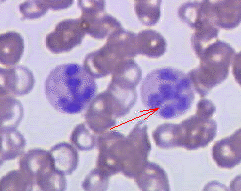
A anemia megaloblástica responsiva à tiamina (TRMA) é caracterizada por uma tríade de anemia megaloblástica, diabetes mellitus não tipo I e surdez neurossensorial.
Introdução
O que você precisa saber de cara
A anemia megaloblástica responsiva à tiamina (TRMA) é caracterizada por uma tríade de anemia megaloblástica, diabetes mellitus não tipo I e surdez neurossensorial.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 13 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 40 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
1 gene identificado com associação a esta condição. Padrão de herança: Autosomal recessive.
High-affinity transporter for the intake of thiamine (PubMed:10391222, PubMed:10542220, PubMed:21836059, PubMed:33008889, PubMed:35512554, PubMed:35724964). Mediates H(+)-dependent pyridoxine transport (PubMed:33008889, PubMed:35512554, PubMed:35724964)
Cell membrane
Thiamine-responsive megaloblastic anemia syndrome
An autosomal recessive disease characterized by megaloblastic anemia, diabetes mellitus, and sensorineural deafness. Onset is typically between infancy and adolescence, but all of the cardinal findings are often not present initially. The anemia, and sometimes the diabetes, improves with high doses of thiamine. Other more variable features include optic atrophy, congenital heart defects, short stature, and stroke.
Variantes genéticas (ClinVar)
115 variantes patogênicas registradas no ClinVar.
Vias biológicas (Reactome)
1 via biológica associada aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Síndrome anemia megaloblástica tiamina-sensível
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
Pesquisa e ensaios clínicos
0 ensaios clínicos encontrados.
Publicações mais relevantes
Thiamine-responsive megaloblastic anemia syndrome with novel compound heterozygous SLC19A2 mutations and thrombotic events: a case report.
Thiamine-responsive megaloblastic anemia syndrome represents a rare autosomal recessive condition originating from mutations in the SLC19A2 gene. It is characterized by a classical triad of megaloblastic anemia, insulin-dependent diabetes mellitus, and sensorineural hearing loss. We present the case of a woman diagnosed with thiamine-responsive megaloblastic anemia, with no history of consanguinity, in whom genetic testing revealed novel SLC19A2 mutations and an unreported clinical manifestation. This case describes an 18-year-old mestizo female patient who presented with a medical history of diabetes starting in infancy, bilateral sensorineural hearing loss, and megaloblastic anemia. The diagnosis of thiamine-responsive megaloblastic anemia was confirmed by genetic testing, which detected compound heterozygous mutations in the SLC19A2 gene that included a pathogenic frameshift mutation (c.620_624dup; p.Pro209Phefs*21) and a missense variant (c.170 T > C; p.Leu57Pro). The patient also experienced thrombotic events, including deep vein and mesenteric thrombosis, previously unreported findings in thiamine-responsive megaloblastic anemia. High-dose thiamine treatment resulted in improved hematologic and glycemic control. This case broadens the genetic and clinical spectrum of thiamine-responsive megaloblastic anemia, highlighting the importance of genetic testing in young patients with the classic triad and showing that early thiamine therapy can markedly improve outcomes.
Thiamine-Responsive Megaloblastic Anemia Syndrome: A Rare Syndromic Cause of Diabetes in Childhood.
Recurrent and Novel Pathogenic Variants in Genes Involved with Hearing Loss in the Pakistani Population.
Molecular diagnostic rates for hereditary hearing loss vary by genetic ancestry, highlighting the importance of population-specific studies. In Pakistan, where consanguineous marriages are prevalent, genetic research has identified many autosomal recessive genes, advancing understanding of rare and novel hearing loss mechanisms. This study aimed to identify pathogenic genetic variants in 31 families from Azad Kashmir, Pakistan, presenting non-syndromic hearing loss. We conducted exome sequencing and bioinformatics analysis, and targeted gene sequencing on 31 Pakistani families with hearing loss. We identified ten pathogenic, three likely pathogenic variants, and one variant of uncertain significance, comprising six nonsense, four missense, three frameshift, and one deep intronic variant, across ten hearing loss-associated genes (MYO15A, GJB2, SLC26A4, TMC1, HGF, TMIE, SLC19A2, KCNE1, ILDR, PCDH15 and MYO6) in 25 families. The overall diagnostic rate, including families with pathogenic and likely pathogenic variants, was 77.4%. GJB2 was the most frequently affected gene, identified in seven families. Thirteen out of 14 identified variants were homozygous. Notably, we identified two novel variants: MYO15A (NM_016239.4, DFNB3) c.870C>G, p.(Tyr290*) and MYO6 (NM_016239.4, DFNB37) c.3465del, p.(Pro1156Leufs*9). Additionally, we identified c.10475dupA, p.(Leu3493Alafs*25) in MYO15A (NM_016239.4, DFNB3) and c.617T>A, p.(Leu206*) in SLC26A4 (NM_000441.2, DFNB4), previously documented in ClinVar but unpublished. We also propose SLC19A2 as a candidate gene presenting as non-syndromic hearing loss, despite its association with thiamine-responsive megaloblastic anemia syndrome. Our work expands the genotypic and phenotypic spectrum of hearing loss by emphasizing the importance of investigating under-represented groups to identify unique genetic variants and clinical characteristics. Such efforts deepen understanding of genetic diversity in under-represented populations to improve diagnosis and treatment strategies.
Diagnosis of a patient with severe sensorineural hearing loss as the initial symptom caused by novel compound heterozygous variant in SLC19A2 gene.
Thiamine-Responsive Megaloblastic Anemia (TRMA) syndrome, caused by biallelic variants in the SLC19A2 gene, typically presents with a triad of megaloblastic anemia, diabetes mellitus, and sensorineural hearing loss. This study aims to determine the genetic etiology and clinical phenotype of a patient who presented with severe sensorineural hearing loss as the initial symptom, and to expand our understanding of the SLC19A2 variant spectrum. Proband-only whole-exome sequencing was performed to screen the candidate variants, which were subsequently validated by Sanger sequencing within the family. cDNA sequencing based on RT-PCR and TA cloning analysis was used to determine the effect of splicing variants on mRNA processing of SLC19A2 gene. Detailed clinical features were evaluated by a diagnostic hearing test, laboratory and imaging examination. A 2-year-5-month-old Chinese girl was diagnosed with diabetes mellitus and severe sensorineural hearing loss, without abnormal hemoglobin. DNA sequencing revealed a novel compound heterozygous variant of c.808-1G > A and c.1228C > T (p.Gln410*) in the SLC19A2 gene. Both variants were previously unreported. The c.808-1G > A splicing variant is located in intron 2 of SLC19A2, and is predicted to cause exon 3 skipping. The cDNA experiment confirmed this biological event, further indicating that the splicing variant can cause amino acid frameshift alteration (p.Glu270Valfs*10) in SLC19A2. We report a patient with TRMA syndrome (without anemia) caused by a novel compound heterozygous variant in SLC19A2 gene. This study suggests that the possibility of TRMA syndrome should be considered when encountering patients with early-onset severe sensorineural hearing loss in clinical practice. Level 4.
4-phenylbutyric acid attenuates diabetes mellitus secondary to thiamine-responsive megaloblastic anaemia syndrome by modulating endoplasmic reticulum stress.
Thiamine-responsive megaloblastic anaemia syndrome (TRMA) is a rare genetic disease caused by mutations in the SLC19A2 gene that encodes thiamine transporter 1 (THTR-1). The common manifestations are diabetes, anaemia, and deafness. The pathogenic mechanism has not yet been clarified. Rat pancreatic islet tumour cells INS.1 were used to construct cell lines stably overexpressing wild-type SLC19A2 and SLC19A2 (c.1409insT) mutants. The mRNA and protein expressions of THTR-1 and endoplasmic reticulum stress (ERS)-associated factors were detected by real-time fluorescence quantitative polymerase chain reaction (PCR) and western blot methods, respectively. Flow cytometry and cell counting kit-8 were used to analyse the effects of SLC19A2 (c.1409insT) mutation on cell apoptosis and proliferation, respectively. 4-Phenylbutyric acid (4-PBA), an ERS inhibitor, was administered to SLC19A2 (c.1409insT)-mutated INS.1 cells, and then the mRNA and protein expressions of ERS-related factors in cells were detected. Mutations in the SLC19A2 (c.1409insT) promote apoptosis and inhibit cell proliferation, thereby upregulating the mRNA and protein levels of ERS-associated factors glucose-regulated protein 78, protein kinase R-like endoplasmic reticulum kinase, C/EBP homologous protein, and activating transcription factor 4. 4-PBA could inhibit ERS caused by SLC19A2 (c.1409insT) mutations, downregulate mRNA and protein expression levels of GRP78, CHOP, and phosphorylated eukaryotic initiation factor 2α, and protect pancreatic islet β-cells. THTR-1 deficiency triggers diabetes in TRMA patients through ERS, and 4-PBA protects pancreatic islet β-cells by inhibiting ERS, which provides new ideas and intervention targets for the prevention and treatment of TRMA and diabetes.
Publicações recentes
Thiamine-responsive megaloblastic anemia syndrome with novel compound heterozygous SLC19A2 mutations and thrombotic events: a case report.
Thiamine-Responsive Megaloblastic Anemia Syndrome: A Rare Syndromic Cause of Diabetes in Childhood.
Recurrent and Novel Pathogenic Variants in Genes Involved with Hearing Loss in the Pakistani Population.
Diagnosis of a patient with severe sensorineural hearing loss as the initial symptom caused by novel compound heterozygous variant in SLC19A2 gene.
Thiamine-Responsive Megaloblastic Anemia Syndrome Mimicking Myelodysplastic Neoplasm.
📚 EuropePMC34 artigos no totalmostrando 41
Thiamine-responsive megaloblastic anemia syndrome with novel compound heterozygous SLC19A2 mutations and thrombotic events: a case report.
Journal of medical case reportsThiamine-Responsive Megaloblastic Anemia Syndrome: A Rare Syndromic Cause of Diabetes in Childhood.
Indian pediatricsRecurrent and Novel Pathogenic Variants in Genes Involved with Hearing Loss in the Pakistani Population.
Molecular diagnosis & therapyDiagnosis of a patient with severe sensorineural hearing loss as the initial symptom caused by novel compound heterozygous variant in SLC19A2 gene.
Brazilian journal of otorhinolaryngology4-phenylbutyric acid attenuates diabetes mellitus secondary to thiamine-responsive megaloblastic anaemia syndrome by modulating endoplasmic reticulum stress.
Endokrynologia PolskaThiamine-Responsive Megaloblastic Anemia Syndrome Mimicking Myelodysplastic Neoplasm.
Acta haematologicaThiamine-responsive megaloblastic anaemia in a young adult with acute pancytopenia.
BMJ case reports[Bibliometric visualization analysis of thiamine-responsive megaloblastic anemia syndrome].
Zhonghua yu fang yi xue za zhi [Chinese journal of preventive medicine]Thiamine-responsive megaloblastic anaemia.
The National medical journal of IndiaAn extremely rare case of Rogers syndrome or thiamine responsive megaloblastic anemia.
Indian journal of pathology & microbiologyAn Italian case series' description of thiamine responsive megaloblastic anemia syndrome: importance of early diagnosis and treatment.
Italian journal of pediatricsThiamine responsive megaloblastic anaemia complicated with acute Parvovirus infection: A case report.
JPMA. The Journal of the Pakistan Medical AssociationWhole-Exome Sequencing Revealed a Pathogenic Nonsense Variant in the SLC19A2 Gene in an Iranian Family with Thiamine-Responsive Megaloblastic Anemia.
Laboratory medicineLeber congenital amaurosis as an initial manifestation in a Chinese patient with thiamine-responsive megaloblastic anemia syndrome.
American journal of medical genetics. Part ACase Report: Genetic and Clinical Features of Maternal Uniparental Isodisomy-Induced Thiamine-Responsive Megaloblastic Anemia Syndrome.
Frontiers in pediatricsThe Effects of Genetic Mutations and Drugs on the Activity of the Thiamine Transporter, SLC19A2.
The AAPS journalIdentification of novel compound heterozygous variants in SLC19A2 and the genotype-phenotype associations in thiamine-responsive megaloblastic anemia.
Clinica chimica acta; international journal of clinical chemistryRelapse of rare diseases during COVID-19 pandemic: bicytopenia in an adult patient with thiamine-responsive megaloblastic anaemia.
The Pan African medical journalDyserythropoiesis and myelodysplasia in thiamine-responsive megaloblastic anemia syndrome.
Clinical case reportsA novel mutation in the SLC19A2 gene in a Turkish male with thiamine-responsive megaloblastic anemia syndrome.
The Turkish journal of pediatricsMutations in both SAMD9 and SLC19A2 genes caused complex phenotypes characterized by recurrent infection, dysphagia and profound deafness - a case report for dual diagnosis.
BMC pediatricsTRMA syndrome with a severe phenotype, cerebral infarction, and novel compound heterozygous SLC19A2 mutation: a case report.
BMC pediatricsNeonatal diabetes mellitus: remission induced by novel therapy.
BMJ case reportsWhole exome sequencing identifies a new mutation in the SLC19A2 gene leading to thiamine-responsive megaloblastic anemia in an Egyptian family.
Molecular genetics & genomic medicineAn Adult Case of Thiamine-Sensitive Megaloblastic Anemia Syndrome Accidentally Diagnosed Myelodysplastic Syndrome.
Journal of the College of Physicians and Surgeons--Pakistan : JCPSPGenetic defects of thiamine transport and metabolism: A review of clinical phenotypes, genetics, and functional studies.
Journal of inherited metabolic disease50 Years Ago in The Journal of Pediatrics: Thiamine-Responsive Megaloblastic Anemia.
The Journal of pediatricsArrhythmia in thiamine responsive megaloblastic anemia syndrome.
The Turkish journal of pediatricsThiamine Responsive Megaloblastic Anaemia, Diabetes Mellitus and Sensorineural Hearing Loss in a Child.
Journal of the College of Physicians and Surgeons--Pakistan : JCPSP[Thiamine-responsive megaloblastic anemia or Rogers syndrome: A literature review].
La Revue de medecine interneA Novel Mutation of SLC19A2 in a Chinese Zhuang Ethnic Family with Thiamine-Responsive Megaloblastic Anemia.
Cellular physiology and biochemistry : international journal of experimental cellular physiology, biochemistry, and pharmacologyPancytopenia in an adult patient with thiamine-responsive megaloblastic anaemia.
BMJ case reportsPharmacogenomics in diabetes: outcomes of thiamine therapy in TRMA syndrome.
Diabetologia[Defect of thiamine transport and activation and related disease].
Zhonghua yi xue yi chuan xue za zhi = Zhonghua yixue yichuanxue zazhi = Chinese journal of medical geneticsRecurrent Stroke in a Child with TRMA Syndrome and SLC19A2 Gene Mutation.
Iranian journal of child neurologyInfantile-onset thiamine responsive megaloblastic anemia syndrome with SLC19A2 mutation: a case report.
Archivos argentinos de pediatriaMonogenic diabetes syndromes: Locus-specific databases for Alström, Wolfram, and Thiamine-responsive megaloblastic anemia.
Human mutationBeta cell function and clinical course in three siblings with thiamine-responsive megaloblastic anemia (TRMA) treated with thiamine supplementation.
Journal of pediatric endocrinology & metabolism : JPEMFirst 2 cases with thiamine-responsive megaloblastic anemia in the Czech Republic, a rare form of monogenic diabetes mellitus: a novel mutation in the thiamine transporter SLC19A2 gene-intron 1 mutation c.204+2T>G.
Pediatric diabetesNovel nonsense mutation (p.Ile411Metfs*12) in the SLC19A2 gene causing Thiamine Responsive Megaloblastic Anemia in an Indian patient.
Clinica chimica acta; international journal of clinical chemistryThiamine responsive megaloblastic anemia syndrome: a novel homozygous SLC19A2 gene mutation identified.
American journal of medical genetics. Part AAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Síndrome anemia megaloblástica tiamina-sensível.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Síndrome anemia megaloblástica tiamina-sensível
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Thiamine-responsive megaloblastic anemia syndrome with novel compound heterozygous SLC19A2 mutations and thrombotic events: a case report.
- Thiamine-Responsive Megaloblastic Anemia Syndrome: A Rare Syndromic Cause of Diabetes in Childhood.
- Recurrent and Novel Pathogenic Variants in Genes Involved with Hearing Loss in the Pakistani Population.
- Diagnosis of a patient with severe sensorineural hearing loss as the initial symptom caused by novel compound heterozygous variant in SLC19A2 gene.
- 4-phenylbutyric acid attenuates diabetes mellitus secondary to thiamine-responsive megaloblastic anaemia syndrome by modulating endoplasmic reticulum stress.
- Thiamine-Responsive Megaloblastic Anemia Syndrome Mimicking Myelodysplastic Neoplasm.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:49827(Orphanet)
- OMIM OMIM:249270(OMIM)
- MONDO:0009575(MONDO)
- GARD:9210(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Q2857909(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar