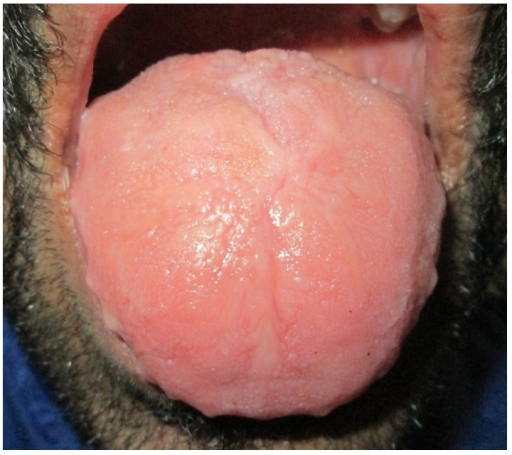
É quando a língua é maior que o normal. Isso pode ser de nascença, ou surgir por causa de um tumor, ou de um inchaço causado pelo bloqueio dos vasos que drenam a linfa. Também pode acontecer em conjunto com o hiperpituitarismo (quando uma glândula no cérebro produz hormônios em excesso) ou com a acromegalia (uma doença que causa o crescimento exagerado de algumas partes do corpo). Além disso, pode estar associada a problemas de mordida (maloclusão), devido à pressão da língua nos dentes.
Introdução
O que você precisa saber de cara
É quando a língua é maior que o normal. Isso pode ser de nascença, ou surgir por causa de um tumor, ou de um inchaço causado pelo bloqueio dos vasos que drenam a linfa. Também pode acontecer em conjunto com o hiperpituitarismo (quando uma glândula no cérebro produz hormônios em excesso) ou com a acromegalia (uma doença que causa o crescimento exagerado de algumas partes do corpo). Além disso, pode estar associada a problemas de mordida (maloclusão), devido à pressão da língua nos dentes.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 1 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 4 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Macroglossia
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
6 ensaios clínicos encontrados.
Publicações mais relevantes
Bilateral ovarian steroid cell tumor in a postmenopausal woman with progressive hyperandrogenism.
Severe hyperandrogenism with new-onset virilization in postmenopausal women is rare and often associated with androgen-secreting tumors. Nevertheless, a comprehensive differential diagnosis must be considered, including ovarian hyperthecosis and Cushing syndrome. We report a 71-year-old woman with progressive hirsutism over 1-2 years, presenting with severe hyperandrogenism and insulin resistance. Physical examination revealed moderate hirsutism with a score of 15 according to the modified Ferriman-Gallwey scale, androgenic alopecia, dental diastema, macroglossia, and acanthosis. Hormonal analysis demonstrated elevated free testosterone levels on two separate occasions: 8.1 ng/mL (SI: 28 nmol/L) and 6.7 ng/mL (SI: 23.2 nmol/L) (reference range 0.12-0.35 ng/mL [SI 0.42-1.22 nmol/L]); with all other androgenic parameters within the normal range. Imaging studies, including abdominal computed tomography (CT) and transvaginal ultrasound, showed normal adrenal glands and adnexa. Based on clinical suspicion, the patient underwent bilateral adnexectomy. Histopathology confirmed a bilateral ovarian steroid cell tumor, not otherwise specified. Postoperatively, serum testosterone normalized (0.16 ng/mL [SI: 0.55 nmol/L]) within one month with progressive improvement in hirsutism.
[Guidelines for the diagnosis and treatment of obstructive sleep apnea in adults (2025)].
Obstructive sleep apnea (OSA) is a highly prevalent sleep-related breathing disorder with a considerable healthcare burden. Previously, the 2011 guideline for adult obstructive sleep apnea was largely formulated on the basis of expert opinion and consensus, which played an important role in guiding clinical practice. With the growing body of evidence from high-quality clinical studies, however, guideline development models that rely primarily on expert consensus are no longer adequate to support contemporary clinical decision-making. To further standardize the screening, diagnosis, treatment, and long-term management of OSA in adults, the Sleep Disordered Breathing Assembly of the Chinese Thoracic Society has developed evidence-based clinical practice guidelines. The recommendations were formulated according to the best currently available evidence, following the Appraisal of Guidelines for Research and Evaluation Ⅱ (AGREE Ⅱ) framework and the Reporting Items for Practice Guidelines in Healthcare (RIGHT) statement. Based on an extensive preliminary investigation, the guideline addresses 18 key clinical questions and provides detailed, evidence-based recommendations, aiming to support clinical decision-making and to promote standardized diagnosis, treatment, and management of adults with OSA in China.The clinical questions and recommendations are listed below.Question 1: Which populations should be screened for OSA?Recommendation 1: Routine screening for OSA is not recommended in the general population without high-risk features (1, A). Screening is recommended for individuals at high risk for OSA who exhibit typical symptoms or physical signs, or who have relevant comorbidities. Screening is also recommended for perioperative patients (e.g., candidates for bariatric surgery or other high-risk procedures) (1, A). Screening may be considered for high-risk individuals without typical symptoms (2, B). Screening is also recommended for individuals whose OSA may increase the risk of driving or occupational accidents (1, A).High-risk populations for OSA include: (1) Individuals with typical OSA symptoms, such as habitual snoring, excessive daytime sleepiness, witnessed apneas, nocturnal gasping or choking, morning headaches, morning dry mouth, non-restorative sleep, nocturia, impaired attention, memory decline, and reduced sexual function; (2) Individuals with typical physical signs of OSA, including obesity, increased neck circumference, retrognathia or micrognathia, macroglossia, enlarged uvula and soft palate, and tonsillar hypertrophy; (3) Individuals with OSA-related complications or comorbidities, such as obesity, hypertension, type 2 diabetes mellitus, cardiovascular disease, metabolic syndrome, hypothyroidism, polycystic ovary syndrome, acromegaly, neuromuscular diseases, depression, and anxiety; (4) Specific populations, including middle-aged and older men, pregnant women, and postmenopausal women; (5) Individuals with a family history of OSA, particularly those with first-degree relatives affected by OSA (1, A).Question 2: What is the role of questionnaires, craniofacial assessment, and other predictive tools in screening and evaluating individuals at high risk for OSA?Recommendation 2: The STOP-Bang questionnaire is recommended for OSA screening (1, A). The Berlin questionnaire and STOP questionnaire may also be considered (1, B). The Epworth Sleepiness Scale (ESS) is recommended to assess daytime sleepiness severity but should not be used to diagnose OSA (1, A). Subjective questionnaires alone, without objective sleep monitoring, are not recommended for OSA diagnosis (1, A).A structured physical examination of the upper airway and craniofacial features is recommended, including the modified Mallampati score and Friedman tongue position classification. Further evaluation (e.g., cephalometric radiography, CT or MRI of the upper airway) may be performed when indicated (1, A).Clinically validated consumer-grade sleep monitors and wearable AI devices may be considered to assist self-screening in high-risk individuals and encourage timely medical consultation. However, these are non-medical screening tools and should not replace medical-grade sleep monitoring for diagnosis (1, A).Question 3: How should polysomnography (PSG) and home sleep apnea testing (HSAT) be used in the diagnosis of OSA in adults?Recommendation 3: PSG is the gold standard for diagnosing OSA in adults (1, A). It is recommended as the first choice for complex cases (especially those with comorbid sleep disorders) and individuals in high-risk occupations (1, A). PSG is also preferred for precise assessment of treatment efficacy and follow-up (1, A).HSAT is recommended for diagnosing clinically suspected moderate-to-severe uncomplicated OSA, but should not be used to rule out OSA (1, A). It may also be used for hospitalized patients with limited mobility or critical illness requiring prompt intervention (1, A). HSAT can serve as an adjunct tool for treatment response assessment and follow-up (1, A). It is not recommended for general screening of asymptomatic individuals or for diagnosing mild OSA (1, A).Question 4: What are the diagnostic criteria and severity classification for OSA in adults?Recommendation 4: The ICSD-3-TR diagnostic criteria are recommended for diagnosing OSA in adults (1, A). In resource-limited primary care settings, simplified criteria incorporating history, physical examination, and pulse oximetry may be used (1, A).OSA severity should be classified primarily based on the apnea-hypopnea index (AHI), with nocturnal minimum pulse oxygen saturation as a supplementary measure of hypoxemia burden (1, A). Emerging indices such as HB and SBII may be considered when assessing cardiovascular and comorbidity risks (2, B).Question 5: How should OSA phenotypes and endotypes be assessed?Recommendation 5: There is no universally accepted phenotyping standard. In clinical practice, symptom-based categories are commonly used: excessive daytime sleepiness predominant, sleep disturbance/fragmentation predominant, and asymptomatic/minimally symptomatic phenotypes (1, B). Phenotype assessment should integrate demographics, symptoms, history, PSG data, and validated questionnaires (1, B).Endotyping may be considered using four physiological traits: critical closing pressure, arousal threshold, loop gain, and upper airway muscle responsiveness (1, B). Techniques such as CPAP pressure titration and esophageal pressure monitoring may be used to assess OSA endotypes (1, B). Alternatively, OSA endotypes may be estimated through advanced analysis of PSG signals (2, B).Individualized assessment of patients with OSA may also incorporate potentially treatable traits, including daytime functional impairment (e.g., excessive daytime sleepiness), co-existing sleep disorders (e.g., insomnia), specific high-risk factors (e.g., obesity), and underlying pathophysiological mechanisms, such as those described in the PALM framework (2, B).Question 6: Which health complications and safety risks should be prioritized in adults with OSA?Recommendation 6: Adults with OSA should be specifically monitored for cardiovascular disease, cerebrovascular disease, metabolic disorders, cognitive impairment, and traffic-or occupation-related safety risks (1, A). Evaluation for other potential risks, including malignancy, depression, chronic cough, asthma, and chronic obstructive pulmonary disease (COPD), is also recommended (1, B).Question 7: How should comprehensive management of adults with OSA be implemented?Recommendation 7: Comprehensive management of adult OSA should be multidisciplinary, individualized, and long-term, based on disease severity, etiology, lifestyle, and patient preferences (1, A).Lifestyle interventions are recommended for all patients, including dietary control, alcohol avoidance, smoking cessation, cautious use or avoidance of sedative-hypnotic agents and other medications that may induce or exacerbate OSA, sleep hygiene, and regular physical activity (1, A). Positional therapy is recommended for position-dependent OSA (1, A). Active weight management with a body mass index (BMI)-based stepwise strategy is recommended (1, A).Question 8: What are the indications for positive airway pressure (PAP) therapy in adults with OSA?Recommendation 8: PAP therapy is recommended as first-line treatment for adults with moderate-to-severe OSA (AHI≥15 events/h) (1, A). It may also be considered for patients with mild OSA who have cardiovascular or cerebrovascular disease, hypertension, diabetes, COPD, or prominent symptoms such as EDS, cognitive impairment, insomnia, or depression, as well as for perioperative patients (1, B).Question 9: How should PAP modalities be selected for adults with OSA?Recommendation 9: CPAP, APAP and BPAP are comparable in efficacy, safety, and adherence. CPAP is recommended as the default modality due to lower cost (1, A). APAP is recommended for patients intolerant to CPAP, or with positional, sleep-stage dependent, or alcohol-related OSA, or significant weight fluctuations (1, A). For asymptomatic patients, CPAP or APAP is recommended (1, A). BPAP is indicated if obstructive events persist at CPAP pressures≥15 cmH2O (1 cmH2O=0.098 kPa), for intolerance to high CPAP pressures, or for OSA with chronic hypoventilation disorders such as COPD, neuromuscular diseases, or obesity hypoventilation syndrome (1, A).Question 10: What are the principles and procedures for PAP titration?Recommendation 10: PAP pressure titration is recommended before initiating therapy (1, A). In-laboratory, full-night manual titration during PSG is the gold standard (1, A). For moderate-to-severe OSA, split-night in-laboratory titration or home auto-titration are acceptable alternatives (1, A). Manual titration is preferred over auto-titration in patients with congestive heart failure, severe pulmonary disease, neuromuscular disease, prior uvulopalatopharyngoplasty, need for nocturnal oxygen, or expected desaturation from non-OSA causes (e.g., hypoventilation or central sleep apnea syndromes) (1, A).Question 11: How can adherence to PAP therapy be improved?Recommendation 11: A structured, regular follow-up system is recommended, including telemedicine (remote monitoring, phone/video consultations, AI/smartphone apps) and behavioral or psychosocial interventions (e.g., motivational enhancement therapy, motivational interviewing) (1, A).Question 12: What are the indications for oral appliance therapy?Recommendation 12: Oral appliance therapy is recommended for primary snoring and mild-to-moderate OSA (1, A). It is also recommended as an alternative or adjunct for patients with poor PAP tolerance or adherence (1, A). Custom-made oral appliances are preferred over non-custom devices to improve adherence and effectiveness (1, A).Question 13: What are the indications for oropharyngeal myofunctional therapy?Recommendation 13: Oropharyngeal myofunctional therapy is recommended as an adjunct or combined therapy in patients with OSA (1, A).Question 14: What are the indications for upper airway surgery?Recommendation 14: Upper airway surgery may be considered for adults with significant anatomical abnormalities who are intolerant or nonadherent to PAP therapy, after a careful evaluation of the potential benefits and risks (1, A).Question 15: What are the indications for pharmacological therapy?Recommendation 15: Pharmacological therapy is not recommended as routine treatment for all adults with OSA (1, A). It may be considered as adjunctive treatment for specific phenotypes or treatable traits such as EDS, insomnia, or obesity, with appropriate patient selection (1, B).For OSA-related EDS: After careful clinical evaluation, wake-promoting agents may be considered for patients with OSA-related EDS who meet one or more of the following criteria: 1. Residual EDS despite adequate and adherent standard OSA therapy (including CPAP, oral appliance therapy, or surgery), with other causes of EDS excluded; 2. Presence of EDS in patients who refuse, are intolerant of, or are nonadherent to standard OSA therapy; 3. EDS that substantially impairs quality of life, interferes with work or study, or significantly increases the risk of traffic or occupational accidents (e.g., documented accidents or near-miss events)(Expert consensus; no grading). For patients with residual EDS despite adequate and adherent OSA therapy, treatment with solriamfetol or modafinil is recommended to improve daytime sleepiness (1, A). For patients with EDS who refuse or cannot tolerate standard OSA therapy, individualized treatment with solriamfetol is recommended (1, A), while modafinil may be considered (2, B). During pharmacologic treatment, continued counseling and encouragement to initiate or resume standard OSA therapy are recommended.For COMISA: With attention to interindividual variability in treatment response, short-term use of non-benzodiazepine hypnotic agents may be considered to improve insomnia symptoms (1, B). When non-benzodiazepine hypnotics are deemed necessary, they should be used under close monitoring or in combination with CPAP therapy (1, B). Benzodiazepines are not recommended for the treatment of COMISA (1, A).For OSA with obesity: For patients with moderate-to-severe OSA complicated by obesity, who have not achieved adequate control despite structured weight-management interventions (including dietary modifications and exercise), treatment with dual GIP/GLP-1 receptor agonists (e.g., tirzepatide) may be considered as an adjunctive therapy (1, A).Question 16: How can phenotype-and endotype-based evaluation guide individualized treatment?Recommendation 16: An individualized treatment strategy based on OSA phenotypes and endotypes may be considered in adults with OSA (1, B).Question 17: How should long-term follow-up of adults with OSA be planned?Recommendation 17: Follow-up should assess symptoms, sleep-related quality of life, patient-reported sleep quality, treatment adherence, adverse events, and patient/family satisfaction (1, A). Tools may include questionnaires (ESS, PSQI, SF) and objective tests (PSG, HSAT, pulse oximetry, MSLT, MWT) (1, A). Follow-up intervals should be tailored to the treatment; for PAP therapy, visits at 1 week, 1 month, and 3 months are recommended, and then every 6-12 months if stable (1, A).Question 18: What are the major applications of telemedicine in comprehensive OSA management?Recommendation 18: Telemedicine is valuable for remote diagnosis, treatment, and follow-up. It is recommended to improve PAP adherence (1, A). Remote diagnostic pathways combining HSAT with electronic questionnaires may be considered (2, B). Quality control measures should be implemented to ensure safety and effectiveness (1, A). 阻塞性睡眠呼吸暂停(OSA)是一种常见的睡眠呼吸疾病,其患病率高,社会医疗负担重。此前,2011年版我国成人OSA相关指南主要基于专家经验和共识形成,为临床实践提供了重要参考,但随着循证医学研究的不断积累,既往以专家共识为主的指南模式已难以充分满足当前临床决策需求。为进一步规范我国成人OSA患者的筛查、诊断、治疗及疾病管理,中华医学会呼吸病学分会睡眠呼吸障碍学组基于当前可获得的最佳证据,参考指南研究与评价方法(AGREE Ⅱ)并按照卫生保健实践指南的报告条目(RIGHT)就前期调研形成的18个临床问题进行充分的讨论并给出了详细的推荐意见和相关证据,旨在为成人OSA的规范诊治提供临床决策支持。.
Patient-Reported Speech Outcomes in Patients with Beckwith-Wiedemann Syndrome.
Macroglossia is a hallmark feature of Beckwith-Wiedemann Syndrome (BWS) and may affect a child's appearance, speech, and feeding. Tongue reduction surgery (TRS) is often recommended to address functional concerns, but its effects on patient-reported speech outcomes remain unclear. This study evaluates self-reported speech outcomes in individuals with BWS. Patients with BWS (aged 4-18 years) were prospectively administered the FACE-Q Craniofacial measures (speech distress, breathing, eating and drinking, facial function, speech function). Surveys were Rasch transformed score (0-100, 100=best outcome). Clinical characteristics, BWS Index of Macroglossia (BIG), and Intelligibility in Context Scale (ICS) scores were reviewed. Thirty-six patients (50% male; mean age 8.6±3.8 years at survey) were included. Most patients had an IC2-LOM genetic diagnosis (n=24, 66.6%). Average BIG score was 1.3±1.1 (range 0-3). Speech therapy was received by 28 patients (77.8%) and 16 (44.4%) underwent TRS at mean age 2.3±2.0 years. FACE-Q scores averaged 84.7±15.0 for speech distress, 84.9±15.0 for breathing, 80.9±15.9 for eating and drinking, 92.0±12.1 for facial function, and 75.8±19.5 for speech function. There was moderate correlation between ICS score and speech function (r=0.697, p=0.001). Patients who received speech therapy at school and clinically had lower speech function (p=0.014). No significant differences were found between surgical and non-surgical patients or by BIG scores (p>0.1). While overall reported outcomes were favorable, speech function scores were lower, suggesting persistent speech challenges in this population. These findings underscore the multifactorial nature of speech development in BWS and the importance of individualized, longitudinal management to optimize outcomes.
Tongue Reduction for Pediatric Obstructive Sleep Apnea: A Systematic Review.
Obstructive sleep apnea (OSA) is a prevalent pediatric disorder that, if untreated, can result in substantial developmental and health consequences. Tongue reduction procedures, such as midline posterior glossectomy (MPG), are increasingly used to address tongue base obstruction. This systematic review evaluates the effectiveness and safety of tongue reduction procedures for pediatric OSA. Embase, PubMed, and Web of Science databases were queried for studies from inception to September 20, 2023. Studies reporting on outcomes of pediatric patients (≤21 years) undergoing tongue reduction surgery for OSA were included. From 477 abstracts, 9 studies met the inclusion criteria, representing 146 pediatric patients. Surgical techniques included MPG, transoral robotic-assisted tongue base resection, and keyhole partial glossectomy. Primary outcomes assessed were apnea-hypopnea index (AHI), minimum oxygen saturation, and adverse events. All studies reported a reduction in AHI and increased minimum oxygen saturation following tongue reduction despite the method. Adverse events appear to be rare but included postoperative bleeding, need for reintubation, and wound dehiscence. Tongue reduction procedures appear to be safe and effective for managing pediatric OSA, improving key clinical outcomes. However, long-term results, comparative studies of surgical techniques, and refined patient selection criteria are needed. Future research should also identify risk factors for persistent OSA following tongue base reduction. These findings suggest that tongue reduction is a valuable addition to the treatment arsenal for pediatric OSA.
Obstructive Sleep Apnea-Hypopnea Syndrome in Children With Down Syndrome Treated at a Tertiary Care Hospital in Northeastern Colombia.
Obstructive sleep apnea-hypopnea syndrome (OSAHS) is frequent in children with Down Syndrome (DS), associated with anatomical characteristics such as midfacial hypoplasia, macroglossia, and hypotonia. It represents a frequent cause of morbidity and mortality among children with DS. Early identification of OSAHS in the DS population is essential, as untreated sleep breathing disorders are linked to severe complications, including pulmonary hypertension. Consequently, guidelines, such as the Health Supervision for Children with Down Syndrome from the American Academy of Pediatrics, recommend polysomnography (PSG) for all children with DS before age 4. This case-control study examined the profile of OSAHS in 124 patients with DS under 13 years of age who were treated at a tertiary care institution in northeastern Colombia from 2012 to 2023. Of the 124 patients, 19 (15.3%) were diagnosed with OSAHS. The only significant association identified was with place of residence, related to the fact that individuals (not patients) living in the city or its metropolitan area have greater access to PSG. Our observed frequency is lower than previously reported in the literature, indicating possible systematic underdiagnosis. Socioeconomic status and access to diagnostic evaluation, rather than clinical characteristics, appear to be the primary determinants for receiving a diagnosis. Expanding access to PSG, particularly in rural and low-income regions, and prioritizing universal screening in clinical protocols over symptom-based referral are essential steps.
Publicações recentes
Fissured Tongue associated with Hypothyroidism in a Young Patient.
🥇 DiretrizTongue swelling following cleft palate repair: report of a rare case.
The Natural Evolution of Macroglossia Among Beckwith-Wiedemann Patients: A 30-Year Institutional Review.
📖 RevisãoPRS Journal Club: Cleft Palate Technique Outcomes, Primary Cleft Rhinoplasty Grafts, and Macroglossia Reduction.
Discussion: A Comparison of Surgical Techniques for Macroglossia in Beckwith-Wiedemann Syndrome.
📚 EuropePMC498 artigos no totalmostrando 200
Bilateral ovarian steroid cell tumor in a postmenopausal woman with progressive hyperandrogenism.
JCEM case reports[Guidelines for the diagnosis and treatment of obstructive sleep apnea in adults (2025)].
Zhonghua jie he he hu xi za zhi = Zhonghua jiehe he huxi zazhi = Chinese journal of tuberculosis and respiratory diseasesPatient-Reported Speech Outcomes in Patients with Beckwith-Wiedemann Syndrome.
Plastic and reconstructive surgeryTongue Reduction for Pediatric Obstructive Sleep Apnea: A Systematic Review.
OTO openObstructive Sleep Apnea-Hypopnea Syndrome in Children With Down Syndrome Treated at a Tertiary Care Hospital in Northeastern Colombia.
CureusMacroglossia Due to Symmetrical Lipomatosis of the Tongue: A Rare Presentation of Madelung's Disease-Case Report.
Clinical case reportsSuccessful Medical Management of Severe Macroglossia Associated With Lingual Abscess in a Dog.
Journal of the American Animal Hospital AssociationCombination Lingual Compression and Maxillomandibular Fixation for Persistent Acquired Macroglossia: A Case Report.
OTO openCardiofaciocutaneous Syndrome Type 4 due to a MAP2K2 Variant: Expanding the Phenotypic Spectrum With Feeding Dysfunction and Neurodevelopmental Involvement.
Clinical case reportsMethylation profile characteristics in the H19/IGF2:IG-DMR revealed by long-read sequencing analysis in patients with Beckwith-Wiedemann syndrome having defects in the OCT4/SOX2 binding site.
Clinical epigeneticsBridging Diagnostic Gaps in AL Cardiac Amyloidosis: The Emerging Role of 68Ga-FAPI PET/CT.
Clinical nuclear medicineRaccoon eyes and macroglossia in AL amyloidosis.
QJM : monthly journal of the Association of PhysiciansCraniofacial and Radiological Features as Diagnostic Clues to Unmask Acromegaly: A Case Report.
CureusDermatological Manifestations of Amyloid Light-Chain (AL) Amyloidosis: A Case Report Highlighting Early Diagnosis and Treatment.
CureusAcromegaly in an elderly male with hepatic malignancy: a case report of a diagnostic dilemma.
Annals of medicine and surgery (2012)Development and Preliminary Application of a Beak Development Index in Pathogenicity Studies of Novel Goose Parvovirus.
Veterinary sciencesOrofacial manifestations in mucopolysaccharidoses: a comprehensive clinical and radiographic evaluation of 35 pediatric cases.
Head & face medicinePatient-Reported Psychosocial Outcomes in Patients with Beckwith-Wiedemann Syndrome.
Plastic and reconstructive surgery[Pediatric pneumological aspects in the care of children with Down Syndrome].
Klinische PadiatrieAnesthetic Management of a Patient With Myhre Syndrome.
Anesthesia progressScalloped Tongue as a Manifestation of Light Chain Amyloidosis in Multiple Myeloma.
Acta medica portuguesaOral mucosal health in acromegaly: clinical insights and metabolic associations.
BMC oral healthA Triad of Telltale Clues: Macroglossia Raccoon Eye and Nerve Compression Unveil Amyloid Light Chain Amyloidosis.
The Journal of the Association of Physicians of IndiaDental Implantology in Acromegaly: Pathophysiological Challenges, Biomaterial Interactions, and Future Directions-A Narrative Review.
Journal of functional biomaterialsCase Report: Beckwith-Wiedemann syndrome with reduced H19 expression.
Frontiers in pediatricsThe herculean illusion: congenital hypothyroidism masquerading as muscular dystrophy.
Acta neurologica BelgicaClinical and Molecular Evaluation of Beckwith-Wiedemann Syndrome with the BWSICS Score.
Molecular syndromologyExploring the boundaries of Niemann-Pick disease type A/B: a report of a case and review of literature.
Molecular and cellular pediatricsBeckwith-Wiedemann spectrum (BWSp): an update on diagnosis, management, and follow-up from the scientific committee of the Italian BWSp association.
Italian journal of pediatricsThe Successful Anesthetic Management of an Adult With Cri-du-Chat Syndrome by Using Personalized Behavioral Strategies: A Case Report.
CureusMacroglossia Caused by Venous Congestion in a Patient With Amyotrophic Lateral Sclerosis.
Clinical case reports(Epi)genotype-phenotype correlations of Beckwith-Wiedemann syndrome in China.
Italian journal of pediatricsDifficult airway and anesthesia management in a patient with sturge-weber syndrome related to excessive lip swollen and giant facial hemangioma: A case report.
Saudi journal of anaesthesiaMacroglossia and the Current Evidence of Surgical and Clinical Management.
The Journal of craniofacial surgeryClinical phenotype and molecular genetic analysis of 24 cases of Beckwith-Wiedemann syndrome.
Translational pediatricsAnalysis on the plane and mechanism of tongue-originated obstruction in Obstructive Sleep Apnea Syndrome (OSAS) patients with macroglossia.
Brazilian journal of otorhinolaryngologyA Comparison of Surgical Techniques for Macroglossia in Beckwith-Wiedemann Syndrome.
Plastic and reconstructive surgeryEvaluation of a caudal midline glossectomy on tongue volume and upper airway cross-sectional areas in brachycephalic dogs: a cadaveric study.
Frontiers in veterinary scienceCollaboration Between Endocrinologists and Dentists in the Care of Patients with Acromegaly-A Narrative Review.
Journal of clinical medicineUltrasonographic Features of Amyloid Arthropathy in Light Chain Amyloidosis: A Case Report.
Current rheumatology reviewsPartial Glossectomy in a 2-month-old Infant with Beckwith-Wiedemann Syndrome - A Case Report.
Annals of maxillofacial surgeryDiffuse Tongue Enlargement Related to Amyloidosis: A Case Report.
Journal of pharmacy & bioallied sciencesImportance of a Healthy Tongue: Could It Be a Reflection of Overall Health in Children?
CureusSupraglottic airway devices in neuroanesthesia practice: A narrative review.
Journal of anaesthesiology, clinical pharmacologyComparison of Minimally Invasive Surfactant Therapy and Intubation-surfactant Administration-extubation in Premature Neonates with Respiratory Distress Syndrome.
Oman medical journalCytological Diagnosis of Amyloidosis From Orbital Papules.
Cytopathology : official journal of the British Society for Clinical CytologyHyperbaric oxygen therapy for ballistic injuryinduced traumatic macroglossia.
BMJ case reportsOral Health and Quality of Life in Acromegaly: A Questionnaire-Based Study.
Dentistry journalLight Chain (AL) Amyloidosis Masquerading as Scleroderma: A Diagnostic Challenge.
Journal of hematologyMulti-locus methylation analyses reveal GNAS methylation defects in three patients with the Beckwith-Wiedemann syndrome phenotype and no molecular defects in the 11p15.5 imprinted region.
Clinical epigeneticsManagement of Congenital Macroglossia Due to Lymphatic Malformation in a Child with Review of Literature.
Journal of Indian Association of Pediatric SurgeonsMultidiscipline Therapy: Cervicofacial Vascular Anomaly With Macroglossia, Maxillofacial Deformity.
The LaryngoscopeMaternal Cell-Free DNA Analysis in a Fetus Affected by Beckwith-Wiedemann Syndrome: Potential for Prenatal Diagnosis.
CureusThe Obstructive Sleep Apnea Physical Exam: A Systematic Review and Meta-Analysis.
Laryngoscope investigative otolaryngologyNovel WAC gene variant identified in the first documented case of DeSanto-Shinawi Syndrome in India.
Molecular and cellular pediatricsTreatment Experience With Midfacial Distraction Osteogenesis for Down Syndrome.
The Journal of craniofacial surgeryClinical Characteristics and Remission Monitoring of 6q24-Related Transient Neonatal Diabetes.
Pediatric diabetesThe Effect of Tongue Volume and Adipose Content on Obstructive Sleep Apnea: Meta-analysis & Systematic Review.
OTO openDiagnosis and Management of Natal Tooth Secondary to Beckwith-Wiedemann Syndrome in a 25-day-old Infant: A Rare Case Report.
Contemporary clinical dentistryCantú Syndrome With Acromegaloid Features, Multiple Endocrinopathies, and Infection Susceptibility.
JCEM case reportsA scientometric study on research characteristics and trends of amyloidosis involving the oral cavity.
Journal of dental sciencesRespiratory and airway disorders in children with Down Syndrome: a review of the clinical challenges and management.
Frontiers in pediatricsImmediate Autologous Breast Reconstruction in a Patient With Achondroplasia.
Annals of plastic surgeryConservative Management of Macroglossia in Beckwith-Wiedemann Syndrome.
PediatricsAssociation between serum levels of inflammatory mediators and periodontitis severity in people with down syndrome.
CytokineOral manifestations of undiscovered systemic amyloidosis: a series of seven cases.
The Pan African medical journalPhenotypes of headache in patients with obstructive sleep apnea.
Scientific reportsSurgical management of the second cavernous lymphangioma in the tongue globally: A case report.
International journal of surgery case reportsPostprandial Hypoglycemia in a Patient With Clinical Beckwith-Wiedemann Syndrome.
JCEM case reportsPrenatal diagnosis of chromothripsis causing complex chromosomal rearrangement involving chromosomes 5, 7 and 11 leading to TWIST1 deletion and Saethre-Chotzen syndrome.
Taiwanese journal of obstetrics & gynecologyOutcomes of Tongue Reduction Surgery in Beckwith-Wiedemann Syndrome: A Systematic Review.
The Journal of craniofacial surgeryMultidisciplinary Treatment of A Class III Patient With Giant Open Bite Secondary to Macroglossia.
The Journal of craniofacial surgeryCase reports of oral appliance therapy on three young adults with Down syndrome and OSA.
Journal of prosthodontics : official journal of the American College of ProsthodontistsClinical Reasoning: A 65-Year-Old Woman With Isolated Macroglossia as the Initial Presentation of a Rare Disease.
NeurologyUnderstanding the clinical management of co-occurring sleep-related bruxism and obstructive sleep apnea in adults: A narrative and critical review.
Journal of prosthodontics : official journal of the American College of ProsthodontistsManagement for lymphatic malformations of head and neck.
Frontiers in neurologyMorphometric measurements of intraoral anatomy in children with Beckwith-Wiedemann syndrome: a novel approach.
Orphanet journal of rare diseasesA cross-sectional study of tongue disorders among dental outpatients.
Journal of stomatology, oral and maxillofacial surgeryBridging the Gaps: Multidisciplinary and Dental Strategies for Beckwith-Wiedemann Syndrome Management.
International journal of clinical pediatric dentistryPhenotypic Variability of LGMD 2C/R5 in a Genetically Homogenous Group of Bulgarian Muslim Roma.
GenesThe Peripheral Reduction With Keyhole Tongue Reduction Technique for Macroglossia in Beckwith-Wiedemann Syndrome.
The Journal of craniofacial surgeryAvalglucosidase alfa in infantile-onset Pompe disease: A snapshot of real-world experience in Italy.
Molecular genetics and metabolism reportsPhenotypic spectrum and tumor risk in Simpson-Golabi-Behmel syndrome: Case series and comprehensive literature review.
American journal of medical genetics. Part ABulbar muscle impairment in patients with late onset Pompe disease: Insight from the French Pompe registry.
European journal of neurologyConcurrent Papillary Craniopharyngioma and Growth Hormone-Secreting Pituitary Adenoma: A Rare and Aggressive Collision Tumor.
AACE clinical case reportsFeline dystrophin-deficient muscular dystrophy misdiagnosed as Toxoplasma myositis.
JFMS open reportsMacroglossia in endocrine and metabolic disorders: current evidence, perspectives and challenges.
Minerva endocrinologyEnzyme replacement therapy and immunotherapy lead to significant functional improvement in two children with Pompe disease: a case report.
Journal of medical case reportsA Case Report of a Filipino Boy with Childhood Cataract and Clinically Diagnosed Roberts Syndrome.
Acta medica PhilippinaThe Influence of the Tongue on the Development of Dental Malocclusion.
CureusUnusual Presentation of Beckwith-Wiedemann Syndrome in an Extremely Low Birth Weight Infant.
CureusCoexistence of variant-type transthyretin and immunoglobulin light-chain amyloidosis: a case report.
European heart journal. Case reportsPartial amputation due to tongue bite in death-associated with eclampsia.
Forensic science, medicine, and pathologyExpanded phenotype and cancer risk in patients with Beckwith-Wiedemann spectrum caused by CDKN1C variants.
American journal of medical genetics. Part ACASK pathogenic variant which expands the clinical spectrum for MICPCH syndrome in an adult patient.
American journal of medical genetics. Part ACerebrocostomandibular syndrome: a diagnostic challenge.
BMJ case reportsA rare case of extremely low birth weight infant with Beckwith-Wiedemann syndrome.
International journal of surgery case reportsAn idiopathic severe macroglossia in a young adult patient: a rare case.
Journal of surgical case reportsFailed Tracheal Extubation Due to Transient Isolated Macroglossia in a Child.
Annals of cardiac anaesthesiaBeckwith-Wiedemann Syndrome With Severe Relapsing Hypoglycemia After the Neonatal Period: A Case Report and a Literature Review.
CureusInterdisciplinary Treatment of Macroglossia Due to a Microcystic Lymphatic Malformation with Bleomycin Electrosclerotherapy Followed by Partial Resection.
Cardiovascular and interventional radiologyA Novel Macroglossia Severity Index for Beckwith-Wiedemann Syndrome.
Annals of surgeryRare but Real: Severe Unilateral Macroglossia and Submandibular Sialoadenitis After Skull Base Surgery.
CureusTrends in Blood Mosaicism and Clinical Phenotype Score in Patients with Beckwith-Wiedemann Syndrome Evaluated for Tongue Reduction Surgery.
Plastic and reconstructive surgeryOral Structural Dysphagia in Children.
Otolaryngologic clinics of North AmericaMultiple myeloma initially manifesting as a solitary deep ulcer on the tongue: a case study and literature review.
European journal of dermatology : EJDEffective Collaboration in the Surgical Management of Macroglossia in Beckwith-Wiedemann Syndrome.
Plastic and reconstructive surgery. Global openHypothyroidism presenting as a fissure tongue.
Clinical case reportsEvaluation of keyhole-pattern reduction glossoplasty for macroglossia in beckwith-wiedemann syndrome: A multidimensional analysis of postoperative course and outcomes.
Journal of cranio-maxillo-facial surgery : official publication of the European Association for Cranio-Maxillo-Facial SurgeryAssessment of Preoperative Predictors for Difficult Laryngeal Exposure in Endolaryngeal Surgery.
Indian journal of otolaryngology and head and neck surgery : official publication of the Association of Otolaryngologists of IndiaBeckwith-Wiedemann syndrome mimicking the classical form of congenital adrenal hyperplasia in newborn screening.
Archives of endocrinology and metabolismSturge-Weber syndrome with massive macroglossia and anterior neck space infection- a case report and review of literature.
JPMA. The Journal of the Pakistan Medical AssociationInfant with macroglossia.
Archives of disease in childhood. Education and practice editionPolyhydramnios associated with rare genetic syndromes: two case reports.
Journal of medical case reportsMacroglossia and lip edema: A case of paraproteinemia-associated scleredema responsive to intravenous immunoglobulins.
JAAD case reportsApplication of bilateral condylectomy as an alternative surgical treatment for Class III malocclusion with posterior vertical excess, a technical note.
Journal of stomatology, oral and maxillofacial surgeryFragile lip in a patient with macroglossia due to hemodialysis-associated amyloidosis.
JA clinical reportsPrecision medicine using whole genome sequencing identifies a novel dystrophin (DMD) variant for X-linked muscular dystrophy in a cat.
Journal of veterinary internal medicineLingual Abscess after Posterior Fossa Surgery: An Unusual Complication of the Concorde Position.
Asian journal of neurosurgeryHistotoxicity induced by copper oxide nanoparticles (CuO-NPs) on developing mice (Mus musculus).
Food and chemical toxicology : an international journal published for the British Industrial Biological Research AssociationComprehensive Preventive and Therapeutic Oral Health Care: A Case Report of Mucopolysaccharidosis Type IV A in a Pediatric Patient.
Puerto Rico health sciences journalComprehensive review of the timing of surgical management of macroglossia in Beckwith-Wiedemann syndrome.
Bratislavske lekarske listy[Giant tongue leading to dysphagia in light chain amyloidosis patient].
Revista medica del Instituto Mexicano del Seguro Social"Snail-Track Ulcers" And Macroglossia Due to Secondary Syphilis.
Dermatology practical & conceptualTongue and Mandibular Disorders of the Pediatric Patient.
Facial plastic surgery clinics of North AmericaCase 16: A 75-Year-Old Man With Macroglossia and Hypercalcemia.
Journal of Korean medical scienceMultisystem approach for management of OSA in Down syndrome: a case report.
Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep MedicineManagement of Macroglossia Secondary to Beckwith-Weidmann Syndrome in a Pediatric Patient: A Case Report.
CureusIntroduction to the Beckwith-Wiedemann Syndrome and Cancer Special Issue.
Cancers(Epi)genotype and Timing of Tongue Reduction Predict Safety and Long-Term Outcomes in Beckwith-Wiedemann Syndrome.
Plastic and reconstructive surgeryPediatric cancer incidence among individuals with overgrowth syndromes and overgrowth features: A population-based assessment in seven million children.
CancerKleefstra Syndrome-Dental Manifestations and Needs: A Case Report with a Literature Review.
Case reports in dentistrySupernumerary chromosome 6 marker associated with paternal uniparental isodisomy of chromosome 6 in a patient with a syndromic disorder of insulin secretion.
European journal of medical geneticsBeckwith-Wiedemann Syndrome in Newborn of Mother with HELLP Syndrome/Preeclampsia: An Analysis of Literature and Case Report with Fetal Growth Restriction and Absence of CDKN1C Typical Pathogenic Genetic Variation.
International journal of molecular sciencesOrofacial myofunctional therapy associated with the use of the stimulating palatal plate in children with trisomy 21: case studies.
CoDASAmyloidosis initially only manifesting as oral mucosal hemorrhagic lesions: a case series report.
Oral surgery, oral medicine, oral pathology and oral radiologyA Case Report on Obstructive Sleep Apnea in a Pediatric Patient with Achondroplasia.
Acta medica PhilippinaBeckwith-Wiedemann syndrome with multiple hepatic and cutaneous hemangiomas in a female patient of Albanian origin: Diagnostic and therapeutic considerations.
American journal of medical genetics. Part A[Macroglossia: compressiontherapy as an alternative treatment option].
Laryngo- rhino- otologieThe role of pediatric oncologist in prenatal diagnosis: A 10-year retrospective study at Assistance Publique Hôpitaux de Marseille (AP-HM).
Pediatric hematology and oncologyAssociations between the timing of tongue reduction surgery, (Epi)genotype, and dentoskeletal development in patients with Beckwith-Wiedemann syndrome.
Journal of cranio-maxillo-facial surgery : official publication of the European Association for Cranio-Maxillo-Facial SurgeryBeckwith-Wiedemann syndrome in a child with multifocal Wilms tumor and lateralized overgrowth: A case report.
Radiology case reportsAmyloid Deposition in the Upper Aerodigestive Tract, A Single Institute Experience.
Ear, nose, & throat journalOrofacial symptoms suggestive of malignant lesions and the role of imaging: literature review and case presentation.
Oral radiologyBeckwith-Wiedemann syndrome.
The Pan African medical journalMicroperimetric evaluation for different methods of epiretinal membrane surgery.
BMC ophthalmologyNasotracheal intubation awake in a patient with multiple fractures of the maxilla and cervical spine: A case report.
MedicineOpen Bite Malocclusion and Orofacial Dysfunction in Patients with Myotonic Dystrophy Type 1 and Duchenne Muscular Dystrophy.
Journal of neuromuscular diseasesOral amyloidosis: an update.
Medicina oral, patologia oral y cirugia bucalApplication of Original Therapy for Stimulation of Oral Areas Innervated by the Trigeminal Nerve in a Child with Beckwith-Wiedemann Syndrome.
Brain sciencesAdult experiences in Beckwith-Wiedemann syndrome.
American journal of medical genetics. Part C, Seminars in medical geneticsDentoskeletal features and growth pattern in Beckwith-Wiedemann spectrum: is surgical tongue reduction always necessary?
Clinical oral investigationsPhenotype Genotype Characterization of FKRP-related Muscular Dystrophy among Indian Patients.
Journal of neuromuscular diseasesHereditary transthyretin amyloidosis presenting with spontaneous periorbital purpura: a case report.
European heart journal. Case reportsFeatures of Obstructive Sleep Apnea in Children with and without Comorbidities.
Journal of clinical medicineMethodical control of the difficult pediatric airway: two case reports.
Journal of medical case reportsClinical, Phenotypic, and Demographic Characteristics of Peruvian Children and Neonates with Autosomal and Sex Chromosome Aneuploidies.
The Eurasian journal of medicineTwo emerging phenotypes of atypical inclusion body myositis: illustrative cases.
Clinical and experimental rheumatologyIndividualized treatment of congenital vascular malformations of the tongue.
Clinical hemorheology and microcirculationThe Efficacy of the Partial Glossectomy for Prevention of Airway Volume Reduction in Orthognathic Surgery of Class III Patients.
Life (Basel, Switzerland)Dystrophin (DMD) Missense Variant in Cats with Becker-Type Muscular Dystrophy.
International journal of molecular sciencesRecurrent PIK3CA H1047R-Mutated Congenital Infiltrative Facial Lipomatosis: A Case Report and Review of Literature.
Current issues in molecular biologyCT volumetric analysis permits comparison of tongue size and tongue fat in different canine brachycephalic and mesaticephalic breeds.
Veterinary radiology & ultrasound : the official journal of the American College of Veterinary Radiology and the International Veterinary Radiology AssociationA Delayed Diagnosis of Myxedema Coma.
CureusClinical relevance of macroglossia to disease progression in ventilation dependent patients with advanced ALS.
Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology[Preterm with Macroglossia and Persistent Hypoglycemia - Beckwith-Wiedemann Syndrome].
Zeitschrift fur Geburtshilfe und NeonatologieBeckwith-Widemann Macroglossia: The Role of Surgical Tongue Reduction.
The Cleft palate-craniofacial journal : official publication of the American Cleft Palate-Craniofacial AssociationWhat to Expect of Feeding Abilities and Nutritional Aspects in Achondroplasia Patients: A Narrative Review.
GenesInfantile hypothyroidism and its relationship with delayed tooth eruption: A case report.
Journal of clinical and experimental dentistryInvestigation of a pervasive immune, cardiac, and behavioral phenotype in Beckwith-Wiedemann syndrome: A case report.
American journal of medical genetics. Part ARadiographic, MRI, and CT findings in a young dog with Becker-like muscular dystrophy.
Veterinary radiology & ultrasound : the official journal of the American College of Veterinary Radiology and the International Veterinary Radiology AssociationLong-Term Follow-up With Multispecialty Management of a Giant Lymphangioma of an Infant Tongue Contributed to Reduced Complications of the Disease: A Case Report of a 21-Year Follow-up.
EplastyOral findings as predictors of obstructive sleep apnea- A case-control study.
Journal of family medicine and primary careCUL4B-associated epilepsy: Report of a novel truncating variant promoting drug-resistant seizures and systematic review of the literature.
SeizureMacroglossia as the first oral manifestation of dialysis-associated systemic amyloidosis.
Asian journal of surgeryBeckwith-Wiedemann syndrome with long QT caused by a deletion involving KCNQ1 but not KCNQ1OT1:TSS-DMR.
European journal of medical geneticsMacroglossia in rapidly progressive inclusion body myositis.
Neuropathology : official journal of the Japanese Society of NeuropathologyOrofacial abnormalities in mucopolysaccharidosis and mucolipidosis type II and III: A systematic review.
JIMD reportsTongue Reduction Surgery Improves Mandibular Prognathism in Beckwith-Wiedemann Syndrome Without Compromising Tongue Function.
Clinical and experimental otorhinolaryngologyFamilial Beckwith-Wiedemann syndrome in a multigenerational family: Forty years of careful phenotyping.
American journal of medical genetics. Part AMetastatic Phyllodes Tumor in a Patient With Beckwith-Wiedemann Syndrome.
Journal of investigative medicine high impact case reportsUltrasound and molecular prenatal diagnosis of Beckwith-Wiedemann syndrome: Two case reports.
Radiology case reportsIdentification of a novel pathogenic TBCK variant in a Chinese patient with infantile hypotonia with psychomotor retardation and characteristic facies type 3 (IHPRF3): a case report.
BMC pediatricsRisk factors for failed first intubation attempt in an out-of-hospital setting: a multicenter prospective study.
Internal and emergency medicineMacroglossia and less advanced dystrophic change in the tongue muscle of the Duchenne muscular dystrophy rat.
Skeletal muscleUsefulness of the MS-MLPA technique in the diagnosis of Beckwith-Wiedemann syndrome and Silver-Russell syndrome.
Gaceta medica de MexicoDouble Valve Replacement in a Patient With Hunter Syndrome.
CureusOral Health-Related Quality of Life among Children and Adolescents with Beckwith-Wiedemann Syndrome in Northern Italy.
Journal of clinical medicineEtiological diagnosis of macroglossia: Systematic review and diagnostic algorithm.
Annales de dermatologie et de venereologieFree Fibula Flap for the Treatment of Agnathia in a 10-Year-Old With Severe Agnathia-Otocephaly Complex.
The Journal of craniofacial surgeryMacroglossia associated with multiple nodular lesions of the tongue.
Oral diseasesManagement of MACROGLOSSIA: Case Series and Suggested Algorithm.
Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial SurgeonsTaming the Tongue: The Surgical Approach to Macroglossia.
The Journal of craniofacial surgeryPartial Glossectomy Combined With Radiofrequency Ablation for Macroglossia in Beckwith-Wiedemann Syndrome.
The Journal of craniofacial surgeryPrevalence of Dental Caries and Gingivitis among children with Intellectual Disability in India.
Journal of family medicine and primary careConsecutive Severe Orofacial Complications in Intensive Care Unit Patients: Quincke's Disease and Macroglossia due to Prolonged Prone Positioning for Management of Acute Respiratory Distress Syndrome.
European journal of case reports in internal medicineClinical Spectrum and Tumour Risk Analysis in Patients with Beckwith-Wiedemann Syndrome Due to CDKN1C Pathogenic Variants.
CancersTraumatic Macroglossia in a Patient With Rett Syndrome.
CureusMacroglossia as the initial presentation of AL amyloidosis: review and updates in treatment.
BMJ case reportsDeciphering Epigenetic Backgrounds in a Korean Cohort with Beckwith-Wiedemann Syndrome.
Annals of laboratory medicineAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Macroglossia.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Macroglossia
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Bilateral ovarian steroid cell tumor in a postmenopausal woman with progressive hyperandrogenism.
- [Guidelines for the diagnosis and treatment of obstructive sleep apnea in adults (2025)].Zhonghua jie he he hu xi za zhi = Zhonghua jiehe he huxi zazhi = Chinese journal of tuberculosis and respiratory diseases· 2026· PMID 41820035mais citado
- Patient-Reported Speech Outcomes in Patients with Beckwith-Wiedemann Syndrome.
- Tongue Reduction for Pediatric Obstructive Sleep Apnea: A Systematic Review.
- Obstructive Sleep Apnea-Hypopnea Syndrome in Children With Down Syndrome Treated at a Tertiary Care Hospital in Northeastern Colombia.
- Fissured Tongue associated with Hypothyroidism in a Young Patient.
- Tongue swelling following cleft palate repair: report of a rare case.
- The Natural Evolution of Macroglossia Among Beckwith-Wiedemann Patients: A 30-Year Institutional Review.
- PRS Journal Club: Cleft Palate Technique Outcomes, Primary Cleft Rhinoplasty Grafts, and Macroglossia Reduction.
- Discussion: A Comparison of Surgical Techniques for Macroglossia in Beckwith-Wiedemann Syndrome.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:156207(Orphanet)
- MONDO:0015496(MONDO)
- GARD:3342(GARD (NIH))
- Busca completa no PubMed(PubMed)
- Artigo Wikipedia(Wikipedia)
- Q524095(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar