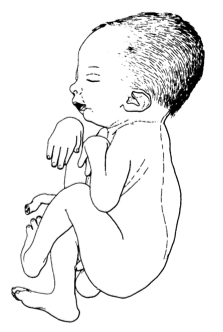
O tálus vertical congênito isolado (TVC) é uma deformidade podal rara, reconhecível ao nascimento por uma luxação da articulação talonavicular, resultando em uma orientação radiográfica quase vertical característica do tálus.
Introdução
O que você precisa saber de cara
O tálus vertical congênito isolado (TVC) é uma deformidade podal rara, reconhecível ao nascimento por uma luxação da articulação talonavicular, resultando em uma orientação radiográfica quase vertical característica do tálus.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 12 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 16 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
1 gene identificado com associação a esta condição. Padrão de herança: Autosomal dominant.
Sequence-specific transcription factor which is part of a developmental regulatory system that provides cells with specific positional identities on the anterior-posterior axis
Nucleus
Vertical talus, congenital
A rare malformation characterized by vertical orientation of the talus with a rigid dorsal dislocation of the navicular, equinus deformity of the calcaneus, abduction deformity of the forefoot, and contracture of the soft tissues of the hind- and mid-foot. This condition is usually associated with multiple other congenital deformities and only rarely is an isolated deformity with familial occurrence.
Variantes genéticas (ClinVar)
31 variantes patogênicas registradas no ClinVar.
Classificação de variantes (ClinVar)
Distribuição de 37 variantes classificadas pelo ClinVar.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Talo vertical congênito
Centros de Referência SUS
24 centros habilitados pelo SUS para Talo vertical congênito
Centros para Talo vertical congênito
Detalhes dos centros
Hospital Universitário Prof. Edgard Santos (HUPES)
R. Dr. Augusto Viana, s/n - Canela, Salvador - BA, 40110-060 · CNES 0003808
Serviço de Referência
Hospital Infantil Albert Sabin
R. Tertuliano Sales, 544 - Vila União, Fortaleza - CE, 60410-794 · CNES 2407876
Serviço de Referência
Hospital de Apoio de Brasília (HAB)
AENW 3 Lote A Setor Noroeste - Plano Piloto, Brasília - DF, 70684-831 · CNES 0010456
Serviço de Referência
Hospital Estadual Infantil e Maternidade Alzir Bernardino Alves (HIABA)
Av. Min. Salgado Filho, 918 - Soteco, Vila Velha - ES, 29106-010 · CNES 6631207
Serviço de Referência
Hospital das Clínicas da UFG
Rua 235 QD. 68 Lote Área, Nº 285, s/nº - Setor Leste Universitário, Goiânia - GO, 74605-050 · CNES 2338424
Serviço de Referência
Hospital Universitário da UFJF
R. Catulo Breviglieri, Bairro - s/n - Santa Catarina, Juiz de Fora - MG, 36036-110 · CNES 2297442
Atenção Especializada
Hospital das Clínicas da UFMG
Av. Prof. Alfredo Balena, 110 - Santa Efigênia, Belo Horizonte - MG, 30130-100 · CNES 2280167
Serviço de Referência
Hospital Universitário Julio Müller (HUJM)
R. Luis Philippe Pereira Leite, s/n - Alvorada, Cuiabá - MT, 78048-902 · CNES 2726092
Atenção Especializada
Hospital Universitário João de Barros Barreto
R. dos Mundurucus, 4487 - Guamá, Belém - PA, 66073-000 · CNES 2337878
Serviço de Referência
Hospital Universitário Lauro Wanderley (HULW)
R. Tabeliao Estanislau Eloy, 585 - Castelo Branco, João Pessoa - PB, 58050-585 · CNES 0002470
Atenção Especializada
Instituto de Medicina Integral Prof. Fernando Figueira (IMIP)
R. dos Coelhos, 300 - Boa Vista, Recife - PE, 50070-902 · CNES 0000647
Serviço de Referência
Hospital Pequeno Príncipe
R. Des. Motta, 1070 - Água Verde, Curitiba - PR, 80250-060 · CNES 3143805
Serviço de Referência
Hospital Universitário Regional de Maringá (HUM)
Av. Mandacaru, 1590 - Parque das Laranjeiras, Maringá - PR, 87083-240 · CNES 2216108
Atenção Especializada
Hospital de Clínicas da UFPR
R. Gen. Carneiro, 181 - Alto da Glória, Curitiba - PR, 80060-900 · CNES 2364980
Serviço de Referência
Hospital Universitário Pedro Ernesto (HUPE-UERJ)
Blvd. 28 de Setembro, 77 - Vila Isabel, Rio de Janeiro - RJ, 20551-030 · CNES 2280221
Serviço de Referência
Instituto Nacional de Saúde da Mulher, da Criança e do Adolescente Fernandes Figueira (IFF/Fiocruz)
Av. Rui Barbosa, 716 - Flamengo, Rio de Janeiro - RJ, 22250-020 · CNES 2269988
Serviço de Referência
Hospital São Lucas da PUCRS
Av. Ipiranga, 6690 - Jardim Botânico, Porto Alegre - RS, 90610-000 · CNES 2232928
Serviço de Referência
Hospital de Clínicas de Porto Alegre (HCPA)
Rua Ramiro Barcelos, 2350 Bloco A - Av. Protásio Alves, 211 - Bloco B e C - Santa Cecília, Porto Alegre - RS, 90035-903 · CNES 2237601
Serviço de Referência
Hospital Universitário da UFSC (HU-UFSC)
R. Profa. Maria Flora Pausewang - Trindade, Florianópolis - SC, 88036-800 · CNES 2560356
Serviço de Referência
Hospital das Clínicas da FMUSP
R. Dr. Ovídio Pires de Campos, 225 - Cerqueira César, São Paulo - SP, 05403-010 · CNES 2077485
Serviço de Referência
Hospital de Base de São José do Rio Preto
Av. Brg. Faria Lima, 5544 - Vila Sao Jose, São José do Rio Preto - SP, 15090-000 · CNES 2079798
Atenção Especializada
Hospital de Clínicas da UNICAMP
R. Vital Brasil, 251 - Cidade Universitária, Campinas - SP, 13083-888 · CNES 2748223
Serviço de Referência
Hospital de Clínicas de Ribeirão Preto (HCRP-USP)
R. Ten. Catão Roxo, 3900 - Vila Monte Alegre, Ribeirão Preto - SP, 14015-010 · CNES 2082187
Serviço de Referência
UNIFESP / Hospital São Paulo
R. Napoleão de Barros, 715 - Vila Clementino, São Paulo - SP, 04024-002 · CNES 2688689
Serviço de Referência
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
2 ensaios clínicos encontrados.
Publicações mais relevantes
Case Report: A novel missense variant in ZC4H2, c.196C>T p.(Leu66Phe), is associated with a mild, ZC4H2-related X-linked syndromic intellectual disability (ZARD) phenotype.
ZC4H2 is an X-linked gene that has emerged as critical for neural development, synaptic functioning, and gene regulation. We present an 11-month-old male who was evaluated for bilateral congenital vertical talus identified in the newborn period. Exome sequencing identified a hemizygous, missense variant in ZC4H2, NM_018684.4:c.196C>T p.(Leu66Phe), that affects the same amino acid residue as a previously reported, pathogenic ZC4H2 variant, c.197T>A p.(Leu66His). The variant was inherited from his mother, who had camptodactyly of the fifth fingers, and was also present in the maternal uncle who carried a diagnosis of cerebral palsy. The pathogenic missense variant in this family is located in the coiled-coil domain of the ZC4H2 protein. Although data remain scarce, missense variants in this domain may be associated with a milder, ZC4H2-associated rare disorder (ZARD) phenotype.
Naviculectomy With Limited Soft-Tissue Releases as a Third Way Beyond Manipulative Treatment and Extensive Soft-Tissue Releases for Ambulatory Children With Complex Congenital Vertical Talus: A Technical Note.
We investigated the radioclinical outcomes of naviculectomy and limited/tailored soft-tissue releases in a short series of ambulatory children with complex/intractable congenital vertical talus subsets namely neglected, multiple operated, and recurrent patients. We postulated that this technique will yield satisfactory radioclinical outcomes and minimal complications because it avoids extensive surgical release/trauma that is otherwise classically recommended for complex congenital vertical talus. The cohort consisted of 5-4 boys and 1 girl-complex congenital vertical talus children with neglected, multiple operated, and/or recurrent subsets. Patients were included if manipulative casting techniques were deemed unlikely to produce a plantigrade foot. Patients underwent naviculectomy with variable on-demand limited soft-tissue releases. Two patients had bilateral affection and 2 had a nonidiopathic cause. The mean age was 5.2 years (4-6.25) and mean follow-up was 2.3 years (1-3). We reported satisfactory outcomes as per foot posture, function, overall parent satisfaction including pain and radiography per lateral views of talar-axis-first metatarsal base angle on the short/intermediate term. Whereas manipulative casting is unlikely to yield lasting outcomes in ambulatory children with complex subsets of congenital vertical talus, extensive surgical soft-tissue releases have unfavorable long-term complications. As a substitute, naviculectomy as a form of resection arthroplasty created a practical and affordable third way between manipulative casting with or without minimally invasive surgery and the extensive surgical soft-tissue releases on the short-to-intermediate term.Level of Evidence:Level IV case series.
Defining and Differentiating Congenital Vertical Talus and Congenital Oblique Talus: It's Not Primarily About the Talus.
Congenital vertical talus (CVT) and congenital oblique talus (COT) are rocker-bottom foot deformities that have similar names and no objective definitions. This has led to confusion for practitioners, as well as scientific challenges for researchers. Our goal was to provide objective radiographic criteria to define and differentiate CVT and COT. We evaluated 62 pairs of maximum dorsiflexion and plantar flexion lateral radiographs of infant feet that had been clinically diagnosed with CVT. The dorsiflexion tibiotalar angle, the plantar flexion talus-first metatarsal angle, and the plantar flexion foot center of rotation of angulation (foot-CORA) were measured using transparent overlay tools. Freehand measurements were made on a subset of 10 pairs of radiographs to confirm clinical applicability. Nine contralateral pairs of radiographs of normal feet were measured for comparison. Specific values for the radiographic measurements were identified that, together, reliably differentiated the shapes of rocker-bottom feet with CVT, COT, and flexible flatfoot with a short tendo-Achilles (FFF-STA), as well as the shape of the normal foot. More severe and rigid rocker-bottom foot deformities were diagnosed with CVT. Less severe and more flexible deformities were diagnosed with COT. CVT, COT, FFF-STA, and normal feet can be reliably differentiated using 2 angular measurements and 1 bone position measurement on dorsiflexion and plantar flexion lateral radiographs. Our data indicated that the differentiation of CVT and COT is based primarily on the rigidity of the navicular dislocation rather than the verticality of the talus. The data further supported the proposition that COT is a foot deformity along a spectrum of valgus/eversion deformities of the hindfoot that requires early treatment. Application of these diagnostic criteria should lead to clinical studies that identify a specific treatment, treatment outcome, and prognosis for each deformity. Diagnostic Level II. See Instructions for Authors for a complete description of levels of evidence.
Caudal regression in fetus with de novo SMARCA2 pathogenic variant.
Nicolaides-Baraitser syndrome (NCBRS) is a rare autosomal dominant genetic condition that is characterized by severe intellectual disability, dysmorphic facial features, short stature, sparse hair, and early onset seizures. This diagnosis is established by suggestive clinical findings and the identification of a heterozygous SMARCA2 pathogenic variant by molecular genetic testing. There are not, however, consensus clinical diagnostic criteria for this condition as there are so few documented cases. Here, we present a case of prenatally diagnosed caudal regression with sacral agenesis and congenital vertical talus (rocker bottom feet) that was ultimately found to have a de novo SMARCA2 pathogenic variant. The patient had an amniocentesis with normal karyotype and microarray followed by failed direct rapid whole exome sequencing (WES) due to maternal cell contamination. She elected for termination of the pregnancy based on the clinical prognosis of the ultrasound findings; WES revealed a pathogenic variant after her termination. We believe this is the first case of these findings associated with NCBRS. If any future cases of either finding are found in association with a SMARCA2 genetic variant, caudal regression and rocker bottom feet should be included in the spectrum of physical traits associated with this pathogenic variant.
Minimally Invasive Method for Treatment of Syndromic Congenital Vertical Talus Deformity in Children.
Congenital Vertical Talus (CVT) is a rare form of rigid flatfoot commonly seen in patients with underlying neurologic syndromes. This study aims to evaluate the long-term effectiveness of the minimally invasive method for correcting CVT deformity in a large cohort of syndromic patients. A single author recorded preoperative, 2-week postoperative, 1-year postoperative, and most recent radiographic measurements and complications for 25 patients treated with the minimally invasive method from 2006 to 2021. Patient-Reported Outcomes Measurement Information System (PROMIS) questionnaires were administered for 12 patients after January 1, 2015, when the institution began collecting PROMIS in all orthopaedic patients. Average follow-up was 55 months (13-111); 18 patients had minimum 24-month follow-up. Forty feet in 25 patients were analyzed. The average preoperative lateral talar axis-first metatarsal base angle (TAMBA) was 68.7 ± 21.3 vs 12.1 ± 8.9 after initial surgical intervention (P < .0001). There was a statistically significant increase in the lateral TAMBA between the initial postoperative and final follow-up visits (13.0 vs 21.6, P = .02). Radiographic recurrence of talonavicular deformity was noted in 12 feet (30.9%); 7 (15.55%) required corrective surgery. Larger preoperative lateral TAMBA was predictive of recurrence. Notably, patients with arthrogryposis experienced higher radiographic recurrence than other syndromic patients (45.0% vs 14.3%, P = .0384). PROMIS scores were within population norms. The study suggests that less than one-third of syndromic CVT patients experienced a radiographic recurrence of talonavicular deformity, with 15% requiring further surgical intervention at an average of 55 months following the initial procedure. A higher incidence of radiographic recurrence occurred in patients with distal arthrogryposis. These findings, along with the satisfactory patient-reported outcomes, suggest that the minimally invasive technique is an effective treatment method for syndromic CVT, underscoring the necessity for clinicians to provide detailed prognoses and consider more intensive follow-up for those at higher risk.
Publicações recentes
Case Report: A novel missense variant in ZC4H2, c.196C>T p.(Leu66Phe), is associated with a mild, ZC4H2-related X-linked syndromic intellectual disability (ZARD) phenotype.
Defining and Differentiating Congenital Vertical Talus and Congenital Oblique Talus: It's Not Primarily About the Talus.
Caudal regression in fetus with de novo SMARCA2 pathogenic variant.
Minimally Invasive Method for Treatment of Syndromic Congenital Vertical Talus Deformity in Children.
Corrective bandages and daily manipulations for treatment of congenital vertical talus: a thirteen year follow-up.
📚 EuropePMC111 artigos no totalmostrando 55
Case Report: A novel missense variant in ZC4H2, c.196C>T p.(Leu66Phe), is associated with a mild, ZC4H2-related X-linked syndromic intellectual disability (ZARD) phenotype.
Frontiers in pediatricsDefining and Differentiating Congenital Vertical Talus and Congenital Oblique Talus: It's Not Primarily About the Talus.
JB & JS open accessCaudal regression in fetus with de novo SMARCA2 pathogenic variant.
Prenatal diagnosisMinimally Invasive Method for Treatment of Syndromic Congenital Vertical Talus Deformity in Children.
Foot & ankle internationalCorrective bandages and daily manipulations for treatment of congenital vertical talus: a thirteen year follow-up.
International orthopaedicsHeterozygous deletion of HOXC10-HOXC9 causes lower limb abnormalities in congenital vertical talus.
Journal of medical geneticsClarification on the distinction between congenital vertical talus and oblique talus diagnosis in the intrauterine period.
The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal ObstetriciansCongenital Vertical Talus: An Updated Review.
CureusHFA analysis using scalp electroencephalograms in two cases of Rasmussen's syndrome.
Epilepsy researchRelapsed Congenital Vertical Talus Deformity: Outcomes of a Modified Minimally Invasive Method.
Journal of pediatric orthopedicsExpanding the phenotype of DYNC1H1-associated diseases with a rare variant resulting in spinal muscular atrophy with lower extremity predominance (SMA-LED) and upper motor neuron signs.
The Turkish journal of pediatricsAnkle and Foot Deformities in Children.
Seminars in musculoskeletal radiologyCongenital vertical talus open reduction surgery: Technique description and our twenty-years personal experience.
La Pediatria medica e chirurgica : Medical and surgical pediatricsResults of treatment of congenital vertical talus by the Dobbs method.
Journal of orthopaedic surgery and researchPrenatal ultrasound diagnosis of congenital vertical talus.
The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal ObstetriciansComparison of Different Surgical Techniques in Correction of Congenital Vertical Talus Deformity: A Systematic Review and Meta-Analysis of the Literature.
Journal of pediatric orthopedicsChromosome 2 Interstitial Deletion (del(2)(q14.1q22.1) Syndrome With Novel Skeletal and Central Nervous System Features.
CureusCongenital vertical talus deformity in children with distal arthrogryposis: good clinical outcomes despite high rate of residual radiographic deformity.
Journal of pediatric orthopedics. Part BUntreated congenital vertical talus deformity in walking age: minimally invasive method works.
Journal of pediatric orthopedics. Part BPatient-Reported Pain and Function Outcomes in Children With Congenital Vertical Talus Treated With the Minimally Invasive Method.
Journal of pediatric orthopedicsMinimally Invasive Method in Treatment of Idiopathic Congenital Vertical Talus: Recurrence is Uncommon.
Journal of pediatric orthopedicsDiagnostic yield of exome sequencing in congenital vertical talus.
European journal of medical geneticsWhat is New in Pediatric Orthopaedic Foot and Ankle.
Journal of pediatric orthopedicsA case of focal cortical dysplasia type IIa with pathologically suspected bilateral Rasmussen syndrome.
Brain & developmentOutcomes of Naviculectomy for Severe Recurrent Clubfoot Deformity.
Foot & ankle orthopaedicsNaviculectomy With Limited Soft-Tissue Releases as a Third Way Beyond Manipulative Treatment and Extensive Soft-Tissue Releases for Ambulatory Children With Complex Congenital Vertical Talus: A Technical Note.
Foot & ankle specialistMid-trimester isolated bilateral rocker bottom feet leading to prenatal diagnosis of 7q11.23 microdeletion: Williams syndrome.
Journal of ultrasoundCongenital Vertical Talus.
Foot and ankle clinicsIs Arthrodesis Sufficient in the Setting of Complex, Severe and Rigid Progressive Collapsing Foot Deformities?
Foot and ankle clinicsMultimodality imaging of the paediatric flatfoot.
Skeletal radiologyOutcomes of a Minimally Invasive Approach for Congenital Vertical Talus With a Comparison Between the Idiopathic and Syndromic Feet.
Journal of pediatric orthopedicsComparison of outcome between idiopathic and non-idiopathic congenital vertical talus treated with soft tissue release.
Journal of pediatric orthopedics. Part BEpithelial dynamics shed light on the mechanisms underlying ear canal defects.
Development (Cambridge, England)Talectomy by Medial Surgical Approach for Congenital Vertical Talus in Arthrogryposis Multiplex Congenita.
OrthopedicsConjoined twins presenting with foot deformities: insights to management and challenges.
BMJ case reportsManagement of pediatric foot deformities: an imaging review.
Pediatric radiologyForefoot malformations, deformities and other congenital defects in children.
Orthopaedics & traumatology, surgery & research : OTSROne-stage release by double surgical approach for neglected congenital vertical talus: results in a series of walking children in Tanzania.
Journal of pediatric orthopedics. Part BNaviculectomy for two ambulatory children with intractable congenital vertical talus: redefining the indications of an old technique.
Journal of pediatric orthopedics. Part BBilateral Congenital Vertical Talus in Association with Beals Contractural Arachnodactyly: A Case Report.
JBJS case connector[The interdisciplinary approach to the rehabilitation of the patients presenting with congenital atresia of the external auditory canal and the concomitant microtia].
Vestnik otorinolaringologiiPrenatal congenital vertical talus (rocker bottom foot): a marker for multisystem anomalies.
Pediatric radiologyCongenital talipes equinovarus and congenital vertical talus secondary to sacral agenesis.
BMJ case reportsThe 2017 ABJS Nicolas Andry Award: Advancing Personalized Medicine for Clubfoot Through Translational Research.
Clinical orthopaedics and related researchMultiple pterygium syndrome: Challenge for anesthesiologist.
Saudi journal of anaesthesiaA comparison of the Dobbs method for correction of idiopathic and teratological congenital vertical talus.
Journal of children's orthopaedicsElectrophysiological findings in Rasmussen's syndrome.
Epileptic disorders : international epilepsy journal with videotapeDeletions of 5' HOXC genes are associated with lower extremity malformations, including clubfoot and vertical talus.
Journal of medical geneticsEffect of Amplification on Speech and Language in Children With Aural Atresia.
American journal of audiologySyndromic Feet: Arthrogryposis and Myelomeningocele.
Foot and ankle clinics[Vertical Talus: Mid-Term Results of Surgical Therapy].
Acta chirurgiae orthopaedicae et traumatologiae CechoslovacaA witnessed case of a classic metaphyseal fracture caused during IV line placement in a child: Insight into mechanism of injury.
Journal of forensic and legal medicineCongenital Vertical Talus: Etiology and Management.
The Journal of the American Academy of Orthopaedic SurgeonsWhat's New in Pediatric Flatfoot?
Journal of pediatric orthopedicsTreatment of Congenital Vertical Talus: Comparison of Minimally Invasive and Extensive Soft-Tissue Release Procedures at Minimum Five-Year Follow-up.
The Journal of bone and joint surgery. American volumeAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Talo vertical congênito.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Talo vertical congênito
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Case Report: A novel missense variant in ZC4H2, c.196C>T p.(Leu66Phe), is associated with a mild, ZC4H2-related X-linked syndromic intellectual disability (ZARD) phenotype.
- Naviculectomy With Limited Soft-Tissue Releases as a Third Way Beyond Manipulative Treatment and Extensive Soft-Tissue Releases for Ambulatory Children With Complex Congenital Vertical Talus: A Technical Note.
- Defining and Differentiating Congenital Vertical Talus and Congenital Oblique Talus: It's Not Primarily About the Talus.
- Caudal regression in fetus with de novo SMARCA2 pathogenic variant.
- Minimally Invasive Method for Treatment of Syndromic Congenital Vertical Talus Deformity in Children.
- Corrective bandages and daily manipulations for treatment of congenital vertical talus: a thirteen year follow-up.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:178382(Orphanet)
- OMIM OMIM:192950(OMIM)
- MONDO:0008652(MONDO)
- GARD:5488(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Q7355063(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar