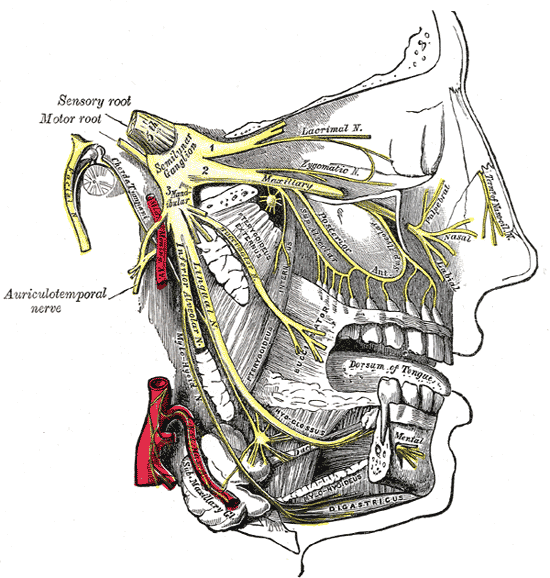
Cefaleia caracterizada por dor orbital, supraorbital e/ou temporal unilateral intensa e periódica, associada a sintomas autonômicos cranianos ipsilaterais.
Introdução
O que você precisa saber de cara
Cefaleia caracterizada por dor orbital, supraorbital e/ou temporal unilateral intensa e periódica, associada a sintomas autonômicos cranianos ipsilaterais.
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 8 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Nenhum gene associado encontrado
Os dados genéticos desta condição ainda estão sendo catalogados.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — NÃO RARA NA EUROPA: Cefaleia em salvas
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
🟢 Recrutando agora
1 pesquisa recrutando participantes. Converse com seu médico sobre a possibilidade de participar.
Outros ensaios clínicos
0 ensaios clínicos encontrados.
Publicações mais relevantes
Global burden of 292 causes of death in 204 countries and territories and 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
Timely and comprehensive analyses of causes of death stratified by age, sex, and location are essential for shaping effective health policies aimed at reducing global mortality. The Global Burden of Diseases, Injuries, and Risk Factors Study (GBD) 2023 provides cause-specific mortality estimates measured in counts, rates, and years of life lost (YLLs). GBD 2023 aimed to enhance our understanding of the relationship between age and cause of death by quantifying the probability of dying before age 70 years (70q0) and the mean age at death by cause and sex. This study enables comparisons of the impact of causes of death over time, offering a deeper understanding of how these causes affect global populations. GBD 2023 produced estimates for 292 causes of death disaggregated by age-sex-location-year in 204 countries and territories and 660 subnational locations for each year from 1990 until 2023. We used a modelling tool developed for GBD, the Cause of Death Ensemble model (CODEm), to estimate cause-specific death rates for most causes. We computed YLLs as the product of the number of deaths for each cause-age-sex-location-year and the standard life expectancy at each age. Probability of death was calculated as the chance of dying from a given cause in a specific age period, for a specific population. Mean age at death was calculated by first assigning the midpoint age of each age group for every death, followed by computing the mean of all midpoint ages across all deaths attributed to a given cause. We used GBD death estimates to calculate the observed mean age at death and to model the expected mean age across causes, sexes, years, and locations. The expected mean age reflects the expected mean age at death for individuals within a population, based on global mortality rates and the population's age structure. Comparatively, the observed mean age represents the actual mean age at death, influenced by all factors unique to a location-specific population, including its age structure. As part of the modelling process, uncertainty intervals (UIs) were generated using the 2·5th and 97·5th percentiles from a 250-draw distribution for each metric. Findings are reported as counts and age-standardised rates. Methodological improvements for cause-of-death estimates in GBD 2023 include a correction for the misclassification of deaths due to COVID-19, updates to the method used to estimate COVID-19, and updates to the CODEm modelling framework. This analysis used 55 761 data sources, including vital registration and verbal autopsy data as well as data from surveys, censuses, surveillance systems, and cancer registries, among others. For GBD 2023, there were 312 new country-years of vital registration cause-of-death data, 3 country-years of surveillance data, 51 country-years of verbal autopsy data, and 144 country-years of other data types that were added to those used in previous GBD rounds. The initial years of the COVID-19 pandemic caused shifts in long-standing rankings of the leading causes of global deaths: it ranked as the number one age-standardised cause of death at Level 3 of the GBD cause classification hierarchy in 2021. By 2023, COVID-19 dropped to the 20th place among the leading global causes, returning the rankings of the leading two causes to those typical across the time series (ie, ischaemic heart disease and stroke). While ischaemic heart disease and stroke persist as leading causes of death, there has been progress in reducing their age-standardised mortality rates globally. Four other leading causes have also shown large declines in global age-standardised mortality rates across the study period: diarrhoeal diseases, tuberculosis, stomach cancer, and measles. Other causes of death showed disparate patterns between sexes, notably for deaths from conflict and terrorism in some locations. A large reduction in age-standardised rates of YLLs occurred for neonatal disorders. Despite this, neonatal disorders remained the leading cause of global YLLs over the period studied, except in 2021, when COVID-19 was temporarily the leading cause. Compared to 1990, there has been a considerable reduction in total YLLs in many vaccine-preventable diseases, most notably diphtheria, pertussis, tetanus, and measles. In addition, this study quantified the mean age at death for all-cause mortality and cause-specific mortality and found noticeable variation by sex and location. The global all-cause mean age at death increased from 46·8 years (95% UI 46·6-47·0) in 1990 to 63·4 years (63·1-63·7) in 2023. For males, mean age increased from 45·4 years (45·1-45·7) to 61·2 years (60·7-61·6), and for females it increased from 48·5 years (48·1-48·8) to 65·9 years (65·5-66·3), from 1990 to 2023. The highest all-cause mean age at death in 2023 was found in the high-income super-region, where the mean age for females reached 80·9 years (80·9-81·0) and for males 74·8 years (74·8-74·9). By comparison, the lowest all-cause mean age at death occurred in sub-Saharan Africa, where it was 38·0 years (37·5-38·4) for females and 35·6 years (35·2-35·9) for males in 2023. Lastly, our study found that all-cause 70q0 decreased across each GBD super-region and region from 2000 to 2023, although with large variability between them. For females, we found that 70q0 notably increased from drug use disorders and conflict and terrorism. Leading causes that increased 70q0 for males also included drug use disorders, as well as diabetes. In sub-Saharan Africa, there was an increase in 70q0 for many non-communicable diseases (NCDs). Additionally, the mean age at death from NCDs was lower than the expected mean age at death for this super-region. By comparison, there was an increase in 70q0 for drug use disorders in the high-income super-region, which also had an observed mean age at death lower than the expected value. We examined global mortality patterns over the past three decades, highlighting-with enhanced estimation methods-the impacts of major events such as the COVID-19 pandemic, in addition to broader trends such as increasing NCDs in low-income regions that reflect ongoing shifts in the global epidemiological transition. This study also delves into premature mortality patterns, exploring the interplay between age and causes of death and deepening our understanding of where targeted resources could be applied to further reduce preventable sources of mortality. We provide essential insights into global and regional health disparities, identifying locations in need of targeted interventions to address both communicable and non-communicable diseases. There is an ever-present need for strengthened health-care systems that are resilient to future pandemics and the shifting burden of disease, particularly among ageing populations in regions with high mortality rates. Robust estimates of causes of death are increasingly essential to inform health priorities and guide efforts toward achieving global health equity. The need for global collaboration to reduce preventable mortality is more important than ever, as shifting burdens of disease are affecting all nations, albeit at different paces and scales. Gates Foundation.
Burden of 375 diseases and injuries, risk-attributable burden of 88 risk factors, and healthy life expectancy in 204 countries and territories, including 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
For more than three decades, the Global Burden of Diseases, Injuries, and Risk Factors Study (GBD) has provided a framework to quantify health loss due to diseases, injuries, and associated risk factors. This paper presents GBD 2023 findings on disease and injury burden and risk-attributable health loss, offering a global audit of the state of world health to inform public health priorities. This work captures the evolving landscape of health metrics across age groups, sexes, and locations, while reflecting on the remaining post-COVID-19 challenges to achieving our collective global health ambitions. The GBD 2023 combined analysis estimated years lived with disability (YLDs), years of life lost (YLLs), and disability-adjusted life-years (DALYs) for 375 diseases and injuries, and risk-attributable burden associated with 88 modifiable risk factors. Of the more than 310 000 total data sources used for all GBD 2023 (about 30% of which were new to this estimation round), more than 120 000 sources were used for estimation of disease and injury burden and 59 000 for risk factor estimation, and included vital registration systems, surveys, disease registries, and published scientific literature. Data were analysed using previously established modelling approaches, such as disease modelling meta-regression version 2.1 (DisMod-MR 2.1) and comparative risk assessment methods. Diseases and injuries were categorised into four levels on the basis of the established GBD cause hierarchy, as were risk factors using the GBD risk hierarchy. Estimates stratified by age, sex, location, and year from 1990 to 2023 were focused on disease-specific time trends over the 2010-23 period and presented as counts (to three significant figures) and age-standardised rates per 100 000 person-years (to one decimal place). For each measure, 95% uncertainty intervals [UIs] were calculated with the 2·5th and 97·5th percentile ordered values from a 250-draw distribution. Total numbers of global DALYs grew 6·1% (95% UI 4·0-8·1), from 2·64 billion (2·46-2·86) in 2010 to 2·80 billion (2·57-3·08) in 2023, but age-standardised DALY rates, which account for population growth and ageing, decreased by 12·6% (11·0-14·1), revealing large long-term health improvements. Non-communicable diseases (NCDs) contributed 1·45 billion (1·31-1·61) global DALYs in 2010, increasing to 1·80 billion (1·63-2·03) in 2023, alongside a concurrent 4·1% (1·9-6·3) reduction in age-standardised rates. Based on DALY counts, the leading level 3 NCDs in 2023 were ischaemic heart disease (193 million [176-209] DALYs), stroke (157 million [141-172]), and diabetes (90·2 million [75·2-107]), with the largest increases in age-standardised rates since 2010 occurring for anxiety disorders (62·8% [34·0-107·5]), depressive disorders (26·3% [11·6-42·9]), and diabetes (14·9% [7·5-25·6]). Remarkable health gains were made for communicable, maternal, neonatal, and nutritional (CMNN) diseases, with DALYs falling from 874 million (837-917) in 2010 to 681 million (642-736) in 2023, and a 25·8% (22·6-28·7) reduction in age-standardised DALY rates. During the COVID-19 pandemic, DALYs due to CMNN diseases rose but returned to pre-pandemic levels by 2023. From 2010 to 2023, decreases in age-standardised rates for CMNN diseases were led by rate decreases of 49·1% (32·7-61·0) for diarrhoeal diseases, 42·9% (38·0-48·0) for HIV/AIDS, and 42·2% (23·6-56·6) for tuberculosis. Neonatal disorders and lower respiratory infections remained the leading level 3 CMNN causes globally in 2023, although both showed notable rate decreases from 2010, declining by 16·5% (10·6-22·0) and 24·8% (7·4-36·7), respectively. Injury-related age-standardised DALY rates decreased by 15·6% (10·7-19·8) over the same period. Differences in burden due to NCDs, CMNN diseases, and injuries persisted across age, sex, time, and location. Based on our risk analysis, nearly 50% (1·27 billion [1·18-1·38]) of the roughly 2·80 billion total global DALYs in 2023 were attributable to the 88 risk factors analysed in GBD. Globally, the five level 3 risk factors contributing the highest proportion of risk-attributable DALYs were high systolic blood pressure (SBP), particulate matter pollution, high fasting plasma glucose (FPG), smoking, and low birthweight and short gestation-with high SBP accounting for 8·4% (6·9-10·0) of total DALYs. Of the three overarching level 1 GBD risk factor categories-behavioural, metabolic, and environmental and occupational-risk-attributable DALYs rose between 2010 and 2023 only for metabolic risks, increasing by 30·7% (24·8-37·3); however, age-standardised DALY rates attributable to metabolic risks decreased by 6·7% (2·0-11·0) over the same period. For all but three of the 25 leading level 3 risk factors, age-standardised rates dropped between 2010 and 2023-eg, declining by 54·4% (38·7-65·3) for unsafe sanitation, 50·5% (33·3-63·1) for unsafe water source, and 45·2% (25·6-72·0) for no access to handwashing facility, and by 44·9% (37·3-53·5) for child growth failure. The three leading level 3 risk factors for which age-standardised attributable DALY rates rose were high BMI (10·5% [0·1 to 20·9]), drug use (8·4% [2·6 to 15·3]), and high FPG (6·2% [-2·7 to 15·6]; non-significant). Our findings underscore the complex and dynamic nature of global health challenges. Since 2010, there have been large decreases in burden due to CMNN diseases and many environmental and behavioural risk factors, juxtaposed with sizeable increases in DALYs attributable to metabolic risk factors and NCDs in growing and ageing populations. This long-observed consequence of the global epidemiological transition was only temporarily interrupted by the COVID-19 pandemic. The substantially decreasing CMNN disease burden, despite the 2008 global financial crisis and pandemic-related disruptions, is one of the greatest collective public health successes known. However, these achievements are at risk of being reversed due to major cuts to development assistance for health globally, the effects of which will hit low-income countries with high burden the hardest. Without sustained investment in evidence-based interventions and policies, progress could stall or reverse, leading to widespread human costs and geopolitical instability. Moreover, the rising NCD burden necessitates intensified efforts to mitigate exposure to leading risk factors-eg, air pollution, smoking, and metabolic risks, such as high SBP, BMI, and FPG-including policies that promote food security, healthier diets, physical activity, and equitable and expanded access to potential treatments, such as GLP-1 receptor agonists. Decisive, coordinated action is needed to address long-standing yet growing health challenges, including depressive and anxiety disorders. Yet this can be only part of the solution. Our response to the NCD syndemic-the complex interaction of multiple health risks, social determinants, and systemic challenges-will define the future landscape of global health. To ensure human wellbeing, economic stability, and social equity, global action to sustain and advance health gains must prioritise reducing disparities by addressing socioeconomic and demographic determinants, ensuring equitable health-care access, tackling malnutrition, strengthening health systems, and improving vaccination coverage. We live in times of great opportunity. Gates Foundation and Bloomberg Philanthropies.
Global, Regional, and National Burden of Nontraumatic Subarachnoid Hemorrhage: The Global Burden of Disease Study 2021.
Nontraumatic subarachnoid hemorrhage (SAH) represents the third most common stroke type with unique etiologies, risk factors, diagnostics, and treatments. Nevertheless, epidemiological studies often cluster SAH with other stroke types leaving its distinct burden estimates obscure. To estimate the worldwide burden of SAH. Based on the repeated cross-sectional Global Burden of Disease (GBD) 2021 study, the global burden of SAH in 1990 to 2021 was estimated. Moreover, the SAH burden was compared with other diseases, and its associations with 14 individual risk factors were investigated with available data in the GBD 2021 study. The GBD study included the burden estimates of nontraumatic SAH among all ages in 204 countries and territories between 1990 and 2021. SAH and 14 modifiable risk factors. Absolute numbers and age-standardized rates with 95% uncertainty intervals (UIs) of SAH incidence, prevalence, mortality, and disability-adjusted life-years (DALYs) as well as risk factor-specific population attributable fractions (PAFs). In 2021, the global age-standardized SAH incidence was 8.3 (95% UI, 7.3-9.5), prevalence was 92.2 (95% UI, 84.1-100.6), mortality was 4.2 (95% UI, 3.7-4.8), and DALY rate was 125.2 (95% UI, 110.5-142.6) per 100 000 people. The highest burden estimates were found in Latin America, the Caribbean, Oceania, and high-income Asia Pacific. Although the absolute number of SAH cases increased, especially in regions with a low sociodemographic index, all age-standardized burden rates decreased between 1990 and 2021: the incidence by 28.8% (95% UI, 25.7%-31.6%), prevalence by 16.1% (95% UI, 14.8%-17.7%), mortality by 56.1% (95% UI, 40.7%-64.3%), and DALY rate by 54.6% (95% UI, 42.8%-61.9%). Of 300 diseases, SAH ranked as the 36th most common cause of death and 59th most common cause of DALY in the world. Of all worldwide SAH-related DALYs, 71.6% (95% UI, 63.8%-78.6%) were associated with the 14 modeled risk factors of which high systolic blood pressure (population attributable fraction [PAF] = 51.6%; 95% UI, 38.0%-62.6%) and smoking (PAF = 14.4%; 95% UI, 12.4%-16.5%) had the highest attribution. Although the global age-standardized burden rates of SAH more than halved over the last 3 decades, SAH remained one of the most common cardiovascular and neurological causes of death and disabilities in the world, with increasing absolute case numbers. These findings suggest evidence for the potential health benefits of proactive public health planning and resource allocation toward the prevention of SAH.
Characterising acute and chronic care needs: insights from the Global Burden of Disease Study 2019.
Chronic care manages long-term, progressive conditions, while acute care addresses short-term conditions. Chronic conditions increasingly strain health systems, which are often unprepared for these demands. This study examines the burden of conditions requiring acute versus chronic care, including sequelae. Conditions and sequelae from the Global Burden of Diseases Study 2019 were classified into acute or chronic care categories. Data were analysed by age, sex, and socio-demographic index, presenting total numbers and contributions to burden metrics such as Disability-Adjusted Life Years (DALYs), Years Lived with Disability (YLD), and Years of Life Lost (YLL). Approximately 68% of DALYs were attributed to chronic care, while 27% were due to acute care. Chronic care needs increased with age, representing 86% of YLDs and 71% of YLLs, and accounting for 93% of YLDs from sequelae. These findings highlight that chronic care needs far exceed acute care needs globally, necessitating health systems to adapt accordingly.
The profile of refractory chronic cluster headache.
Chronic cluster headache (CCH) is a relatively rare primary headache disorder whose management is often challenging. The prevalence of refractory CCH (rCCH) is unknown. Our aim is to describe the frequency of rCCH within a population of CCH, define the clinical profile of the refractory patients and the treatments they underwent. We conducted a cross-sectional study through a review of the medical records of CCH patients in six hospitals in Madrid, Spain. Data on epidemiological, clinical presentation, treatment and disease activity at the moment were collected. The European Headache Federation diagnostic criteria were used for rCCH definition. High disease activity was defined as having at least 3 severe attacks per week that impact quality of life despite treatment. Non-rCCH and rCCH groups were compared. 88 CCH patients were analyzed, 68.2% (60/88) met rCCH criteria at some point in their evolution. A longer diagnostic delay (4.6 ± 7.1 vs. 3.2 ± 3.7 years, p = 0.017) was observed in rCCH. All rCCH patients tried therapies without established evidence from randomized clinical trials. OnabotulinumtoxinA and galcanezumab were initiated in 77.3% (68/88) and 5.7% (5/88), but discontinued in 52.9% (36/68) and 60.0% (3/5), respectively. Occipital nerve stimulation (ONS) was implanted in 29.6% (26/88), with 50.0% (13/26) still active. Other treatment options are described and discussed. Despite treatment, 60.2% (53/88) still have high disease activity. CCH is a disorder with poor prognosis, meeting refractoriness criteria in more than half. OnabotulinumtoxinA and ONS could be the effective in refractory patients.
Publicações recentes
Ver todas no PubMed📚 EuropePMCmostrando 6
Global burden of 292 causes of death in 204 countries and territories and 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
Lancet (London, England)Burden of 375 diseases and injuries, risk-attributable burden of 88 risk factors, and healthy life expectancy in 204 countries and territories, including 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
Lancet (London, England)Global, Regional, and National Burden of Nontraumatic Subarachnoid Hemorrhage: The Global Burden of Disease Study 2021.
JAMA neurologyCharacterising acute and chronic care needs: insights from the Global Burden of Disease Study 2019.
Nature communicationsThe profile of refractory chronic cluster headache.
Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical NeurophysiologyCase report: A fatal case of cryptococcosis in an immunocompetent patient due to Cryptococcus deuterogattii (AFLP6/VGII).
JMM case reportsAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para NÃO RARA NA EUROPA: Cefaleia em salvas.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para NÃO RARA NA EUROPA: Cefaleia em salvas
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Global burden of 292 causes of death in 204 countries and territories and 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
- Burden of 375 diseases and injuries, risk-attributable burden of 88 risk factors, and healthy life expectancy in 204 countries and territories, including 660 subnational locations, 1990-2023: a systematic analysis for the Global Burden of Disease Study 2023.
- Global, Regional, and National Burden of Nontraumatic Subarachnoid Hemorrhage: The Global Burden of Disease Study 2021.
- Characterising acute and chronic care needs: insights from the Global Burden of Disease Study 2019.
- The profile of refractory chronic cluster headache.Neurological sciences : official journal of the Italian Neurological Society and of the Italian Society of Clinical Neurophysiology· 2025· PMID 39044103mais citado
- Cefaleia em Salvas em Crianças e Adolescentes: Uma revisão sistemática de relatos de casos.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:1002(Orphanet)
- MONDO:0043537(MONDO)
- Busca completa no PubMed(PubMed)
- Q55780428(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar