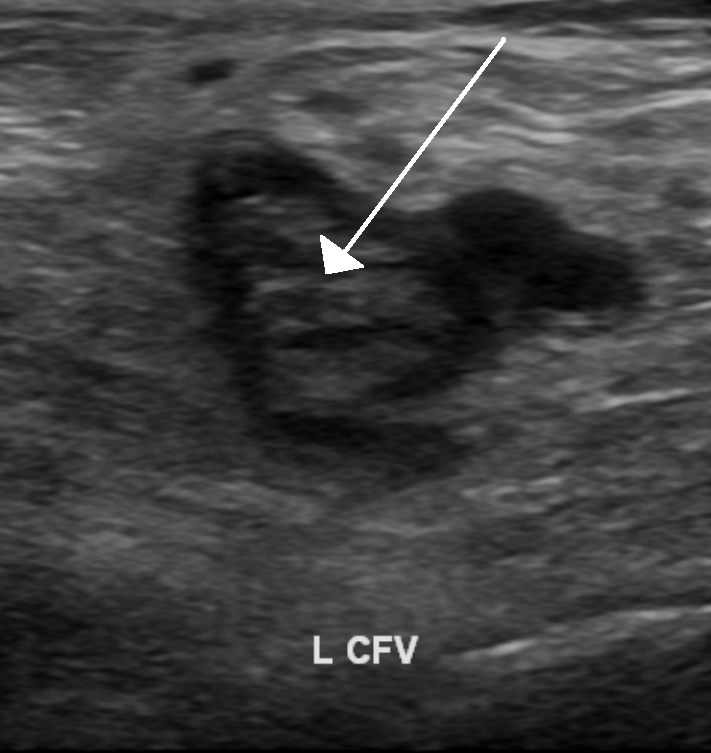
A deficiência congênita de proteína C é um distúrbio hereditário da coagulação caracterizado por sintomas de trombose venosa profunda devido à redução da síntese e/ou níveis de atividade da proteína C.
Introdução
O que você precisa saber de cara
A deficiência congênita de proteína C é um distúrbio hereditário da coagulação caracterizado por sintomas de trombose venosa profunda devido à redução da síntese e/ou níveis de atividade da proteína C.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 6 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 22 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
1 gene identificado com associação a esta condição. Padrão de herança: Autosomal dominant, Autosomal recessive.
Protein C is a vitamin K-dependent serine protease that regulates blood coagulation by inactivating factors Va and VIIIa in the presence of calcium ions and phospholipids (PubMed:25618265, PubMed:39880037). Exerts a protective effect on the endothelial cell barrier function (PubMed:25651845)
SecretedGolgi apparatusEndoplasmic reticulum
Thrombophilia due to protein C deficiency, autosomal dominant
A hemostatic disorder characterized by impaired regulation of blood coagulation and a tendency to recurrent venous thrombosis. Individuals with decreased amounts of protein C are classically referred to as having type I protein C deficiency and those with normal amounts of a functionally defective protein as having type II deficiency.
Medicamentos aprovados (FDA)
1 medicamento encontrado nos registros da FDA americana.
Variantes genéticas (ClinVar)
182 variantes patogênicas registradas no ClinVar.
Vias biológicas (Reactome)
8 vias biológicas associadas aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Trombofilia hereditária grave por deficiência de proteína C congênita
Centros de Referência SUS
24 centros habilitados pelo SUS para Trombofilia hereditária grave por deficiência de proteína C congênita
Centros para Trombofilia hereditária grave por deficiência de proteína C congênita
Detalhes dos centros
Hospital Universitário Prof. Edgard Santos (HUPES)
R. Dr. Augusto Viana, s/n - Canela, Salvador - BA, 40110-060 · CNES 0003808
Serviço de Referência
Hospital Infantil Albert Sabin
R. Tertuliano Sales, 544 - Vila União, Fortaleza - CE, 60410-794 · CNES 2407876
Serviço de Referência
Hospital de Apoio de Brasília (HAB)
AENW 3 Lote A Setor Noroeste - Plano Piloto, Brasília - DF, 70684-831 · CNES 0010456
Serviço de Referência
Hospital Estadual Infantil e Maternidade Alzir Bernardino Alves (HIABA)
Av. Min. Salgado Filho, 918 - Soteco, Vila Velha - ES, 29106-010 · CNES 6631207
Serviço de Referência
Hospital das Clínicas da UFG
Rua 235 QD. 68 Lote Área, Nº 285, s/nº - Setor Leste Universitário, Goiânia - GO, 74605-050 · CNES 2338424
Serviço de Referência
Hospital Universitário da UFJF
R. Catulo Breviglieri, Bairro - s/n - Santa Catarina, Juiz de Fora - MG, 36036-110 · CNES 2297442
Atenção Especializada
Hospital das Clínicas da UFMG
Av. Prof. Alfredo Balena, 110 - Santa Efigênia, Belo Horizonte - MG, 30130-100 · CNES 2280167
Serviço de Referência
Hospital Universitário Julio Müller (HUJM)
R. Luis Philippe Pereira Leite, s/n - Alvorada, Cuiabá - MT, 78048-902 · CNES 2726092
Atenção Especializada
Hospital Universitário João de Barros Barreto
R. dos Mundurucus, 4487 - Guamá, Belém - PA, 66073-000 · CNES 2337878
Serviço de Referência
Hospital Universitário Lauro Wanderley (HULW)
R. Tabeliao Estanislau Eloy, 585 - Castelo Branco, João Pessoa - PB, 58050-585 · CNES 0002470
Atenção Especializada
Instituto de Medicina Integral Prof. Fernando Figueira (IMIP)
R. dos Coelhos, 300 - Boa Vista, Recife - PE, 50070-902 · CNES 0000647
Serviço de Referência
Hospital Pequeno Príncipe
R. Des. Motta, 1070 - Água Verde, Curitiba - PR, 80250-060 · CNES 3143805
Serviço de Referência
Hospital Universitário Regional de Maringá (HUM)
Av. Mandacaru, 1590 - Parque das Laranjeiras, Maringá - PR, 87083-240 · CNES 2216108
Atenção Especializada
Hospital de Clínicas da UFPR
R. Gen. Carneiro, 181 - Alto da Glória, Curitiba - PR, 80060-900 · CNES 2364980
Serviço de Referência
Hospital Universitário Pedro Ernesto (HUPE-UERJ)
Blvd. 28 de Setembro, 77 - Vila Isabel, Rio de Janeiro - RJ, 20551-030 · CNES 2280221
Serviço de Referência
Instituto Nacional de Saúde da Mulher, da Criança e do Adolescente Fernandes Figueira (IFF/Fiocruz)
Av. Rui Barbosa, 716 - Flamengo, Rio de Janeiro - RJ, 22250-020 · CNES 2269988
Serviço de Referência
Hospital São Lucas da PUCRS
Av. Ipiranga, 6690 - Jardim Botânico, Porto Alegre - RS, 90610-000 · CNES 2232928
Serviço de Referência
Hospital de Clínicas de Porto Alegre (HCPA)
Rua Ramiro Barcelos, 2350 Bloco A - Av. Protásio Alves, 211 - Bloco B e C - Santa Cecília, Porto Alegre - RS, 90035-903 · CNES 2237601
Serviço de Referência
Hospital Universitário da UFSC (HU-UFSC)
R. Profa. Maria Flora Pausewang - Trindade, Florianópolis - SC, 88036-800 · CNES 2560356
Serviço de Referência
Hospital das Clínicas da FMUSP
R. Dr. Ovídio Pires de Campos, 225 - Cerqueira César, São Paulo - SP, 05403-010 · CNES 2077485
Serviço de Referência
Hospital de Base de São José do Rio Preto
Av. Brg. Faria Lima, 5544 - Vila Sao Jose, São José do Rio Preto - SP, 15090-000 · CNES 2079798
Atenção Especializada
Hospital de Clínicas da UNICAMP
R. Vital Brasil, 251 - Cidade Universitária, Campinas - SP, 13083-888 · CNES 2748223
Serviço de Referência
Hospital de Clínicas de Ribeirão Preto (HCRP-USP)
R. Ten. Catão Roxo, 3900 - Vila Monte Alegre, Ribeirão Preto - SP, 14015-010 · CNES 2082187
Serviço de Referência
UNIFESP / Hospital São Paulo
R. Napoleão de Barros, 715 - Vila Clementino, São Paulo - SP, 04024-002 · CNES 2688689
Serviço de Referência
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Ensaios em destaque
🟢 Recrutando agora
2 pesquisas recrutando participantes. Converse com seu médico sobre a possibilidade de participar.
Outros ensaios clínicos
0 ensaios clínicos encontrados.
Publicações mais relevantes
Mostrando amostra de 6 publicações de um total de 44
Clinical implications of genetic testing for congenital protein C deficiency in pregnancy.
Congenital protein C (PC) deficiency is a mostly autosomal dominant hereditary thrombophilia associated with early onset arterial and venous thrombotic diseases. In newborns, PC deficiency results in severe complications such as cerebral hemorrhage, cerebral infarction, and purpura fulminans, leading to death in some cases. We report two cases of deep vein thrombosis diagnosed during pregnancy that prompted genetic testing confirming definitive congenital PC deficiency. One patient with deep vein thrombosis at 30 weeks of gestation underwent anticoagulation therapy with the placement of an inferior vena cava filter. Genetic testing revealed a missense mutation in the PC gene. Another patient developed deep vein thrombosis at 9 weeks of gestation and received anticoagulant therapy, revealing a frameshift mutation in the gene. Genetic testing confirming congenital PC deficiency facilitates tailored postpartum management, including long-term anticoagulation therapy, based on the mother's thrombosis risk. For newborns, early diagnosis allows timely preparation of treatments, such as freshly thawed frozen plasma or PC replacement therapy and ensures closer monitoring through imaging evaluations, enabling early intervention to decrease the severity of potential complications. Given its utility in managing maternal and neonatal outcomes, early genetic testing in suspected cases of maternal PC deficiency is crucial before delivery.
Analysis of PROC mutations and clinical features in 22 unrelated families with inherited protein C deficiency.
Currently, limited information is available in the literature regarding the relationships between PROC mutations and clinical features in Chinese individuals. We aimed to characterize severe congenital Protein C deficiency in 22 unrelated Chinese families in a tertiary hospital by analyzing its clinical manifestation, associated risk factors, and gene mutations. We measured protein C activity and antigen levels for all participants, screened them for mutations in the PROC gene, and analyzed the clinical features of each family to identify commonalities and differences. The analysis revealed a total of 75 individuals with PCD and 16 different PROC mutations, including 12 missense mutations and 4 deletion mutations. Among them, 11 who were compound heterozygotes or homozygotes for mutations tended to develop symptoms at a younger age without any clear triggers. In contrast, the remaining 64 individuals who were heterozygotes for mutations often had clear triggers for their symptoms and experienced a milder course of the disease. It is worth noting that the mutation c.565C > T occurred most frequently, being identified in 8 out of 22 families (36%). Our team also reported five novel mutations, including c.742-744delAAG, c.383G > A, c.997G > A, c.1318C > T, and c.833T > C mutations. The identification of five novel mutations adds to the richness of the Human Genome Database. Asymptomatic heterozygotes are not uncommon, and they are prone to develop symptoms with obvious triggers. The evidence presented strongly suggest that asymptomatic individuals with family history of protein C deficiency can benefit from mutational analysis of PROC gene.
Fetal hydrocephalus and neonatal stroke as the first presentation of protein C deficiency.
Severe protein C-deficiency is a rare heritable thrombophilia of the newborn. Infants with biallelic PROC mutations present purpura fulminans and intracranial thromboembolism, while the prenatal onset of mutated heterozygotes remains unclear. We herewith present the first case of fetal ventriculomegaly and neonatal stroke associated with heterozygous PROC mutation. The infant was born to a healthy mother at 38 gestational weeks. The fetal growth had been normal, but the routine ultrasound screening had indicated mild hydrocephalus at 28 weeks of gestation. He developed convulsions two days after birth. Computed tomography of the brain revealed multiple hemorrhagic infarctions and ventriculomegaly. Dissociated levels of the plasma activity between protein C (21%) and protein S (42%) reached to determine the heterozygote of PROC c.574_576delAAG, a common thrombophilic predisposition in Asian ancestries. PC-mutant heterozygotes may have a limited high risk of cerebral thromboembolism during the perinatal course.
Peters Anomaly in Twins: A Case Report of a Rare Incident with Novel Comorbidities.
Peters anomaly is a rare developmental malformation involving the anterior segment of the eye, which culminates in amblyopia or congenital blindness. Multiple ocular and/or systemic malformations have been observed with this anomaly, and novel comorbidities continue to be reported. The probands were monozygotic twin boys (twin I and twin II) born to consanguineous parents at 36 weeks of gestation. Coarse facial features and deep-seated eyes were noted at birth. At 6 months, ophthalmic examination revealed that both twins were unable to blink in response to light, or to fixate and follow a moving object. Both twins had prominent horizontal nystagmus. Slit-lamp examination demonstrated varying degrees of central leukoma (corneal opacity) associated with iridocorneal adhesion, which is characteristic of type I Peters anomaly. No cataractous changes were observed. Normal intraocular pressure and disorganized retina were observed. Pupillary abnormalities included bilaterally underdeveloped pupils and bilateral absence of pupils was noted. Ocular MRI showed bilateral microphthalmia and optic nerve hypoplasia, with a small optic chiasm in both twins. At this age, the diagnosis of Peters anomaly was made. At 16 months of age, both twins developed deep venous thrombosis and purpuric skin lesions. Investigations revealed a hereditary thrombophilia secondary to a homozygous mutation causing protein C deficiency, which is a rare thrombotic condition. Ocular ultrasonography revealed bilateral vitreous hemorrhaging linked to altered coagulation. One twin developed bilateral inguinal hernia and cryptorchidism. The novel concordance of Peters anomaly in these monozygotic twins sharing a mutation in PROC gene provides further evidence that this anomaly has a genetic basis. Hypoplasia of the optic nerves and optic chiasm, along with severe protein C deficiency and bilateral absence of the pupils, are associated comorbidities that have not previously been reported with this anomaly.
Efficacy and safety of protein C concentrate to treat purpura fulminans and thromboembolic events in severe congenital protein C deficiency.
Severe congenital protein C (PC) deficiency (SCPCD) is associated with disseminated intravascular coagulation (DIC), purpura fulminans (PF), and vascular thromboembolic events (TE), often leading to organ failure and death. PC replacement therapy offers a safe, effective treatment for thromboembolic complications of SCPCD and secondary prophylaxis for recurrent DIC, PF, and TEs. A prospective, multi-centre, open-label, phase 2/3 study was conducted to demonstrate the safety and efficacy of protein C concentrate for treatment of PF and acute TEs. Fifteen enrolled patients with SCPCD received protein C concentrate; 11 received treatment for acute TEs (PF, 18 events; PF and other coumarin-related vascular thromboembolic events [coumarin-induced skin necrosis; CISN], 1 event; venous thrombosis, 5 events). Pre-defined efficacy criteria for treatment of acute TEs were compared with a historical control arm (i. e. patients receiving conventional therapy without protein C replacement). PF/CISN was demonstrated by pre-defined primary and secondary efficacy ratings. Primary ratings of protein C concentrate-treated episodes were significantly higher (p=0.0032) than in the historical control. For 19 PF/CISN episodes in 11 patients, 94.7 % of treatments were rated effective and 5.3 % effective with complications (not related to protein C concentrate). In a secondary efficacy rating, all treatments were rated effective (68.4 % excellent; 21.1 % good; 10.5 % fair). For 5/24 vascular thrombosis episodes, 80 % of treatments were rated excellent and 20 % were rated good. No treatment-related adverse events or serious adverse events occurred. In conclusion, protein C concentrate provides an efficacious, safe treatment for PF, CISN, and other TEs in SCPCD patients.
Publicações recentes
Congenital Protein C Deficiency Presenting as Neonatal Purpura Fulminans: A Report of Two Cases.
A Phase 1/2, Open-Label, Single-Dose, Multicenter Study to Evaluate the Pharmacokinetics and Safety of Human Plasma-Derived Protein C Concentrate in Japanese Patients with Severe Congenital Protein C Deficiency (SCPCD).
Compound Heterozygous Protein C Deficiency Presenting With Splenic Infarction After COVID-19: A Case Report.
[Plasma-derived human protein C replacement concentrate therapy in a patient with severe congenital protein C deficiency presenting with purpura fulminans and disseminated intravascular coagulation].
Pharmacokinetic Evidence Supporting Subcutaneous Use of Protein C Concentrate in Patients with Protein C Deficiency.
📚 EuropePMCmostrando 6
Clinical implications of genetic testing for congenital protein C deficiency in pregnancy.
The journal of obstetrics and gynaecology researchAnalysis of PROC mutations and clinical features in 22 unrelated families with inherited protein C deficiency.
Annals of hematologyPeters Anomaly in Twins: A Case Report of a Rare Incident with Novel Comorbidities.
Case reports in ophthalmologyEfficacy and safety of protein C concentrate to treat purpura fulminans and thromboembolic events in severe congenital protein C deficiency.
Thrombosis and haemostasisFetal hydrocephalus and neonatal stroke as the first presentation of protein C deficiency.
Brain & developmentPrenatal genetic testing for familial severe congenital protein C deficiency.
Human genome variationAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Trombofilia hereditária grave por deficiência de proteína C congênita.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Trombofilia hereditária grave por deficiência de proteína C congênita
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- Clinical implications of genetic testing for congenital protein C deficiency in pregnancy.
- Analysis of PROC mutations and clinical features in 22 unrelated families with inherited protein C deficiency.
- Fetal hydrocephalus and neonatal stroke as the first presentation of protein C deficiency.
- Peters Anomaly in Twins: A Case Report of a Rare Incident with Novel Comorbidities.
- Efficacy and safety of protein C concentrate to treat purpura fulminans and thromboembolic events in severe congenital protein C deficiency.
- Congenital Protein C Deficiency Presenting as Neonatal Purpura Fulminans: A Report of Two Cases.
- A Phase 1/2, Open-Label, Single-Dose, Multicenter Study to Evaluate the Pharmacokinetics and Safety of Human Plasma-Derived Protein C Concentrate in Japanese Patients with Severe Congenital Protein C Deficiency (SCPCD).
- Compound Heterozygous Protein C Deficiency Presenting With Splenic Infarction After COVID-19: A Case Report.
- [Plasma-derived human protein C replacement concentrate therapy in a patient with severe congenital protein C deficiency presenting with purpura fulminans and disseminated intravascular coagulation].
- Pharmacokinetic Evidence Supporting Subcutaneous Use of Protein C Concentrate in Patients with Protein C Deficiency.
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:745(Orphanet)
- MONDO:0019145(MONDO)
- GARD:16544(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar