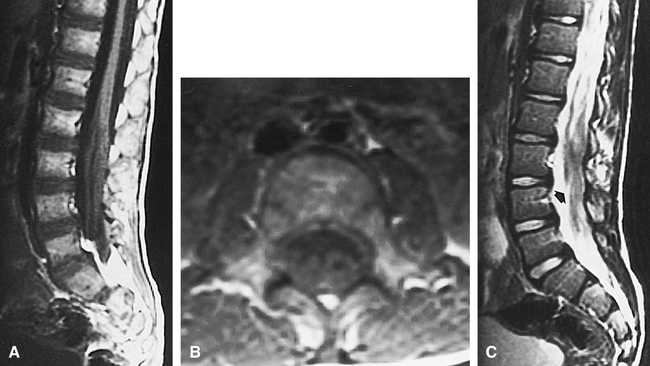
Síndrome de Guillain–Barré (SGB) é uma fraqueza muscular de aparecimento súbito causada pelo ataque do sistema imunitário ao sistema nervoso periférico. Os sintomas iniciais são geralmente dor ou alterações de sensibilidade e fraqueza muscular com início nos pés e nas mãos. Esta fraqueza muitas vezes espalha-se para os braços e parte superior do corpo, envolvendo ambos os lados. Os sintomas desenvolvem-se ao longo de um intervalo de algumas horas a algumas semanas. Durante a fase aguda, a doença pode colocar a vida em risco, dado que 15% das pessoas apresentam fraqueza nos músculos respiratórios e necessitam de ventilação mecânica. Algumas são afetadas por alterações funcionais no sistema nervoso autónomo, o que pode provocar anormalidades graves no ritmo cardíaco e na pressão arterial.
Introdução
O que você precisa saber de cara
Doença rara que causa neuropatia periférica progressiva, com fraqueza muscular, perda de sensibilidade e deformidades nos pés e mãos. Caracteriza-se por velocidade de condução nervosa reduzida e pode apresentar cifoescoliose e pé cavo.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 23 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 35 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
4 genes identificados com associação a esta condição. Padrão de herança: Autosomal dominant, Autosomal recessive, Not applicable.
Seems to be involved in pore-forming activity and may contribute to the unspecific permeability of the peroxisomal membrane
Peroxisome membrane
Scaffolding protein that functions as part of a dystroglycan complex in Schwann cells, and as part of EZR and AHNAK-containing complexes in eye lens fiber cells. Required for the maintenance of the peripheral myelin sheath that is essential for normal transmission of nerve impulses and normal perception of sensory stimuli. Required for normal transport of MBP mRNA from the perinuclear to the paranodal regions. Required for normal remyelination after nerve injury. Required for normal elongation o
Cell membraneNucleusCytoplasmCell junction
Dejerine-Sottas syndrome
A severe degenerating neuropathy of the demyelinating Charcot-Marie-Tooth disease category, with onset by age 2 years. Characterized by motor and sensory neuropathy with very slow nerve conduction velocities, increased cerebrospinal fluid protein concentrations, hypertrophic nerve changes, delayed age of walking as well as areflexia. There are both autosomal dominant and autosomal recessive forms of Dejerine-Sottas syndrome.
Is an adhesion molecule necessary for normal myelination in the peripheral nervous system. It mediates adhesion between adjacent myelin wraps and ultimately drives myelin compaction
Cell membraneMyelin membrane
Charcot-Marie-Tooth disease, demyelinating, type 1B
A dominant demyelinating form of Charcot-Marie-Tooth disease, a disorder of the peripheral nervous system, characterized by progressive weakness and atrophy, initially of the peroneal muscles and later of the distal muscles of the arms. Charcot-Marie-Tooth disease is classified in two main groups on the basis of electrophysiologic properties and histopathology: primary peripheral demyelinating neuropathies (designated CMT1 when they are dominantly inherited) and primary peripheral axonal neuropathies (CMT2). Demyelinating neuropathies are characterized by severely reduced nerve conduction velocities (less than 38 m/sec), segmental demyelination and remyelination with onion bulb formations on nerve biopsy, slowly progressive distal muscle atrophy and weakness, absent deep tendon reflexes, and hollow feet.
Sequence-specific DNA-binding transcription factor (PubMed:17717711). Plays a role in hindbrain segmentation by regulating the expression of a subset of homeobox containing genes and in Schwann cell myelination by regulating the expression of genes involved in the formation and maintenance of myelin (By similarity). Binds to two EGR2-consensus sites EGR2A (5'-CTGTAGGAG-3') and EGR2B (5'-ATGTAGGTG-3') in the HOXB3 enhancer and promotes HOXB3 transcriptional activation (By similarity). Binds to sp
Nucleus
Neuropathy, congenital hypomyelinating, 1, autosomal recessive
A severe degenerating neuropathy that results from a congenital impairment in myelin formation. It is clinically characterized by early onset of hypotonia, areflexia, distal muscle weakness, and very slow nerve conduction velocities (as low as 3m/s). Some patients manifest nearly complete absence of spontaneous limb movements, respiratory distress at birth, and complete absence of myelin shown by electron microscopy of peripheral nerves.
Variantes genéticas (ClinVar)
649 variantes patogênicas registradas no ClinVar.
Classificação de variantes (ClinVar)
Distribuição de 17 variantes classificadas pelo ClinVar.
Vias biológicas (Reactome)
6 vias biológicas associadas aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Síndrome de Dejerine-Sottas
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
Hereditary Polyneuropathies in the Era of Precision Medicine: Genetic Complexity and Emerging Strategies.
Hereditary polyneuropathies represent a genetically and clinically heterogeneous group of disorders affecting the peripheral nervous system, characterized by progressive motor, sensory, and autonomic impairment. Advances in molecular genetics have identified key causative genes, including PMP22, MPZ, MFN2, TTR, EGR2, and CX32 (GJB1), which are implicated in Charcot-Marie-Tooth disease, Dejerine-Sottas syndrome, and related neuropathies. These conditions display substantial allelic and locus heterogeneity. Pathogenetically, mechanisms involve impaired myelin maintenance, disrupted axonal transport, mitochondrial dysfunction, and aberrant Schwann cell biology. Despite these insights, therapeutic options remain limited, and there is a pressing need to translate genetic findings into effective interventions. This review aims to provide a comprehensive synthesis of current knowledge compiling all known mutations resulting in hereditary polyneuropathies. In addition, it underscores the molecular pathomechanisms of hereditary polyneuropathies and evaluates emerging therapeutic strategies, including adeno-associated virus mediated RNA interference, CRISPR-based gene editing, antisense oligonucleotide therapy, and small-molecule modulators of axonal degeneration. Furthermore, the integration of precision diagnostics, such as next-generation sequencing and functional genomic approaches, is discussed in the context of personalized disease management. Collectively, this review underscores the need for patient-centered approaches in advancing care for individuals with hereditary polyneuropathies.
PMP22-Related Neuropathies: A Systematic Review.
Background. PMP22-related neuropathies comprise a spectrum of predominantly demyelinating disorders, most commonly Charcot-Marie-Tooth type 1A (CMT1A; 17p12 duplication) and hereditary neuropathy with liability to pressure palsies (HNPP; 17p12 deletion), with rarer phenotypes due to PMP22 sequence variants (CMT1E, Dejerine-Sottas syndrome [DSS]). Methods. We conducted a PRISMA-compliant systematic review (PROSPERO ID: 1139921) of PubMed and Scopus (January 2015-August 2025). Eligible studies reported genetically confirmed PMP22-related neuropathies with clinical and/or neurophysiological data. Owing to heterogeneous reporting, we synthesized pooled counts and proportions without meta-analysis, explicitly tracking missing denominators. Results. One hundred twenty-seven studies (n = 4493 patients) were included. Sex was available for 995 patients (males 53.8% [535/995]; females 46.2% [460/995]); mean age at onset was 23.7 years in males and 16.4 years in females. Phenotypic classification was reported for 4431/4493 (75.4% CMT1A, 20.9% HNPP, 2.6% CMT1E, 1.2% DSS). Across phenotypes, weakness/foot drop was the leading presenting symptom when considering only cohorts that explicitly reported it (e.g., 65.3% in CMT1A; 76.0% in HNPP); sensory complaints (numbness, paresthesia/dysesthesia) were variably documented. Neurophysiology consistently showed demyelinating patterns, with median and ulnar nerves most frequently abnormal among assessed nerves; in HNPP, deep peroneal and sural involvement were also common in evaluated subsets. Comorbidities clustered by phenotype: orthopedic/neuromuscular features (pes cavus/hammer toes, scoliosis/kyphosis, tremor) in CMT1A and DSS; broader metabolic/autoimmune and neurodevelopmental associations in HNPP; and higher syndromic/ocular/hearing involvement in CMT1E. Genetically, 75.6% (3241/4291) had 17p12 duplication, 19.6% (835/4291) 17p12 deletion, and 4.8% (215/4291) PMP22 sequence variants with marked allelic heterogeneity. Among 2571 cases with available methods, MLPA was most used (41.9%), followed by NGS (20.4%) and Sanger sequencing (17.8%). Main limitations include heterogeneous and incomplete reporting across studies (especially symptoms and nerve-specific data) and the absence of a formal risk-of-bias appraisal, which preclude meta-analysis and may skew phenotype proportions toward more frequently reported entities (e.g., CMT1A). Conclusions. Recent literature confirms that PMP22 copy-number variants account for the vast majority of cases, while sequence-level variants underpin a minority with distinct phenotypes (notably CMT1E/DSS). Routine MLPA, complemented by targeted/NGS, optimizes diagnostic yield. Standardized reporting of nerve-conduction parameters and symptom denominators is urgently needed to enable robust cross-study comparisons in both pediatric and adult populations.
The cytoplasmic tail of myelin protein zero induces morphological changes in lipid membranes.
The major myelin protein expressed by the peripheral nervous system Schwann cells is protein zero (P0), which represents 50% of the total protein content in myelin. This 30-kDa integral membrane protein consists of an immunoglobulin (Ig)-like domain, a transmembrane helix, and a 69-residue C-terminal cytoplasmic tail (P0ct). The basic residues in P0ct contribute to the tight packing of myelin lipid bilayers, and alterations in the tail affect how P0 functions as an adhesion molecule necessary for the stability of compact myelin. Several neurodegenerative neuropathies are related to P0, including the more common Charcot-Marie-Tooth disease (CMT) and Dejerine-Sottas syndrome (DSS) as well as rare cases of motor and sensory polyneuropathy. We found that high P0ct concentrations affected the membrane properties of bicelles and induced a lamellar-to-inverted hexagonal phase transition, which caused bicelles to fuse into long, protein-containing filament-like structures. These structures likely reflect the formation of semicrystalline lipid domains with potential relevance for myelination. Not only is P0ct important for stacking lipid membranes, but time-lapse fluorescence microscopy also shows that it might affect membrane properties during myelination. We further describe recombinant production and low-resolution structural characterization of full-length human P0. Our findings shed light on P0ct effects on membrane properties, and with the successful purification of full-length P0, we have new tools to study the role of P0 in myelin formation and maintenance in vitro.
Genotype-phenotype characteristics and baseline natural history of Chinese myelin protein zero gene related neuropathy patients.
The aim was to characterize the phenotypic and genotypic features of myelin protein zero (MPZ) related neuropathy and provide baseline data for longitudinal natural history studies or drug clinical trials. Clinical, neurophysiological and genetic data of 37 neuropathy patients with MPZ mutations were retrospectively collected. Nineteen different MPZ mutations in 23 unrelated neuropathy families were detected, and the frequency of MPZ mutations was 5.84% in total. Mutations c.103_104InsTGGTTTACACCG, c.513dupG, c.521_557del and c.696_699delCAGT had not been reported previously. Hot spot mutation p.Thr124Met was detected in four unrelated families, and seven patients carried de novo mutations. The onset age indicated a bimodal distribution: prominent clustering in the first and fourth decades. The infantile-onset group included 12 families, the childhood-onset group consisted of two families and the adult-onset group included nine families. The Charcot-Marie-Tooth Disease Neuropathy Score ranged from 3 to 25 with a mean value of 15.85 ± 5.88. Mutations that changed the cysteine residue (p.Arg98Cys, p.Cys127Trp, p.Ser140Cys and p.Cys127Arg) in the extracellular region were more likely to cause severe early-onset Charcot-Marie-Tooth disease type 1B (CMT1B) or Dejerine-Sottas syndrome. Nonsense-mediated mRNA decay mutations p.Asp35delInsVVYTD, p.Leu174Argfs*66 and p.Leu172Alafs*63 were related to severe infantile-onset CMT1B or Dejerine-Sottas syndrome; however, mutation p.Val232Valfs*19 was associated with a relatively milder childhood-onset CMT1 phenotype. Four novel MPZ mutations are reported that expand the genetic spectrum. De novo mutations accounted for 30.4% and were most related to a severe infantile-onset phenotype. Genetic and clinical data from this cohort will provide the baseline data necessary for clinical trials and natural history studies.
EGR2 gene-linked hereditary neuropathies present with a bimodal age distribution at symptoms onset.
Mutations in the Early-Growth Response 2 (EGR2) gene cause various hereditary neuropathies, including demyelinating Charcot-Marie-Tooth (CMT) disease type 1D (CMT1D), congenital hypomyelinating neuropathy type 1 (CHN1), Déjerine-Sottas syndrome (DSS), and axonal CMT (CMT2). In this study, we identified 14 patients with heterozygous EGR2 mutations diagnosed between 2000 and 2022. Mean age was 44 years (15-70), 10 patients were female (71%), and mean disease duration was 28 years (1-56). Disease onset was before age 15 years in nine cases (64%), after age 35 years in four cases (28%), and one patient aged 26 years was asymptomatic (7%). All symptomatic patients had pes cavus and distal lower limbs weakness (100%). Distal lower limbs sensory symptoms were observed in 86% of cases, hand atrophy in 71%, and scoliosis in 21%. Nerve conduction studies showed a predominantly demyelinating sensorimotor neuropathy in all cases (100%), and five patients needed walking assistance after a mean disease duration of 50 years (47-56) (36%). Three patients were misdiagnosed as inflammatory neuropathy and treated with immunosuppressive drugs for years before diagnosis was corrected. Two patients presented with an additional neurologic disorder, including Steinert's myotonic dystrophy and spinocerebellar ataxia (14%). Eight EGR2 gene mutations were found, including four previously undescribed. Our findings demonstrate EGR2 gene-related hereditary neuropathies are rare and slowly progressive demyelinating neuropathies with two major clinical presentations, including a childhood-onset variant and an adult-onset variant which may mimic inflammatory neuropathy. Our study also expands the genotypic spectrum of EGR2 gene mutations.
Publicações recentes
Hereditary Polyneuropathies in the Era of Precision Medicine: Genetic Complexity and Emerging Strategies.
PMP22-Related Neuropathies: A Systematic Review.
The cytoplasmic tail of myelin protein zero induces morphological changes in lipid membranes.
EGR2 gene-linked hereditary neuropathies present with a bimodal age distribution at symptoms onset.
A case report of two Moroccan patients with hereditary neurological disorders and molecular modeling study on the S72L de novo PMP22 variant.
📚 EuropePMC23 artigos no totalmostrando 21
Hereditary Polyneuropathies in the Era of Precision Medicine: Genetic Complexity and Emerging Strategies.
GenesPMP22-Related Neuropathies: A Systematic Review.
GenesThe cytoplasmic tail of myelin protein zero induces morphological changes in lipid membranes.
Biochimica et biophysica acta. BiomembranesEGR2 gene-linked hereditary neuropathies present with a bimodal age distribution at symptoms onset.
Journal of the peripheral nervous system : JPNSA case report of two Moroccan patients with hereditary neurological disorders and molecular modeling study on the S72L de novo PMP22 variant.
Revue neurologiqueGenotype-phenotype characteristics and baseline natural history of Chinese myelin protein zero gene related neuropathy patients.
European journal of neurologyExpanding the phenotypic spectrum of Dejerine-Sottas syndrome caused by the trembler mutation.
NeurogeneticsIon mobility-mass spectrometry reveals the role of peripheral myelin protein dimers in peripheral neuropathy.
Proceedings of the National Academy of Sciences of the United States of AmericaSubcellular diversion of cholesterol by gain- and loss-of-function mutations in PMP22.
GliaA Case of Severe Early-Onset Neuropathy Caused by a Compound Heterozygous Deletion of the PMP22 Gene: Clinical and Neurographic Aspects.
Neuropediatrics[A genotyping study of 13 cases of early-onset Charcot-Marie-Tooth disease].
Zhongguo dang dai er ke za zhi = Chinese journal of contemporary pediatricsNeuropathy-related mutations alter the membrane binding properties of the human myelin protein P0 cytoplasmic tail.
PloS oneJules Sottas (1866-1945) forgotten despite the eponym: "Dejerine-Sottas syndrome".
Revue neurologiqueA novel family with axonal Charcot-Marie-Tooth disease caused by a mutation in the EGR2 gene.
Journal of the peripheral nervous system : JPNSJules Dejerine and the peripheral nervous system.
NeurologyA Novel Asp121Asn Mutation of Myelin Protein Zero Is Associated with Late-Onset Axonal Charcot-Marie-Tooth Disease, Hearing Loss and Pupil Abnormalities.
Frontiers in aging neuroscienceEGR2 mutation enhances phenotype spectrum of Dejerine-Sottas syndrome.
Journal of neurologyDéjerine-Sottas syndrome: Prenatal and postnatal postural and motor assessment.
Journal of obstetrics and gynaecology : the journal of the Institute of Obstetrics and GynaecologyProteolipid protein modulates preservation of peripheral axons and premature death when myelin protein zero is lacking.
GliaImpact of I30T and I30M substitution in MPZ gene associated with Dejerine-Sottas syndrome type B (DSSB): A molecular modeling and dynamics.
Journal of theoretical biologyThe use of whole-exome sequencing to disentangle complex phenotypes.
European journal of human genetics : EJHGAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Síndrome de Dejerine-Sottas.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Síndrome de Dejerine-Sottas
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Hereditary Polyneuropathies in the Era of Precision Medicine: Genetic Complexity and Emerging Strategies.
- PMP22-Related Neuropathies: A Systematic Review.
- The cytoplasmic tail of myelin protein zero induces morphological changes in lipid membranes.
- Genotype-phenotype characteristics and baseline natural history of Chinese myelin protein zero gene related neuropathy patients.
- EGR2 gene-linked hereditary neuropathies present with a bimodal age distribution at symptoms onset.
- A case report of two Moroccan patients with hereditary neurological disorders and molecular modeling study on the S72L de novo PMP22 variant.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:64748(Orphanet)
- OMIM OMIM:145900(OMIM)
- MONDO:0007790(MONDO)
- GARD:9204(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Q845618(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar