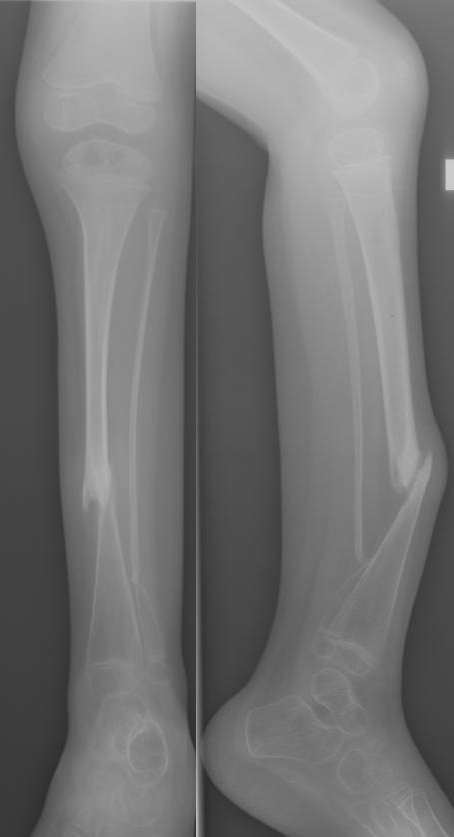
Pseudoartrose é uma séria complicação de uma fratura óssea na qual o osso nunca se regenera. Uma cicatriz de tecido fibroso se forma no meio do osso. Sem tratamento resulta em deformidade e prejuízo permanente da função, como por exemplo uma perna torta e incapaz de suportar peso se a pseudoartrose é no fêmur ou na tíbia. O tratamento é cirúrgico e a recuperação demora muitos meses.
Introdução
O que você precisa saber de cara
Condição rara de nascimento onde a tíbia não se forma corretamente, resultando em uma fratura congênita que falha em consolidar, formando uma "falsa articulação". Frequentemente associada à neurofibromatose tipo 1.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Pseudoartrose congênita da tíbia
Centros de Referência SUS
24 centros habilitados pelo SUS para Pseudoartrose congênita da tíbia
Centros para Pseudoartrose congênita da tíbia
Detalhes dos centros
Hospital Universitário Prof. Edgard Santos (HUPES)
R. Dr. Augusto Viana, s/n - Canela, Salvador - BA, 40110-060 · CNES 0003808
Serviço de Referência
Hospital Infantil Albert Sabin
R. Tertuliano Sales, 544 - Vila União, Fortaleza - CE, 60410-794 · CNES 2407876
Serviço de Referência
Hospital de Apoio de Brasília (HAB)
AENW 3 Lote A Setor Noroeste - Plano Piloto, Brasília - DF, 70684-831 · CNES 0010456
Serviço de Referência
Hospital Estadual Infantil e Maternidade Alzir Bernardino Alves (HIABA)
Av. Min. Salgado Filho, 918 - Soteco, Vila Velha - ES, 29106-010 · CNES 6631207
Serviço de Referência
Hospital das Clínicas da UFG
Rua 235 QD. 68 Lote Área, Nº 285, s/nº - Setor Leste Universitário, Goiânia - GO, 74605-050 · CNES 2338424
Serviço de Referência
Hospital Universitário da UFJF
R. Catulo Breviglieri, Bairro - s/n - Santa Catarina, Juiz de Fora - MG, 36036-110 · CNES 2297442
Atenção Especializada
Hospital das Clínicas da UFMG
Av. Prof. Alfredo Balena, 110 - Santa Efigênia, Belo Horizonte - MG, 30130-100 · CNES 2280167
Serviço de Referência
Hospital Universitário Julio Müller (HUJM)
R. Luis Philippe Pereira Leite, s/n - Alvorada, Cuiabá - MT, 78048-902 · CNES 2726092
Atenção Especializada
Hospital Universitário João de Barros Barreto
R. dos Mundurucus, 4487 - Guamá, Belém - PA, 66073-000 · CNES 2337878
Serviço de Referência
Hospital Universitário Lauro Wanderley (HULW)
R. Tabeliao Estanislau Eloy, 585 - Castelo Branco, João Pessoa - PB, 58050-585 · CNES 0002470
Atenção Especializada
Instituto de Medicina Integral Prof. Fernando Figueira (IMIP)
R. dos Coelhos, 300 - Boa Vista, Recife - PE, 50070-902 · CNES 0000647
Serviço de Referência
Hospital Pequeno Príncipe
R. Des. Motta, 1070 - Água Verde, Curitiba - PR, 80250-060 · CNES 3143805
Serviço de Referência
Hospital Universitário Regional de Maringá (HUM)
Av. Mandacaru, 1590 - Parque das Laranjeiras, Maringá - PR, 87083-240 · CNES 2216108
Atenção Especializada
Hospital de Clínicas da UFPR
R. Gen. Carneiro, 181 - Alto da Glória, Curitiba - PR, 80060-900 · CNES 2364980
Serviço de Referência
Hospital Universitário Pedro Ernesto (HUPE-UERJ)
Blvd. 28 de Setembro, 77 - Vila Isabel, Rio de Janeiro - RJ, 20551-030 · CNES 2280221
Serviço de Referência
Instituto Nacional de Saúde da Mulher, da Criança e do Adolescente Fernandes Figueira (IFF/Fiocruz)
Av. Rui Barbosa, 716 - Flamengo, Rio de Janeiro - RJ, 22250-020 · CNES 2269988
Serviço de Referência
Hospital São Lucas da PUCRS
Av. Ipiranga, 6690 - Jardim Botânico, Porto Alegre - RS, 90610-000 · CNES 2232928
Serviço de Referência
Hospital de Clínicas de Porto Alegre (HCPA)
Rua Ramiro Barcelos, 2350 Bloco A - Av. Protásio Alves, 211 - Bloco B e C - Santa Cecília, Porto Alegre - RS, 90035-903 · CNES 2237601
Serviço de Referência
Hospital Universitário da UFSC (HU-UFSC)
R. Profa. Maria Flora Pausewang - Trindade, Florianópolis - SC, 88036-800 · CNES 2560356
Serviço de Referência
Hospital das Clínicas da FMUSP
R. Dr. Ovídio Pires de Campos, 225 - Cerqueira César, São Paulo - SP, 05403-010 · CNES 2077485
Serviço de Referência
Hospital de Base de São José do Rio Preto
Av. Brg. Faria Lima, 5544 - Vila Sao Jose, São José do Rio Preto - SP, 15090-000 · CNES 2079798
Atenção Especializada
Hospital de Clínicas da UNICAMP
R. Vital Brasil, 251 - Cidade Universitária, Campinas - SP, 13083-888 · CNES 2748223
Serviço de Referência
Hospital de Clínicas de Ribeirão Preto (HCRP-USP)
R. Ten. Catão Roxo, 3900 - Vila Monte Alegre, Ribeirão Preto - SP, 14015-010 · CNES 2082187
Serviço de Referência
UNIFESP / Hospital São Paulo
R. Napoleão de Barros, 715 - Vila Clementino, São Paulo - SP, 04024-002 · CNES 2688689
Serviço de Referência
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Tibial lengthening in congenital pseudoarthrosis of the tibia: a scoping review.
Congenital pseudoarthrosis of the tibia (CPT) is a rare, sinister condition that is often associated with neurofibromatosis type 1 (NF1). Even after achieving union, patients frequently present with significant leg length discrepancy (LLD) due to growth disturbance and repeated reconstructive surgeries. Tibial lengthening using distraction osteogenesis is commonly performed, yet outcomes and complications remain poorly understood. To systematically map the available literature on tibial lengthening in CPT, describe surgical techniques, summarize reported outcomes, and identify research gaps. A scoping review was conducted following Arksey and O'Malley's framework and the PRISMA-ScR guidelines. The PubMed, Embase, Scopus, Web of Science and Cochrane Library databases were searched. Eligible studies included those reporting tibial lengthening during CPT. Data on patient demographics, surgical techniques, length achieved, union rates, complications, and follow-up were extracted. Thirty-one studies involving 486 patients were included. All studies were retrospective. The mean age at lengthening ranged from 3.2 to 33.7 years. NF1 was present in 70% of the patients. The Ilizarov external fixator in isolation or with hybrid techniques was the most frequently reported lengthening modality. The mean lengthening achieved was 5.5 cm (range 1.5-10.2 cm). The most common site of lengthening was through proximal tibial osteotomy followed by physeal distraction. Complications such as pin tract infection, regenerate fractures and tibial bowing deformities were commonly encountered. The follow-up period ranged from 1.6 to 24 years. Tibial lengthening is feasible in CPT and can achieve meaningful limb length equalization. However, complication rates remain high, and evidence is limited by the small number of retrospective studies. Standardized outcome reporting and prospective multicenter collaboration are needed to optimize care.
Development of the Extended Lane and Sandu Score to Assess Osseous Repair.
Lane and Sandhu introduced a radiological score to evaluate bone union in animal and human models after experimental bone grafting. We introduce an extension of the Lane and Sandhu Scoring system to serve as a more granular system for robust bone healing assessment in clinical research. We describe the application of this scoring system in the context of an autologous cell-based osteogenic implant (NVD003) designed to improve the rate of bone union. Images from four participants with congenital pseudoarthrosis of the tibia (CPT) and 9 adults with recurrent osseous non-union after conventional surgery were obtained. All participants underwent NVD003 implantation. An extended version of the Lane and Sandhu scoring system (eLSS; range from 0 to 12) was employed to assess bone formation, union, and remodeling by two independent readers longitudinally, with final adjudication in cases of > 1 point disagreement. Interobserver agreement was assessed using quadratic weighted kappa. 206 exams (170 radiographs and 36 CT scans) were studied across the two pathologies (81 scans for participants with CPT and 125 scans for participants with recurrent osseous non-union). Overall agreement between the expert readers was found to be 0.84 (95% CI: 0.79, 0.89), with comparable agreement found per modality (radiographs [0.85] and CT images [0.76]) and per pathology (CPT [0.83] and recurrent osseous non-union [0.84]). These results support that the eLSS has sufficient reliability to warrant further consideration for clinical trial use. Additional studies with a greater number of subjects, raters, and variety of use cases are required to validate and optimize this method. Level of Evidence: III.
Unraveling the molecular landscape of congenital pseudoarthrosis of the tibia: insights from a comprehensive analysis of 159 probands.
Congenital pseudarthrosis of the tibia (CPT, HP:0009736), commonly known as bowing of the tibia, is a rare congenital tibia malformation characterized by spontaneous tibial fractures and difficulty in reunion after tibial fractures during early childhood, with a prevalence between 1/250,000 and 1/140,000. While 80%-84% of CPT cases present with neurofibromatosis type 1, caused by the variations in the NF1 gene, the underlying cause of CPT remains unclear. Considering its congenital nature and the low prevalence, we hypothesized that the rare genomic protein-damaging variations may contribute to CPT. In this study, we conducted whole exome sequencing on 159 patients with CPT and found loss-of-function (LoF) excesses in the 159 patient cases compared to 208 healthy controls from the 1000 Genomes Project. The LoF variant types primarily included stop-gained and frameshift variants, both present in 97% of the 159 patients with CPT, as well as splice-changing variants, which were found in 78% of these patients. Rare LoF variations in osteocyte-related pathways, such as ossification, were identified in 112 of the 159 CPT cases (70.4%). The top seven genes carrying rare protein-damaging variants that might be related to CPT are NF1, GLI3, MRC2, PTH1R, RYR1, NPR2 and ITGA11. These findings shed light on novel genetic mutations and osteocyte transcriptome-related molecular pathways involved in CPT, providing a new framework for understanding the genetic regulation of CPT pathology and suggesting potential directions to further elucidate its pathogenesis.
Vascularized Periosteal Grafts for Bone Union in Children: A Systematic Review.
The periosteum is the main organ responsible for bone regeneration. Vascularized Periosteal Grafts (VPG) have demonstrated exceptional efficacy and speed in facilitating bone union among children with challenging bone healing conditions. Despite their promising results, the overall impact of these interventions has yet to be comprehensively evaluated through systematic review. This systematic review aimed to provide comprehensive insights into bone union outcomes and complications related to the use of VPG in children. MEDLINE/PubMed, Embase, Web of Science, Clinicaltrials.gov, and Cochrane Library were searched from database inception to September 2023 and screened for relevant studies. Data were collected regarding patient demographics, disease, treatment, anatomical location, graft used, donor and receptor vessels, skin paddle monitoring, follow-up duration, time to union, consolidation, and complications. The correlation between age and bone union was assessed using Pearson and Spearman correlation coefficients, as appropriate. Study quality was assessed using the Methodological Index for Non-randomized Studies Criteria. A total of 15 studies involving 135 patients were included. All the studies were classified as Level 4 evidence. The mean MINORS score was 5.1 ± 1. The aim of the VPG was nonunion treatment in 90 patients (67%), nonunion prevention in 35 patients (26%), and bone union acceleration in 10 patients (7%). The origin of the bone union problem was traumatic in 59 cases (44%), congenital pseudoarthrosis of the tibia or fibula in 48 patients (35%), oncologic in 23 patients (17%), and infectious in 5 patients (4%). Nine different sources of periosteal flaps were used to enhance bone union. Bone union rate was 96% with a mean time of 4.2 months (range 1-18 months). Spearman test showed a non-statistically significant negative correlation between age and bone union time (r = -0.3, p = 0.759). VPGs are a safe and reliable treatment for promoting bone union, especially in the context of complex pediatric bone-healing challenges.
Paley cross union protocol for congenital pseudoarthrosis of the tibia.
Congenital pseudarthrosis of the tibia (CPT) is a rare, dysplastic condition causing significant disability in the lower limbs. A treatment aims to achieve long-lasting union, prevent limb length discrepancies, and prevent soft tissue lesions. Traditional surgery often yields satisfactory results, but amputation may be proposed in failed cases. This report presents a congenital pseudarthrosis of the tibia and fibula, treated with the Paley cross-union protocol. A 15-month-old girl presented with a crooked right lower leg at the age of two months, history of a right lower leg fracture at the age of eight months, and pain when moving her leg. She had undergone an initial surgical procedure to maintain tibia alignment with K-Wire insertion and was cast at a private hospital. The patient's physical examination showed a cast causing limited range of motion, but no tenderness or distal neurovascular issues. The Paley cross-union protocol was performed, involving anterior approach, curettage, and insertion of a titanium intramedullary elastic nail into the tibia. The fracture site area was covered with a meshed periosteum layer and filled with synthetic bone grafts. A long leg cast was performed after the procedure. An imaging examination post-cross-union protocol showed a good result. Cross-union for CPT represents a paradigm shift in the treatment of this horrible child disease. Given the promising result, the cross-union approach has to be regarded as a fresh criterion for treating CPT.
Publicações recentes
Tibial lengthening in congenital pseudoarthrosis of the tibia: a scoping review.
Development of the Extended Lane and Sandu Score to Assess Osseous Repair.
Unraveling the molecular landscape of congenital pseudoarthrosis of the tibia: insights from a comprehensive analysis of 159 probands.
Vascularized Periosteal Grafts for Bone Union in Children: A Systematic Review.
Paley cross union protocol for congenital pseudoarthrosis of the tibia.
📚 EuropePMC46 artigos no totalmostrando 30
Tibial lengthening in congenital pseudoarthrosis of the tibia: a scoping review.
BMC musculoskeletal disordersDevelopment of the Extended Lane and Sandu Score to Assess Osseous Repair.
Journal of orthopaedic research : official publication of the Orthopaedic Research SocietyUnraveling the molecular landscape of congenital pseudoarthrosis of the tibia: insights from a comprehensive analysis of 159 probands.
Orphanet journal of rare diseasesVascularized Periosteal Grafts for Bone Union in Children: A Systematic Review.
MicrosurgeryPaley cross union protocol for congenital pseudoarthrosis of the tibia.
Medicinski glasnik : official publication of the Medical Association of Zenica-Doboj Canton, Bosnia and HerzegovinaBilateral congenital pseudoarthrosis of the tibia: A case report and literature review.
Journal of clinical orthopaedics and traumaIlizarov Distraction for Congenital Pseudoarthrosis of the Tibia in Adults.
Orthopaedic surgeryFree Fibula Flap for Congenital Pseudarthrosis of the Tibia: Indications and Challenges.
JPRAS openOsteogenic organoid for bone regeneration: Healing of bone defect in congenital pseudoarthrosis of the tibia.
The International journal of artificial organsManagement of congenital pseudoarthrosis using Ilizarov Device-Delsuth, oghara experience.
Nigerian journal of clinical practiceTreatment of Refractory Congenital Pseudoarthrosis of Tibia with Contralateral Vascularized Fibular Bone Graft and Anatomic Distal Tibial Locking Plate: A Case Series and Literature Review.
Children (Basel, Switzerland)Umbilical cord mesenchymal stem cells combined with secretome for treating congenital pseudarthrosis of the Tibia: a case series.
European journal of orthopaedic surgery & traumatology : orthopedie traumatologieCongenital Pseudoarthrosis of the Tibia: A Narrative Review.
CureusEXPERIMENTAL STUDY OF BONE DENSITY IN PATIENTS WITH CONGENITAL PSEUDOARTHROSIS OF THE TIBIA BEFORE AND AFTER SURGERY.
Wiadomosci lekarskie (Warsaw, Poland : 1960)Anterolateral Tibial Bowing and Congenital Pseudoarthrosis of the Tibia: Current Concept Review and Future Directions.
Current reviews in musculoskeletal medicineCombination of the Ilizarov Method and Intramedullary Fixation for the Treatment of Congenital Pseudarthrosis of the Tibia in Children: A Retrospective Observational Study.
Frontiers in surgeryEvaluation of the efficacy of ipsilateral fibular transfer for reconstruction of large tibial defects in children: a retrospective study.
Journal of orthopaedic surgery and researchSuccess Story of Ilizarov in Chronic Non-union of Tibia with 18 Years of Morbidity: A Case Report.
Journal of orthopaedic case reportsCross-Union Surgery for Congenital Pseudarthrosis of the Tibia.
Children (Basel, Switzerland)Effectiveness of bone marrow aspirate concentrate (BMAC) as adjuvant therapy in the surgical treatment of congenital pseudoarthrosis of the tibia: a retrospective comparative study.
Journal of biological regulators and homeostatic agentsDiagnostic and treatment challenge in adult presentation of congenital pseudoarthrosis of the tibia: A case report.
Annals of medicine and surgery (2012)Management of Congenital Pseudoarthrosis of the Tibia and Fibula.
Current reviews in musculoskeletal medicineEvaluation of bone marrow-derived mesenchymal stem cell quality from patients with congenital pseudoarthrosis of the tibia.
Journal of orthopaedic surgery and researchAnterolateral Bowing of Congenital Pseudoarthrosis of Tibia Treated by Percutaneous Osteotomy and Gradual Correction Using Taylor Spatial Frame, then Late Insertion of a Fussier-Duval Nail: A Case Report.
The American journal of case reportsPedicled Sensate Composite Calcaneal Flap in Children With Congenital Tibial Pseudoarthrosis.
Journal of pediatric orthopedicsFailure of tension band plating: a case series.
Journal of pediatric orthopedics. Part B[Utility of morphogenetic protein for the treatment of congenital pseudoarthrosis of the tibia].
Acta ortopedica mexicana[Versatility of the microvascular fibular flap in limb reconstruction].
Cirugia y cirujanosComputational modeling of bone fracture non-unions: four clinically relevant case studies.
In silico cell and tissue scienceIsolation and Characterization of Multipotential Mesenchymal Stromal Cells from Congenital Pseudoarthrosis of the Tibia: Case Report.
Anatomical record (Hoboken, N.J. : 2007)Associações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Pseudoartrose congênita da tíbia.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Pseudoartrose congênita da tíbia
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Ainda não achamos doenças com sintomas parecidos o suficiente.
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Tibial lengthening in congenital pseudoarthrosis of the tibia: a scoping review.
- Development of the Extended Lane and Sandu Score to Assess Osseous Repair.Journal of orthopaedic research : official publication of the Orthopaedic Research Society· 2026· PMID 41472555mais citado
- Unraveling the molecular landscape of congenital pseudoarthrosis of the tibia: insights from a comprehensive analysis of 159 probands.
- Vascularized Periosteal Grafts for Bone Union in Children: A Systematic Review.
- Paley cross union protocol for congenital pseudoarthrosis of the tibia.Medicinski glasnik : official publication of the Medical Association of Zenica-Doboj Canton, Bosnia and Herzegovina· 2024· PMID 39526728mais citado
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:295018(Orphanet)
- MONDO:0017462(MONDO)
- GARD:21203(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Q15824114(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar