Introdução
O que você precisa saber de cara
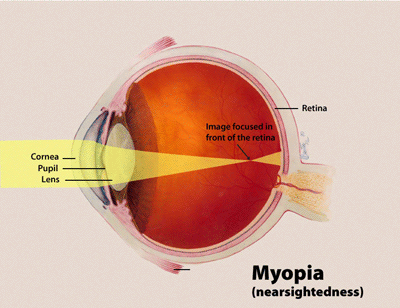
Miopia, também conhecida como visão curta, é uma condição ocular em que a luz proveniente de objetos distantes se foca à frente da retina, em vez de sobre ela. Como resultado, objetos distantes parecem embaçados, enquanto objetos próximos parecem normais. Outros sintomas podem incluir dores de cabeça e fadiga ocular. A miopia grave está associada a um risco aumentado de degeneração macular, descolamento de retina, catarata e glaucoma.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — NÃO RARA NA EUROPA: Degeneração macular miópica
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Exploring Concomitant Ophthalmic Comorbidities in Portuguese Patients with Inherited Retinal Diseases: A Comprehensive Clinical Study.
Background/Objectives: Inherited retinal diseases (IRDs) are a heterogeneous group of rare eye disorders characterized by progressive photoreceptor degeneration, leading to severe visual impairment or even blindness. This study aims to investigate the prevalence, types, and clinical significance of ophthalmic comorbidities in Portuguese patients with IRDs. Methods: This nationwide Portuguese population-based retrospective study was based on the IRD-PT registry (retina.com.pt). Statistical analysis was conducted using Microsoft® Excel® for Microsoft 365 and IBM SPSS Statistics version 29.0.2.0. Informed consent was obtained from all participants. Results: A total of 1531 patients (1254 families) from six centers were enrolled. The cohort consisted of 51% males, with a mean age of 45.8 ± 19.3 years and a mean age at diagnosis of 39.4 ± 19.5 years. Overall, ocular comorbidities were reported in 644 patients (42.1%). In 176 individuals (11.5%), multiple concurrent comorbidities were found. Cataract was the most common comorbidity (21.3%), followed by amblyopia (6.3%) and high myopia (5.9%). Statistically significant associations with ocular comorbidities were observed in isolated progressive IRDs. Specifically, AR RP was associated with cataract (p < 0.001), and gene analysis revealed several significant associations. CRB1 was statistically linked to epiretinal membrane (ERM) (p = 0.003), EYS with cataract (p = 0.001), PROM1 with choroidal neovascularization (CNV) (p = 0.0026), and USH2A with macular hole (p = 0.01). Patients with the RPE65 mutation in Leber congenital amaurosis were associated with ERM (p = 0.019). There was also a significant association between X-linked RP and high myopia (p < 0.001) and CNV in Best disease (p < 0.001); in syndromic IRDs, cataract, cystoid macular edema, and ERM were observed in Usher syndrome, p = 0.002, p = 0.002, and p = 0.005, respectively, and the MYO7A gene was linked to cataract (p = 0.041) and strabismus (p = 0.013); pseudoxanthoma elasticum was significantly associated with CNV (p = 0.002); and foveal hypoplasia was associated with anterior segment dysgenesis (p < 0.001). Conclusions: This study enhances the current understanding of ocular comorbidities in IRDs in Portuguese patients. Common findings were cataract, refractive error, and CME. Stationary IRDs and pattern dystrophies showed fewer concomitant comorbidities, supporting their classification as non-progressive or benign conditions. The significance of registries like IRD-PT cannot be overstated, particularly in the context of rare diseases. These databases serve multiple crucial functions in enabling detailed documentation of disease characteristics and long-term monitoring of disease progression.
Five-Year Cumulative Incidence and Progression of Myopic Maculopathy in a German Population.
To investigate the 5-year cumulative incidence and progression of myopic maculopathy in the general population in Germany and to analyze potential risk factors. The Gutenberg Health Study (GHS) is a population-based cohort study including 15 010 participants aged 35 to 74 years at baseline. A total of 494 eyes of 323 participants (mean age, 50.2 ± 9.2 years; median, -7.25 diopters [D] myopic refractive error) without myopic maculopathy at baseline and 34 eyes of 27 subjects (mean age, 56.7 ± 9.1 years; median, -8.75 D myopic refractive error) with myopic maculopathy met the inclusion conditions, phakic eyes with spherical equivalent ≤-6 D (baseline), and had gradable fundus photographs at baseline and 5-year follow-up. Myopic maculopathy incidence and progression were assessed by grading of fundus photographs according to a recent international photographic classification system (META-PM). Multivariable logistic regression analysis was used to assess risk factors for progression of myopic maculopathy. Estimates for incidence and progression of myopic maculopathy. The 5-year cumulative incidence of myopic maculopathy was 0.3% (95% confidence interval [CI], 0.02-1.99; n = 1). Progression occurred in 17 of 34 eyes (50%) with prior myopic maculopathy over 5 years with 4 changes in category. The most common types of progression were enlargement of diffuse and patchy chorioretinal atrophy; a new pathology was present in 8 eyes. Higher intraocular pressure (IOP) (odds ratio [OR], 1.62; 95% CI, 1.51-1.59; P = 0.035) was associated with progression of myopic maculopathy. Female gender (OR, 5.54; 95% CI, 0.93-32.92; P = 0.060) and higher myopic refractive error (OR, 1.62 per diopter; 95% CI, 0.99-1.49; P = 0.063) showed a tendency toward progression. Incidence of myopic maculopathy is rare in highly myopic eyes in the general population aged 35 to 74 years in Germany. Progression of myopic maculopathy in the German population occurred in 50% of highly myopic eyes. We presented population-based 5-year follow-up data on incidence and progression of myopic maculopathy in Europe.
Intravitreal Ranibizumab for the Treatment of Visual Impairment Due to Choroidal Neovascularization Associated with Rare Diseases: Cost-Effectiveness in the UK.
This study sought to determine the cost-effectiveness of intravitreal ranibizumab compared with best supportive care (BSC; considered to be no active treatment) for the treatment of visual impairment due to choroidal neovascularization (CNV) associated with causes other than neovascular age-related macular degeneration (nAMD) and pathologic myopia (PM) in a UK setting. An individual patient-level simulation model was developed to estimate the lifetime costs and quality-adjusted life years (QALYs) of ranibizumab vs. BSC. Regression analyses, performed on patient-level data collected within the pivotal phase III MINERVA trial, modelled visual acuity (VA) progression while patients remained on treatment. Patient utilities were modelled as a function of VA in both eyes and resource use estimates were based on trial data or the literature. Costs were evaluated from the perspective of the UK National Health Service and personal social services, with future costs and health outcomes discounted at 3.5% per annum. Sensitivity and scenario analyses were conducted. The incremental cost-effectiveness ratio for intravitreal ranibizumab was £1363 per QALY compared to BSC and was associated with an incremental benefit of 1.06 QALYs and an incremental cost of £1444 per patient. Drug and administration costs of intravitreal ranibizumab were offset by the prevention of the development of blindness and its associated costs, while the increase in benefits was driven by a reduction in mortality risk and an improved health-related quality of life attributed to an improvement in VA. The findings were robust to a range of sensitivity analyses and ranibizumab consistently remained cost-effective at a willingness-to-pay threshold of £20,000-30,000 per QALY gained for all sensitivity analyses. Intravitreal ranibizumab is a highly cost-effective intervention for the treatment of CNV due to causes other than nAMD and PM as it delivers substantial QALY gains to patients while making cost savings vs. BSC. Novartis Pharmaceuticals UK Ltd.
Publicações recentes
Ver todas no PubMed📚 EuropePMCmostrando 3
Exploring Concomitant Ophthalmic Comorbidities in Portuguese Patients with Inherited Retinal Diseases: A Comprehensive Clinical Study.
GenesFive-Year Cumulative Incidence and Progression of Myopic Maculopathy in a German Population.
OphthalmologyIntravitreal Ranibizumab for the Treatment of Visual Impairment Due to Choroidal Neovascularization Associated with Rare Diseases: Cost-Effectiveness in the UK.
Advances in therapyAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para NÃO RARA NA EUROPA: Degeneração macular miópica.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para NÃO RARA NA EUROPA: Degeneração macular miópica
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Exploring Concomitant Ophthalmic Comorbidities in Portuguese Patients with Inherited Retinal Diseases: A Comprehensive Clinical Study.
- Five-Year Cumulative Incidence and Progression of Myopic Maculopathy in a German Population.
- Intravitreal Ranibizumab for the Treatment of Visual Impairment Due to Choroidal Neovascularization Associated with Rare Diseases: Cost-Effectiveness in the UK.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:178493(Orphanet)
- MONDO:0015807(MONDO)
- GARD:20153(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Q55785730(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar