A deficiência de galactose epimerase é uma forma muito rara de galactosemia, que pode ser de moderada a grave, caracterizada por sinais de moderados a graves de dificuldade no metabolismo da galactose.
Introdução
O que você precisa saber de cara
A deficiência de galactose epimerase é uma forma muito rara de galactosemia, que pode ser de moderada a grave, caracterizada por sinais de moderados a graves de dificuldade no metabolismo da galactose.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 10 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 24 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
1 gene identificado com associação a esta condição. Padrão de herança: Autosomal recessive.
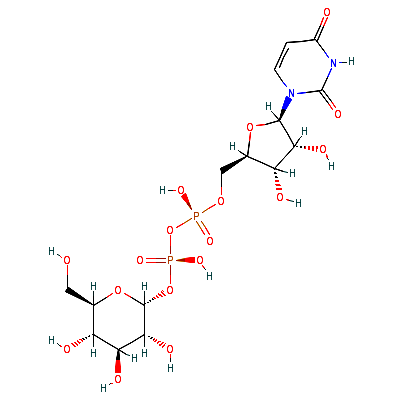
Catalyzes two distinct but analogous reactions: the reversible epimerization of UDP-glucose to UDP-galactose and the reversible epimerization of UDP-N-acetylglucosamine to UDP-N-acetylgalactosamine. The reaction with UDP-Gal plays a critical role in the Leloir pathway of galactose catabolism in which galactose is converted to the glycolytic intermediate glucose 6-phosphate. It contributes to the catabolism of dietary galactose and enables the endogenous biosynthesis of both UDP-Gal and UDP-GalNA
Galactosemia 3
A form of galactosemia, an inborn error of galactose metabolism typically manifesting in the neonatal period, after ingestion of galactose, with jaundice, hepatosplenomegaly, hepatocellular insufficiency, food intolerance, hypoglycemia, renal tubular dysfunction, muscle hypotonia, sepsis and cataract. GALAC3 is an autosomal recessive form caused by galactose epimerase deficiency. It can manifest as benign, peripheral form with mild symptoms and enzymatic deficiency in circulating blood cells only. A second form, known as generalized epimerase deficiency, is characterized by undetectable levels of enzyme activity in all tissues and severe clinical features, including restricted growth and intellectual disability.
Variantes genéticas (ClinVar)
89 variantes patogênicas registradas no ClinVar.
Vias biológicas (Reactome)
2 vias biológicas associadas aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Deficiência de UDP-galactose-4-epimerase
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Galactose epimerase deficiency: lessons from the GalNet registry.
Galactose epimerase (GALE) deficiency is a rare hereditary disorder of galactose metabolism with only a few cases described in the literature. This study aims to present the data of patients with GALE deficiency from different countries included through the Galactosemia Network to further expand the existing knowledge and review the current diagnostic strategy, treatment and follow-up of this not well characterized entity. Observational study collecting medical data from December 2014 to April 2022 of 22 not previously reported patients from 14 centers in 9 countries. Patients were classified as generalized or non-generalized based on their genotype, enzyme activities in different tissues and/or clinical picture and professional judgment of the treating physician. In total 6 patients were classified as generalized and 16 as non-generalized. In the generalized group, acute neonatal illness was reported in 3, cognitive and developmental delays were present in 5 and hearing problems were reported in 3. Four generalized patients were homozygous for the genetic variant NM_001008216.2:c.280G > A (p.Val94Met). In the non-generalized group, no clearly related symptoms were found. Ten novel genetic variants were reported in this study population. The phenotypic spectrum of GALE deficiency ranges from asymptomatic to severe. The generalized patients have a phenotype that is in line with the 9 described cases in the literature and prescribing dietary interventions is the cornerstone for treatment. In the non-generalized group, treatment advice is more difficult. To be able to offer proper counseling, in addition to red blood cell enzyme activity, genetic studies, transferrin glycoform analysis and enzymatic measurements in fibroblasts are recommended. Due to lack of facilities, additional enzymatic testing is not common practice in many centers nor a tailored long-term follow-up is performed.
Molecular dynamics, residue network analysis, and cross-correlation matrix to characterize the deleterious missense mutations in GALE causing galactosemia III.
Epimerase-deficiency galactosemia (EDG) is caused by mutations in the UDP-galactose 4'-epimerase enzyme, encoded by gene GALE. Catalyzing the last reaction in the Leloir pathway, UDP-galactose-4-epimerase catalyzes the interconversion of UDP-galactose and UDP-glucose. This study aimed to use in-depth computational strategies to prioritize the pathogenic missense mutations in GALE protein and investigate the systemic behavior, conformational spaces, atomic motions, and cross-correlation matrix of the GALE protein. We searched four databases (dbSNP, ClinVar, UniProt, and HGMD) and major biological literature databases (PubMed, Science Direct, and Google Scholar), for missense mutations that are associated with EDG patients, our search yielded 190 missense mutations. We applied a systematic computational prediction pipeline, including pathogenicity, stability, biochemical, conservational, protein residue contacts, and structural analysis, to predict the pathogenicity of these mutations. We found three mutations (p.K161N, p.R239W, and p.G302D) with a severe phenotype in patients with EDG that correlated with our computational prediction analysis; thus, they were selected for further structural and simulation analyses to compute the flexibility and stability of the mutant GALE proteins. The three mutants were subjected to molecular dynamics simulation (MDS) with native protein for 200 ns using GROMACS. The MDS demonstrated that these mutations affected the beta-sheets and helical region that are responsible for the catalytic activity; subsequently, affects the stability and flexibility of the mutant proteins along with a decrease and more deviations in compactness when compared to that of a native. Also, three mutations created major variations in the combined atomic motions of the catalytic and C-terminal regions. The network analysis of the residues in the native and three mutant protein structures showed disturbed residue contacts occurred owing to the missense mutations. Our findings help to understand the structural behavior of a protein owing to mutation and are intended to serve as a platform for prioritizing mutations, which could be potential targets for drug discovery and development of targeted therapeutics.
Expansion of the clinical phenotype of GALE deficiency.
Congenital disorders of glycosylation are a group of rare monogenic inborn errors of metabolism caused by defective glycoprotein and glycolipid glycan synthesis and attachment. Here, we present a patient with galactose epimerase deficiency, also known as GALE deficiency, accompanied by pancytopenia and immune dysregulation. She was first identified by an abnormal newborn screen for galactosemia with subsequent genetic evaluation due to pancytopenia and immune dysregulation. The evaluation ultimately revealed that her known diagnosis of GALE deficiency was the cause of her hematologic and immune abnormalities. These findings further expand the clinical spectrum of disease of congenital disorders of glycosylation.
Screening for galactosemia: is there a place for it?
Galactose is a hexose essential for production of energy, which has a prebiotic role and is essential for galactosylation of endogenous and exogenous proteins, ceramides, myelin sheath metabolism and others. The inability to metabolize galactose results in galactosemia. Galactosemia is an autosomal recessive disorder that affects newborns who are born asymptomatic, apparently well and healthy, then develop serious morbidity and mortality upon consuming milk that contains galactose. Those with galactosemia have a deficiency of an enzyme: classic galactosemia (type 1) results from severe deficiency of galactose-1-uridylyltransferase, while galactosemia type II results from galactokinase deficiency and type III results from galactose epimerase deficiency. Many countries include neonatal screening for galactosemia in their national newborn screening program; however, others do not, as the condition is rather rare, with an incidence of 1:30,000-1:100,000, and screening may be seen as not cost-effective and logistically demanding. Early detection and intervention by restricting galactose is not curative but is very rewarding, as it prevents deaths, mental retardation, liver cell failure, renal tubular acidosis and neurological sequelae, and may lead to resolution of cataract formation. Hence, national newborn screening for galactosemia prevents serious potential life-long suffering, morbidity and mortality. Recent advances in communication and biotechnology promise facilitation of logistics of neonatal screening, including improved cost-effectiveness.
Galactose Epimerase Deficiency: Expanding the Phenotype.
Galactose epimerase deficiency is an inborn error of metabolism due to uridine diphosphate-galactose-4'-epimerase (GALE) deficiency. We report the clinical presentation, genetic and biochemical studies in two siblings with generalized GALE deficiency.Patient 1: The first child was born with a dysmorphic syndrome. Failure to thrive was noticed during the first year. Episodes of heart failure due to dilated cardiomyopathy, followed by liver failure, occurred between 12 and 42 months. The finding of a serum transferrin isoelectrofocusing (IEF) type 1 pattern led to the suspicion of a congenital disorder of glycosylation (CDG). Follow-up disclosed psychomotor disability, deafness, and nuclear cataracts.Patient 2: The sibling of patient 1 was born with short limbs and hip dysplasia. She is deceased in the neonatal period due to intraventricular hemorrhage in the context of liver failure. Investigation disclosed galactosuria and normal transferrin glycosylation.Next-generation sequence panel analysis for CDG syndrome revealed the previously reported c.280G>A (p.[V94M]) homozygous mutation in the GALE gene. Enzymatic studies in erythrocytes (patient 1) and fibroblasts (patients 1 and 2) revealed markedly reduced GALE activity confirming generalized GALE deficiency. This report describes the fourth family with generalized GALE deficiency, expanding the clinical spectrum of this disorder, since major cardiac involvement has not been reported before.
Publicações recentes
Galactose epimerase deficiency: lessons from the GalNet registry.
Expansion of the clinical phenotype of GALE deficiency.
Molecular dynamics, residue network analysis, and cross-correlation matrix to characterize the deleterious missense mutations in GALE causing galactosemia III.
Screening for galactosemia: is there a place for it?
Galactose Epimerase Deficiency: Expanding the Phenotype.
📚 EuropePMC2 artigos no totalmostrando 5
Galactose epimerase deficiency: lessons from the GalNet registry.
Orphanet journal of rare diseasesExpansion of the clinical phenotype of GALE deficiency.
American journal of medical genetics. Part AMolecular dynamics, residue network analysis, and cross-correlation matrix to characterize the deleterious missense mutations in GALE causing galactosemia III.
Cell biochemistry and biophysicsScreening for galactosemia: is there a place for it?
International journal of general medicineGalactose Epimerase Deficiency: Expanding the Phenotype.
JIMD reportsAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Deficiência de UDP-galactose-4-epimerase.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Deficiência de UDP-galactose-4-epimerase
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Galactose epimerase deficiency: lessons from the GalNet registry.
- Molecular dynamics, residue network analysis, and cross-correlation matrix to characterize the deleterious missense mutations in GALE causing galactosemia III.
- Expansion of the clinical phenotype of GALE deficiency.
- Screening for galactosemia: is there a place for it?
- Galactose Epimerase Deficiency: Expanding the Phenotype.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:79238(Orphanet)
- OMIM OMIM:230350(OMIM)
- MONDO:0009257(MONDO)
- GARD:5392(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Q17153517(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar