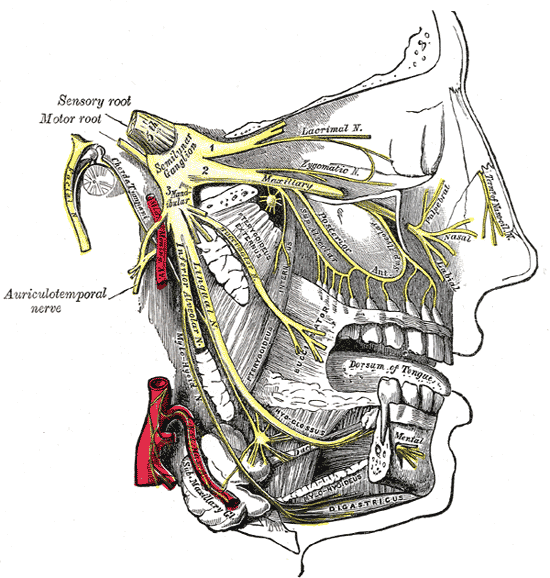
Neuralgia que envolve o feixe de projeção do neurônio craniano.
Introdução
O que você precisa saber de cara
Neuralgia que envolve o feixe de projeção do neurônio craniano.
Tem tratamento?
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 25 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 40 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Neuralgia craniana
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
0 ensaios clínicos encontrados.
Publicações mais relevantes
Reprogramming activated astrocytes into GABAergic neurons to treat trigeminal neuralgia.
Trigeminal neuralgia (TN) is the most common type of cranial neuralgia. Currently, there remains a significant gap in the availability of effective and safe treatment options in clinical practice. Transdifferentiation of proliferating activated astrocytes into inhibitory neurons is a potential therapeutic strategy for central nervous system diseases. GABAergic neurons are one of the most type of prevalent inhibitory neurons. This study aims to reprogram proliferating astrocytes in the spinal trigeminal subnucleus caudalis (SpVc) into GABAergic neurons, could improve neuronal excitation-inhibition balance, alleviate pain, which serve as a potential treatment for trigeminal neuralgia. A chronic constriction injury of the distal infraorbital nerve (CCI-dION) was induced in the infraorbital branch of the trigeminal nerve to create a rat model of TN. Adeno-associated viruses were used to overexpress transcription factors Sox2 and Mash1 in astrocytes. The changes in astrocytes and GABAergic neurons in the SpVc region were detected by immunofluorescence, Western blotting, qPCR, and electron microscopy. The mechanical pain threshold testing was used to assess rat TN. In the SpVc region of CCI-dION rats, astrocytes showed proliferation and activation, and the number of GABAergic neurons decreased significantly. Overexpressing Sox2 and Mash1 in astrocytes led to a significant transdifferentiation into GABAergic neurons, which - improved the mechanical pain threshold in CCI-dION rats. Furthermore, fluorocitrate-mediated astrocyte deactivation abolished both the neuronal reprogramming and the analgesic effects, underscoring the essential role of astrocytes in this process. These findings suggest that overexpressing Sox2 and Mash1 in astrocytes led to a significant transdifferentiation into GABAergic neurons, which significantly improved the mechanical pain threshold in CCI-dION rats. Thus, this approach has the potential to provide a new treatment for TN.
Efficacy of Greater Occipital Nerve Blockade in Craniofacial Neuralgia and Facial Pain Syndromes: A Retrospective Chart Review with Prospectively Collected Follow-Up Data.
Background/Objectives: Greater occipital nerve blockade (GONB) is a minimally invasive intervention used to treat primary headaches. However, the evidence regarding its role in craniofacial pain syndromes and its potential impact on analgesic use remains limited. Previous studies have reported that GONB is an effective method in patients with cranial neuralgia, but its efficacy is limited in persistent idiopathic facial pain (PIFP). Methods: This study was a retrospective cohort trial examining the medical records of 26 patients who applied to our Headache Clinic due to facial pain and cranial neuralgia between April 2023 and April 2025. Of these patients, 12 were trigeminal neuralgia (46%), 6 were occipital neuralgia (23%), 4 were trigeminal neuropathic pain (15%), and 4 were PIFP (15%) patients. In our study, the landmark-based GONB technique was used to determine the greatest tenderness to palpation (TTP) area. A standard 2.5 mL mixture of 30 mg 2% lidocaine and 4 mg dexamethasone was injected bilaterally as a single dose into the nerve region of all patients. After GONB, all patients were routinely contacted by phone or addressed face to face once a week for the first month and monthly thereafter, and medical changes were recorded with a standard-case follow-up form file. The case follow-up form allowed regular monitoring of parameters, such as the Visual Analog Scale (VAS), self-assessment scales for patients' clinical responses, sensitivity to triggers, possible side effects, duration of effect, and the number of analgesics used. Results: A positive response with at least 50% overall improvement compared to the patient's baseline level was found in 22 of 26 patients. Response to treatment was observed in 10 patients in the trigeminal neuralgia group (83%), 3 patients in the trigeminal neuropathic pain (75%) and PIFP groups (75%), and all in the occipital neuralgia group (100%). There was no statistically significant difference in response rates between the diagnostic groups. A significant difference was found in terms of response rates according to gender (p = 0.022). Accordingly, while response was observed in all 15 female patients, response was observed in 7 of 11 male patients (64%). Pre-GONB VAS values of those responding to treatment were found to be higher. Patients with positive responses to GONB had a significantly higher median value of the VAS total score (5; 95% CI: 1.83-4.52) in comparison to those with negative responses (8.32; 95% CI: 8.17-12.12) (p < 0.001). Post-GONB Intensity (VAS) and Post-GONB sensitivity to triggers decreased significantly (p < 0.001, p < 0.001). In those who responded, the decrease in analgesic use after GONB compared to before was statistically significant in the first and second months (p < 0.001, p < 0.003, respectively). Although the decrease continued in the third month, this difference did not reach statistical significance (p = 0.551). Conclusions: GONB reduces the duration, frequency, and intensity of headaches, and the need for acute analgesic use in CN and PIFP patients.
DRESS Syndrome with Cold Agglutinins: An Unusual Immune Response to Anticonvulsants.
DRESS (Drug Reaction with Eosinophilia and Systemic Symptoms) is a rare adverse drug reaction characterized by cutaneous and systemic manifestations, with a mortality rate of up to 10%. In this study, we describe the case of a 77-year-old man who developed DRESS syndrome with cold agglutination. A 77-year-old man prescribed phenytoin and carbamazepine for suspected cranial neuralgia after a tooth extraction developed high-grade fever and hemorrhagic crusting on the upper and lower lips and oral mucosa, morbilliform rashes over the chest, abdomen, and back along with facial edema, all occurring over 2 weeks. Clinically significant right-sided submandibular, cervical, and axillary lymphadenopathy was observed. Additional findings, including peripheral blood eosinophilia, hepatitis, and coagulopathy, helped us make a provisional diagnosis of DRESS syndrome. The peripheral blood smear showed an incidental finding of cold agglutination phenomenon at room temperature (16 °C; winter months in North India), which disappeared under warmer conditions. However, gross hemolysis was not confirmed. The patient showed significant response in both clinical and hematological parameters within 24 hours of initiating intravenous dexamethasone, which was continued and gradually tapered over 14 days. Follow-up at one month showed the disappearance of the cold agglutination phenomenon. Cold agglutination in DRESS syndrome has not been documented in detail in the past. One hypothesis is the agglutination of red blood cells (RBCs) due to the effect of the pathogenetic antibodies in DRESS syndrome directed against RBC antigens. Further molecular research may elucidate the pathways of this rare clinical finding.
Efficacy of Botulinum Toxin Injection via Coronoid Approach in Refractory Trigeminal Neuralgia: A Case Report and Literature Review.
Trigeminal neuralgia (TN) is a well-characterized form of cranial neuralgia that affects one or more divisions of the trigeminal nerve. The first-line treatment for TN is pharmacotherapy, though over 40% of patients may become refractory to medication or experience intolerable side effects. A Gasserian ganglion block is a minimally invasive procedure aimed at alleviating TN symptoms and reducing the reliance on pharmacotherapy. We present a case of TN that was refractory to 2 times Gasserian ganglion block. While botulinum toxin has been effectively used in various nerve blocks, we opted to manage the patient's TN by targeting the peripheral mandibular nerve (V3) via a coronoid approach by using botulinum toxin injection. Our patient experienced 5 months' considerable pain relief, which demonstrates that the V3 injection of botulinum toxin may offer a viable alternative for managing refractory TN.
Atypical presentation of herpes zoster with cranial neuralgia and nodular skin lesions, a case report.
Publicações recentes
Reprogramming activated astrocytes into GABAergic neurons to treat trigeminal neuralgia.
Efficacy of Greater Occipital Nerve Blockade in Craniofacial Neuralgia and Facial Pain Syndromes: A Retrospective Chart Review with Prospectively Collected Follow-Up Data.
DRESS Syndrome with Cold Agglutinins: An Unusual Immune Response to Anticonvulsants.
Efficacy of Botulinum Toxin Injection via Coronoid Approach in Refractory Trigeminal Neuralgia: A Case Report and Literature Review.
📚 EuropePMC11 artigos no totalmostrando 31
Reprogramming activated astrocytes into GABAergic neurons to treat trigeminal neuralgia.
Neurochemistry internationalEfficacy of Greater Occipital Nerve Blockade in Craniofacial Neuralgia and Facial Pain Syndromes: A Retrospective Chart Review with Prospectively Collected Follow-Up Data.
Journal of clinical medicineDRESS Syndrome with Cold Agglutinins: An Unusual Immune Response to Anticonvulsants.
Current drug safetyEfficacy of Botulinum Toxin Injection via Coronoid Approach in Refractory Trigeminal Neuralgia: A Case Report and Literature Review.
Pain medicine case reportsAtypical presentation of herpes zoster with cranial neuralgia and nodular skin lesions, a case report.
Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology[Concomitant, asynchronous and refractory trigeminal and glossopharyngeal neuralgia. Good response to surgical approach in one time].
Revista de neurologiaFluoroscopic Analysis of Cannula Tip Location During Radiofrequency Thermocoagulation of the Trigeminal Ganglion.
Pain physicianSensitivity of the SNNOOP10 list in the high-risk secondary headache detection.
Cephalalgia : an international journal of headacheImaging of Cranial Neuralgias.
Neurologic clinicsSuspected Recurrence of Cranial Neuralgia Following Infection With SARS-CoV-2: A Case Report.
Integrative medicine (Encinitas, Calif.)Imaging predictors of successful surgical treatment of hemifacial spasm.
Brain communicationsCase Report: Direct Visualization of the Nervus Intermedius During the Microvascular Decompression Procedure: Should We Take It Seriously?
Frontiers in neurologyThe Diagnosis and Management of Posttraumatic Headache with Associated Painful Cranial Neuralgias: a Review and Case Series.
Current pain and headache reportsParoxysmal otalgia treated with microvascular decompression of the intermediate nerve: illustrative case.
Journal of neurosurgery. Case lessonsPrevalence and severity of neurovascular compression in hemifacial spasm patients.
Brain : a journal of neurologyFacial Pain: A Comprehensive Review and Proposal for a Pragmatic Diagnostic Approach.
European neurologyPearls for Interpreting Neurosurgical Systematic Reviews and Meta-Analyses: Lessons From a Collaborative Effort.
NeurosurgeryRecurrent painful ophthalmoplegic neuropathy: MRI findings in 2 patients.
Radiology case reportsOccipital Neuralgia and Cervicogenic Headache: Diagnosis and Management.
Current neurology and neuroscience reportsFacial pain: sinus or not?
Acta otorhinolaryngologica Italica : organo ufficiale della Societa italiana di otorinolaringologia e chirurgia cervico-faccialeShort-Lasting Unilateral Neuralgiform Headache Attacks.
Annals of Indian Academy of Neurology[Nummular headache : Subcutaneous peripheral nerve field stimulation as an individual therapeutic attempt].
Schmerz (Berlin, Germany)Treatment of Facial Pain with I Ching Balance Acupuncture.
Medical acupunctureTrigeminal Neuralgia: Toward a Multimodal Approach.
World neurosurgeryEslicarbazepine acetate for neuropathic pain, headache, and cranial neuralgia: Evidence and experience.
NeurologiaLacrimal Nerve Blocks for Three New Cases of Lacrimal Neuralgia.
HeadacheA Cross-Sectional Clinic-Based Study in Patients With Side-Locked Unilateral Headache and Facial Pain.
HeadacheLinear headache: clinical characteristics of eight new cases.
SpringerPlusMicrovascular decompression of the posterior inferior cerebellar artery for intermediate nerve neuralgia.
Surgical neurology internationalCranial neuralgia vs entrapment neuropathy decompression … better names than migraine trigger site deactivation surgery.
Headache[Herpes zoster-induced neuralgia (neuropathy)].
Terapevticheskii arkhivAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Neuralgia craniana.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Neuralgia craniana
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Reprogramming activated astrocytes into GABAergic neurons to treat trigeminal neuralgia.
- Efficacy of Greater Occipital Nerve Blockade in Craniofacial Neuralgia and Facial Pain Syndromes: A Retrospective Chart Review with Prospectively Collected Follow-Up Data.
- DRESS Syndrome with Cold Agglutinins: An Unusual Immune Response to Anticonvulsants.
- Efficacy of Botulinum Toxin Injection via Coronoid Approach in Refractory Trigeminal Neuralgia: A Case Report and Literature Review.
- Atypical presentation of herpes zoster with cranial neuralgia and nodular skin lesions, a case report.Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology· 2024· PMID 38353848mais citado
- Cranial Neuralgias.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:221109(Orphanet)
- MONDO:0016374(MONDO)
- GARD:20542(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Q56013819(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar