneAnterior Ischemic Optic Neuropathy Associated with Acute Severe Anemia Due to Myelodysplastic Syndrome (MDS): A Case Report.
Neuro-ophthalmology (Aeolus Press)Giant Cell Arteritis/Polymyalgia Rheumatica and Atypical Pulmonary Carcinoid Tumor: A Paraneoplastic Syndrome?
The American journal of case reportsDynamic vascular changes on long-term ultrasound monitoring predict relapse in large-vessel giant cell arteritis.
Arthritis research & therapyHydrocortisone replacement therapy in patients with glucocorticoid withdrawal syndrome after cessation of glucocorticoid treatment: REPLACE, a multicentre, randomised, double-blinded, placebo-controlled, 16-week study protocol.
BMJ openThe characteristics of giant cell arteritis patients that went blind in spite of treatment: case based narrative literature review.
Rheumatology internationalTherapeutic management of inflammatory heart diseases.
Pharmacology & therapeuticsPerformance of the Southend Giant Cell Arteritis Probability Score in a Single-Centre New Zealand Fast-Track Pathway.
International journal of rheumatic diseasesEasily Missed? Giant cell arteritis.
BMJ (Clinical research ed.)High-resolution imaging of giant cell arteritis with photon-counting computed tomography.
Annals of the rheumatic diseasesPulmonary artery aneurysm as a rare manifestation of giant cell arteritis.
BMJ case reportsParacentral Acute Middle Maculopathy Associated with Arteritic Anterior Ischemic Optic Neuropathy in a Case of Giant Cell Arteritis.
Klinische Monatsblatter fur AugenheilkundeErdheim-Chester disease mimicking IgG4-related disease.
Modern rheumatology case reportsA rare pair: two cases of clinically isolated pulmonary artery aneurysm.
Therapeutic advances in cardiovascular diseaseBarriers to immediate corticosteroid treatment in suspected giant cell arteritis with visual symptoms: insights from a tertiary eye care unit.
BMC ophthalmologyCardiovascular Risk Factors and Antiphospholipid Antibodies in Giant Cell Arteritis-Related Thrombosis.
Archives of rheumatologyThe real-world experience of combined cranial and large vessel 18F-FDG-PET/CT in the investigation of giant cell arteritis.
Clinical rheumatologyPrevalence of diplopia among giant cell arteritis patients: a systematic review and meta-analysis.
Eye (London, England)OCT and OCT-A Findings in Giant Cell Arteritis: PAMM as a Specific Ischemic Marker.
Retina (Philadelphia, Pa.)The Association of Polymyalgia Rheumatica and Giant Cell Arteritis With COVID-19 Vaccination: A Systematic Review.
Clinical medicine insights. Arthritis and musculoskeletal disordersGiant Cell Arteritis Mimicking Temporomandibular Disorder: Diagnostic Value of Temporal Artery Halo Sign.
Journal of clinical and experimental dentistryAdvances in management of giant cell arteritis.
Internal medicine journalConcurrent Thyroid Tumor in an Elderly Patient with Giant Cell Arteritis: A Case Report.
The Tohoku journal of experimental medicineRe: comment on: Miedany et al. response letter: Beyond the symptoms: personalizing giant cell arteritis care through multidimensional patient reported outcome measure. Volume 75, December 2025, 152844.
Seminars in arthritis and rheumatismDistinguishing Takayasu Arteritis and Giant Cell Arteritis Based on Large-Vessel Involvement Patterns.
Yonsei medical journalGiant Cell Arteritis With Central Nervous System Vasculitis Presenting As Binocular Diplopia and Ptosis due to Third Cranial Nerve Palsy.
CureusGiant Cell Arteritis Following Dental Procedure.
CureusAutomated detection of giant cell arteritis from temporal artery biopsy specimens using deep learning approaches.
Scientific reportsCardiovascular risk among Giant cells arteritis patients.
European journal of preventive cardiologyIschemia of the Tongue and Scalp as an Uncommon Presentation of Giant Cell Arteritis.
European journal of case reports in internal medicineAtypical Oral Presentation of Giant Cell Arteritis With Subsequent Middle Cerebral Artery Involvement.
CureusSubcutaneous Versus Intravenous Tocilizumab in Aortitis Associated With Giant Cell Arteritis: Multicenter Study of 196 Patients.
Arthritis care & researchExploring the Association Between Autoimmune and Inflammatory Diseases and Uveitis.
American journal of ophthalmologyIn synergy with interferon-gamma, interleukin-17 activates vascular stromal cells towards a pro-inflammatory profile in giant cell arteritis.
Arthritis & rheumatology (Hoboken, N.J.)Fast-Track Clinics and Visual Outcomes in Giant Cell Arteritis: A Systematic Review and Meta-Analysis.
Journal of clinical rheumatology : practical reports on rheumatic & musculoskeletal diseasesImaging-guided stratification in giant cell arteritis: prognostic and therapeutic implications.
Therapeutic advances in musculoskeletal diseaseClinical Decision-Making Case: A Giant Headache.
Journal of education & teaching in emergency medicinePotential clinical utility of quantitative 18F-FDG PET/CT parameters in evaluating vascular inflammation in giant cell arteritis.
Clinical and experimental rheumatologyCOVID-19 vaccination and systemic autoimmune rheumatic diseases: No evidence of disproportionately increased reporting in VAERS.
Seminars in arthritis and rheumatismScalp necrosis and visual loss in giant cell arteritis: the importance of recognising atypical cutaneous clues.
Practical neurologyA Case of CRP-Negative Giant Cell Arteritis Detected by Contrast-Enhanced Orbital MRI.
CureusCurrent clinical practice trends in giant cell arteritis diagnosis and management: a national survey of Australian rheumatologists and rheumatology trainees.
Internal medicine journalPatient perspectives on life impact and unmet needs in giant cell arteritis and polymyalgia rheumatica: insights from social media.
Rheumatology advances in practiceWhen the Eyes Deceive: Uncommon Ophthalmic Presentation of Giant Cell Arteritis.
CureusBilateral Optic Sheath Enhancement in Giant Cell Arteritis (GCA) Presenting With Occipital Neuralgia-Like Symptoms.
CureusHow common is vasculitis: what do population-based data tell us?
Current opinion in rheumatologySex differences among patients with giant cell arteritis: insights from the Spanish ARTESER Registry.
Rheumatology (Oxford, England)Varicella Zoster Virus in Giant Cell Arteritis: Evidence From a Systematic Review and Meta-Analytic Synthesis.
Reviews in medical virologyTreatment Patterns and Clinical Outcomes for Patients Living with Active Giant Cell Arteritis in Canada.
Rheumatology and therapyCellular senescence in giant cell arteritis and polymyalgia rheumatica: From mechanisms to therapeutic opportunities.
European journal of clinical investigationThoracic Aortic Aneurysm and Giant Cell Arteritis: Clarifying the Link.
Aorta (Stamford, Conn.)Neuro-ophthalmic Manifestations of Multiple Sclerosis.
International ophthalmology clinicsOral glucocorticoid pulse therapy: a modest change in clinical practice with major benefits.
The Lancet. RheumatologyBilateral Occipital Lobe Infarcts, A Rare Cause of Vision Loss in Giant Cell Arteritis.
Journal of neuro-ophthalmology : the official journal of the North American Neuro-Ophthalmology SocietyPerformance of Diagnostic Examinations for Giant Cell Arteritis and Subtypes: A Multicenter Japanese Study.
International journal of rheumatic diseasesOverlapping macrophage immune profiles in polymyalgia rheumatica and giant cell arteritis.
Rheumatology (Oxford, England)Management of extracranial carotid artery pseudoaneurysms.
Journal of vascular surgery cases and innovative techniquesMarkers of Giant Cell Arteritis in Patients Presenting With Ischemic Stroke: A Scoping Review.
European journal of neurologyGiant Cell Arteritis Causing Isolated Pulmonary Artery Aneurysm.
JACC. Case reportsThe Use of Vessel Wall Imaging for Making an Early Diagnosis of Giant Cell Arteritis in a Case with Cerebral Infarction.
Internal medicine (Tokyo, Japan)Temporal Artery Biopsy: A 10-Year Multi-centre Review of Current Practice.
CureusThe influence of baseline aortitis on aortic dilation risk in GCA: a multicentre imaging study.
Rheumatology (Oxford, England)Mönckeberg medial calcific sclerosis mimicking temporomandibular disorder and giant cell arteritis: a case report.
Quintessence international (Berlin, Germany : 1985)Infographic: GiACTA - Trial of Tocilizumab in Giant-Cell Arteritis.
Eye (London, England)Giant Cell Aortitis and Tuberculosis: Coincidence or a Causal Link?
CureusFast-track pathway for giant cell arteritis: Improved visual outcomes and reduced healthcare costs.
PloS oneLarge Vessel Vasculitis: Multimodality Imaging Findings and Technical Principles.
Radiographics : a review publication of the Radiological Society of North America, IncIdentification of BHLHE40-expressing T cells in giant cell arteritis amplified by interleukin-1.
Immunological medicine[Chinese expert consensus on the treatment of immune-mediated inflammatory diseases with Janus kinase inhibitors].
Zhonghua nei ke za zhiGiant cell arteritis in clinical practice: beyond GiACTA.
Clinical and experimental rheumatologyEosinophilic granulomatosis with polyangiitis mimicking giant cell arteritis.
Canadian journal of ophthalmology. Journal canadien d'ophtalmologieThe effectiveness and safety of leflunomide in the treatment of giant cell arteritis: a systematic review and meta-analysis.
Rheumatology advances in practiceUnusual Presentation of Giant Cell Arteritis With Localised Temporal Artery Aneurysm.
CureusA Rare Case of Giant Cell Arteritis Affecting Two Giants: Pulmonary and Root of Aorta Aneurysm.
Clinical case reportsIdentification of therapeutic targets for giant cell arteritis through integrated analysis of multi-omics datasets.
Hepatobiliary & pancreatic diseases international : HBPD INTCharacteristics of patients with major relapse in giant cell arteritis: a multicenter case-control study.
Clinical rheumatologyUncommon coexistence of giant cell arteritis and SIADH: case reports and literature review.
Internal and emergency medicinePatient characteristics, disease manifestations and diagnostic findings of consecutive patients suspected of Giant Cell Arteritis (GCA) - retrospective experience from a fast-track clinic in Israel.
Clinical rheumatologyThe Type I Interferon Axis in Systemic Autoimmune Diseases: From Molecular Pathways to Targeted Therapy.
BiomoleculesThe Role of Imaging in Monitoring Large Vessel Vasculitis: A Comprehensive Review.
BiomoleculesA Case of Giant Cell Arteritis Presenting With a Hyperechoic Wall Thickening on Temporal Artery Ultrasonography.
CureusMortality in isolated polymyalgia rheumatica and giant cell arteritis is not increased: evidence from cohort data.
Clinical and experimental medicineNocardia farcinica Brain Abscess in a Glucocorticoid-Treated Patient with Giant-Cell Arteritis: A Case Report.
The American journal of case reportsStudy on the chemokine CXCL10 in serum for its value in GCA-PMR spectrum disease stratification.
Clinical rheumatologyCan HALP Score Predict the Prognosis of Patients With Giant Cell Arteritis and Polymyalgia Rheumatica?
International journal of rheumatic diseasesThe Role of FDG-PET in the Diagnosis and Monitoring of Large-Vessel Vasculitis.
Current rheumatology reportsDiagnostic and prognostic utility of complete blood count-derived ratios in giant cell arteritis: a retrospective fast-track clinic cohort study.
Rheumatology internationalRecurrent vertebrobasilar stroke in giant cell arteritis associated with progressive prostate carcinoma: a case report and literature review.
Clinical rheumatologyCurrent Insights and Future Perspectives for the Use of Serological Biomarkers in Polymyalgia Rheumatica.
Journal of inflammation researchEarly-stage cost-utility analysis of novel diagnostic tests for giant cell arteritis: a modelling study in UK secondary care.
BMJ openUnmasking the Great Mimic: An Atypical Presentation of Giant Cell Arteritis With Recurrent and Isolated Diplopia.
CureusIncreased expression of Toll-like receptors and associated alarmins in temporal arteries of patients with giant cell arteritis.
Molecular medicine (Cambridge, Mass.)Ultrasound localisation microscopy reveals mural neovascularisation to diagnose and track giant cell arteritis.
Annals of the rheumatic diseasesTocilizumab monotherapy versus combined in aortitis associated with giant cell arteritis: Factors associated with imaging remission in a multicenter open-label study of 196 patients.
Seminars in arthritis and rheumatism[Lingual symptoms as an initial manifestation of giant cell arteritis].
SemergenOptical coherence tomography angiography detects retinal microvascular changes in giant cell arteritis: the potential protective role of aortitis.
RMD openAn Unusual Case of Cerebral Venous Sinus Thrombosis With Negative D-dimer Mimicking Giant Cell Arteritis.
CureusPolymyalgia rheumatica and giant cell arteritis: lumping versus splitting.
Rheumatology (Oxford, England)Syphilitic Cardiac and Vascular Disease: A Comprehensive Review.
Cardiology in review[Giant cell arteritis (GCA) presenting as isolated paracentral acute middle maculopathy (PAMM)].
Journal francais d'ophtalmologieTreatment and evolution of 134 patients with aortitis and periaortitis: experience of a third-level university hospital.
Internal and emergency medicineYou Never Think Enough About Giant Cell Arteritis.
Ocular immunology and inflammationA Case Report of Bilateral Sequential Central Retinal Artery Occlusion in Occult Giant Cell Arteritis: The Eyes Are Windows to Systemic Disease.
CureusMedium-sized vessel uptake on PET/CT as a clue to extracranial giant cell arteritis.
Revista clinica espanolaGiant Cell Arteritis Manifesting as Area Postrema Syndrome: A Case Report.
CureusVasculitis syndromes: large vessel vasculitides and ANCA-associated vasculitides from a neuroradiologist's perspective.
Japanese journal of radiologyRisk of hospitalization with pneumonia in patients with giant cell arteritis and anti-neutrophil cytoplasmic antibody associated vasculitis.
Rheumatology (Oxford, England)Can Vitamin D Reduce Glucocorticoid-Induced Adverse Effects in Patients with Giant Cell Arteritis? Results from 1568 Patients in the Spanish ARTESER Registry.
NutrientsTemporal artery biopsy and temporal artery ultrasound inter-rater agreement for the diagnosis of giant cell arteritis: an ancillary analysis from the multicentre prospective ECHORTON study.
Rheumatology internationalThe Interplay Between Varicella-Zoster Virus and Giant Cell Arteritis: An In-Depth Narrative Review.
CureusPredictors of giant cell arteritis in patients with polymyalgia rheumatica in southern Sweden-a retrospective study.
Rheumatology advances in practiceRefractory Hypothyroidism: Unexpected Outcome During Treatment of Giant Cell Arteritis.
Clinical case reportsReviewer Comment on Rizwan et al. "CT Angiography of the Head for the Initial Assessment of Giant Cell Arteritis: Presenting Symptoms, Biopsy Outcomes and Alternative Diagnosis".
The Canadian journal of neurological sciences. Le journal canadien des sciences neurologiques[Giant cell arteritis - When should the GP consider it?].
MMW Fortschritte der MedizinVascular uptake on 18F-FDG PET/CT predicts relapse in new-onset PMR.
Rheumatology (Oxford, England)Seasonality and latitude as linked environmental factors in giant cell arteritis incidence: a systematic review and meta-analysis.
Rheumatology internationalAn Atypical Presentation of Giant Cell Arteritis in an Elderly Patient: Diplopia and Fever Masked by Pneumonia.
CureusBirdshot Chorioretinopathy in a Patient on Tocilizumab for the Treatment of Giant Cell Arteritis.
Case reports in ophthalmological medicineHalo Sign on Temporal Artery Ultrasound Aids in Prompt Diagnosis of Giant Cell Arteritis.
Methodist DeBakey cardiovascular journalSpatial profiling of giant cell arteritis tissues reveals immune heterogeneity and potential predictors of glucocorticoid response.
Annals of the rheumatic diseasesSerum interleukin-1 receptor antagonist levels are a useful marker of disease activity and risk of relapse in large vessel vasculitis.
CytokineMature CD209+CD83+CCR7+ dendritic cells infiltrate the arterial wall in giant cell arteritis and derive from in-situ monocyte differentiation.
Scientific reportsUnderstanding the immunopathophysiology of polymyalgia rheumatica: implications for treatment.
Annals of the rheumatic diseasesCase Report: Transient monocular vision loss with isolated paracentral acute middle maculopathy on optical coherence tomography: beware of giant cell arteritis!
Frontiers in neurologyOculoplastics and Augmented Intelligence: A Literature Review.
Journal of clinical medicineModern Management of Isolated Polymyalgia Rheumatica.
Rheumatology and therapyMonocytes/Macrophages in Giant Cell Arteritis-Polymyalgia Rheumatica Spectrum Disease.
Aging and diseaseNew versus old: comparison of the 2022 ACR/EULAR versus the 1990 ACR classification criteria for giant cell arteritis in a real-world cohort.
Rheumatology internationalMultimodality imaging of giant cell arteritis.
Journal of clinical neuroscience : official journal of the Neurosurgical Society of AustralasiaTreatment of systemic vasculitis.
Current opinion in rheumatologyImmediate versus gradual TocilizuMab discontinuAtion in GIant Cell Arteritis: protocol of the multicentre randomised open-label MAGICA trial.
BMJ openSiegrist Streaks in a Case of Biopsy-negative Giant Cell Arteritis: A Case Report.
Ophthalmic surgery, lasers & imaging retinaThe Curious Case of Confounding Headaches.
Case reports in rheumatologyRacial differences in stroke, blindness, and mortality among Black versus non-Black patients with giant cell arteritis: an international cohort study.
Canadian journal of ophthalmology. Journal canadien d'ophtalmologieDupilumab-induced eosinophilic granulomatosis with polyangiitis mimicking giant cell arteritis.
Canadian journal of ophthalmology. Journal canadien d'ophtalmologieTranscatheter Aortic Valve Implantation for Severe Bicuspid Aortic Stenosis With Concomitant Giant Cell Arteritis Aortitis.
JACC. Case reportsCT Angiography of the Head for the Initial Assessment of Giant Cell Arteritis: Presenting Symptoms, Biopsy Outcomes and Alternative Diagnosis.
The Canadian journal of neurological sciences. Le journal canadien des sciences neurologiquesThe role of 18F-fluorodeoxyglucose positron emission tomography for vascular imaging.
Progress in cardiovascular diseasesImmune checkpoint inhibitor associated vasculitis and polymyalgia rheumatica: a case series and systematic review.
BMC rheumatologyAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Arterite de células gigantes.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Arterite de células gigantes
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Polymyalgia Rheumatica.
- Systematic Review and Meta-Analysis for JCS 2026 Guideline on Management of Large-Vessel Vasculitis.Circulation journal : official journal of the Japanese Circulation Society· 2026· PMID 41692437mais citado
- Hydrocortisone replacement therapy in patients with glucocorticoid withdrawal syndrome after cessation of glucocorticoid treatment: REPLACE, a multicentre, randomised, double-blinded, placebo-controlled, 16-week study protocol.
- Pulmonary artery aneurysm as a rare manifestation of giant cell arteritis.
- Scalp necrosis and visual loss in giant cell arteritis: the importance of recognising atypical cutaneous clues.
- Clonal hematopoiesis of indeterminate potential and relapses in patients with giant cell arteritis.
- Diagnostic accuracy of ultrasound versus cranial MRI for giant cell arteritis: dependence on cardiovascular risk for ultrasound only.
- Correction: The DANIsh VASculitis cohort study: protocol for a national multicenter prospective study including incident and prevalent patients with giant cell arteritis and polymyalgia rheumatica.
- A Delphi exercise informing the development of criteria to measure response to treatment in giant cell arteritis.
- Recognition of giant cell arteritis and calcified carotid artery atheromas in dental practice: systematic review and meta-analysis.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:397(Orphanet)
- OMIM OMIM:187360(OMIM)
- MONDO:0008538(MONDO)
- GARD:9615(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Artigo Wikipedia(Wikipedia)
- Q707816(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar