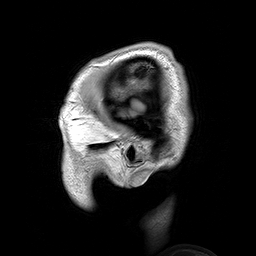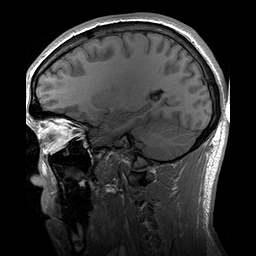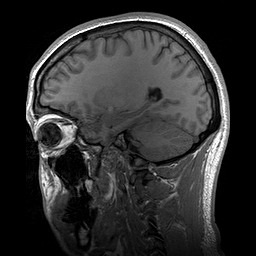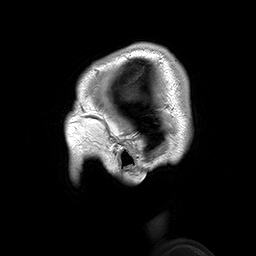
Uma doença rara que causa tumores, caracterizada pela presença de tumores de gordura (lipomas) apenas em um lado da cabeça, rosto e pescoço, e malformações no cérebro do mesmo lado.
Introdução
O que você precisa saber de cara
Uma doença rara que causa tumores, caracterizada pela presença de tumores de gordura (lipomas) apenas em um lado da cabeça, rosto e pescoço, e malformações no cérebro do mesmo lado.
Escala de raridade
<1/50kMuito rara
1/20kRara
1/10kPouco freq.
1/5kIncomum
1/2k
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Entender a doença
Do básico ao detalhe, leia no seu ritmo
Preparando trilha educativa...
Sinais e sintomas
O que aparece no corpo e com que frequência cada sintoma acontece
Partes do corpo afetadas
+ 26 sintomas em outras categorias
Características mais comuns
Os sintomas variam de pessoa para pessoa. Abaixo estão as 83 características clínicas mais associadas, ordenadas por frequência.
Linha do tempo da pesquisa
Encontrou um erro ou informação desatualizada? Sugira uma correção →
Genética e causas
O que está alterado no DNA e como passa nas famílias
Genes associados
2 genes identificados com associação a esta condição. Padrão de herança: Not applicable.
Ras proteins bind GDP/GTP and possess intrinsic GTPase activity (PubMed:20949621, PubMed:39809765). Plays an important role in the regulation of cell proliferation (PubMed:22711838, PubMed:23698361). Activates MAPK1/MAPK3 resulting in phosphorylation and ultimately degradation of GJA1 (By similarity). Plays a role in promoting oncogenic events by inducing transcriptional silencing of tumor suppressor genes (TSGs) in colorectal cancer (CRC) cells in a ZNF304-dependent manner (PubMed:24623306)
Cell membraneEndomembrane systemCytoplasm, cytosol
Leukemia, acute myelogenous
A subtype of acute leukemia, a cancer of the white blood cells. AML is a malignant disease of bone marrow characterized by maturational arrest of hematopoietic precursors at an early stage of development. Clonal expansion of myeloid blasts occurs in bone marrow, blood, and other tissue. Myelogenous leukemias develop from changes in cells that normally produce neutrophils, basophils, eosinophils and monocytes.
Tyrosine-protein kinase that acts as a cell-surface receptor for fibroblast growth factors and plays an essential role in the regulation of embryonic development, cell proliferation, differentiation and migration. Required for normal mesoderm patterning and correct axial organization during embryonic development, normal skeletogenesis and normal development of the gonadotropin-releasing hormone (GnRH) neuronal system. Phosphorylates PLCG1, FRS2, GAB1 and SHB. Ligand binding leads to the activati
Cell membraneNucleusCytoplasm, cytosolCytoplasmic vesicle
Pfeiffer syndrome
A syndrome characterized by the association of craniosynostosis, broad and deviated thumbs and big toes, and partial syndactyly of the fingers and toes. Three subtypes are known: mild autosomal dominant form (type 1); cloverleaf skull, elbow ankylosis, early death, sporadic (type 2); craniosynostosis, early demise, sporadic (type 3).
Variantes genéticas (ClinVar)
666 variantes patogênicas registradas no ClinVar.
Classificação de variantes (ClinVar)
Distribuição de 154 variantes classificadas pelo ClinVar.
Vias biológicas (Reactome)
49 vias biológicas associadas aos genes desta condição.
Diagnóstico
Os sinais que médicos procuram e os exames que confirmam
Tratamento e manejo
Remédios, cuidados de apoio e o que precisa acompanhar
Onde tratar no SUS
Hospitais de referência no Brasil e o protocolo oficial do SUS (PCDT)
🇧🇷 Atendimento SUS — Lipomatose encéfalo-cranio-cutânea
Selecione um estado ou use sua localização para ver resultados.
Dados de DATASUS/CNES, SBGM, ABNeuro e Ministério da Saúde. Sempre confirme a disponibilidade diretamente com o estabelecimento.
Pesquisa ativa
Ensaios clínicos abertos e novidades científicas recentes
Pesquisa e ensaios clínicos
Nenhum ensaio clínico registrado para esta condição.
Publicações mais relevantes
A Case of Encephalocraniocutaneous Lipomatosis (ECCL) With Atypical Clinical Presentation Diagnosed on Molecular Testing: FGFR1 ECCL Tumor Risk.
Encephalocraniocutaneous lipomatosis (ECCL) is a neurocutaneous condition caused by postzygotic mosaic activating variants in genes including FGFR1, NRAS, or KRAS. It primarily affects the skin, eyes, and central nervous system. Diagnosis is typically based on characteristic clinical features and/or molecular confirmation. Here we report a unique case of ECCL in a 12-year-old female with abdominal wall lipoma, ipsilateral lower limb overgrowth, and brachydactyly, in whom somatic mosaicism for FGFR1 was identified using resected lipomatous tissue. Imaging studies confirmed additional spinal lipomas consistent with ECCL. This report expands the phenotypic spectrum of FGFR1-ECCL and underscores the importance of tissue-based somatic testing for diagnosis. Tumor risk is also discussed.
Complex Epibulbar and Corneal Choristomas in Mosaic RASopathies.
To describe the clinical features and management of ocular choristomas in mosaic RASopathy patients. We performed a retrospective single-center case review of all mosaic RASopathy patients. We evaluated for the presence of corneal and epibulbar choristomas and conducted a comprehensive analysis of the imaging, including operative microscope images, slitlamp images, and optical coherence tomography images. In doing so, we provide a precise description for these types of choristomas. Nine patients with mosaic RASopathies, 7 men and 2 women (3 with clinical diagnoses of Linear Sebaceous Nevus Syndrome, 5 with Oculoectodermal Syndrome, and 1 with Encephalocraniocutaneous Lipomatosis), were evaluated. Fourteen eyes with ocular choristomas were identified among the 9 patients-bilaterally in 5 and unilaterally in 4. Molecular confirmation was available in 6 cases, and pathogenic variants in the KRAS gene were identified in all 6. None of the choristomas presented as discrete raised lesions at the limbus alone; they were all relatively flat, very vascularized, and in 4 of the 14 eyes, there was involvement of the visual axis, with 6 having extension with vascularization onto the cornea. All of them extended into the conjunctiva and into the sclera posteriorly. Ocular choristomas with conjunctival and scleral extension, often with concomitant corneal vessels, should alert the clinician to the possibility of a mosaic RASopathy. Management can be complicated and includes measures such as optical iridectomy, anti-VEGF injections, and refractive correction with occlusion therapy, and corneal transplantation may also be considered.
Encephalocraniocutaneous lipomatosis: a rare and sporadic phakomatosis.
Metachronous tumour (DNET and haemorrhagic chiasmal tumour) in a patient with encephalocraniocutaneous syndrome (ECCL).
Encephalocraniocutaneous lipomatosis (ECCL) is a rare neurocutaneous multisystem disorder affecting ectodermal and mesodermal tissues, including the eyes, skin, adipose tissue and the brain. It is hypothesised to be a neural crest disorder. While ECCL presents with various neurological features, the occurrence of brain tumour is an extremely rare association. Here, we report a case of metachronous tumours comprising a dysembryoplastic neuroepithelial tumour (DNET) and a haemorrhagic chiasmal tumour in a patient with ECCL. To the best of our knowledge, this is the first documented case of ECCL presenting with subarachnoid haemorrhage (SAH) in the suprasellar region due to a tumorous bleed. A woman in her mid-20s presented with a sudden onset headache and altered sensorium. Non-contrast CT of the brain showed a focal bleed in the suprasellar region with gyriform cortical calcification in the left temporoparietal lobe and left optic globe calcification. Digital subtraction angiography was inconclusive. MRI of the brain showed intracranial and intraspinal lipomas with changes suggestive of previous surgery in the left temporal lobe. A focal bleed was noticed in the optic chiasm and pial angiomas in the left temporoparietal lobe. The patient had a history of a left temporal arachnoid cyst and dysplastic left temporal lobe, for which she underwent a left temporal lobectomy to manage drug-refractory epilepsy. Histopathological examination of the resected tissue revealed a DNET with focal cortical dysplasia. The diagnosis of ECCL was established, with associated metachronous tumours identified at multiple locations in the brain. The presence of a metachronous tumour in a patient with ECCL is a rare occurrence. Hence, clinicians should maintain a high index of suspicion and ensure that such patients are monitored through long-term follow-up, with regular screening to facilitate the early detection of a second tumour.
Haberland Syndrome (Encephalocraniocutaneous Lipomatosis): A Case Report and Review of Literature.
Encephalocraniocutaneous lipomatosis (ECCL), also known as Haberland syndrome, is a rare, nonhereditary, nonprogressive congenital neurocutaneous syndrome with underlying ectodermal dysgenesis. The classic triad of this syndrome is central nervous system (CNS), ocular, and cutaneous involvement as unilateral lipomatous lesions of the scalp, neck, and face with ipsilateral brain anomalies and ipsilateral ocular choristoma. Herein, this study reports a case of a 2-year-old boy presented with status epilepticus for the first time. Intraspinal lipoma, arachnoid cyst, cerebral hemiatrophy, asymmetric hydrocephaly, choristoma, and corneal clouding were noted. This case fulfilled Moog's clinical criteria for diagnosis of Haberland syndrome. Additionally, this study introduces linear and whorled nevoid hypermelanosis and cerebral periventricular white matter hyperintensity as novel manifestations of this syndrome.
Publicações recentes
A 2-month-old infant with an alopecic plaque.
A Case of Encephalocraniocutaneous Lipomatosis (ECCL) With Atypical Clinical Presentation Diagnosed on Molecular Testing: FGFR1 ECCL Tumor Risk.
Encephalocraniocutaneous lipomatosis: a rare and sporadic phakomatosis.
Histopathologic Features and Molecular Markers of Encephalocraniocutaneous Lipomatosis (ECCL).
Complex Epibulbar and Corneal Choristomas in Mosaic RASopathies.
📚 EuropePMC139 artigos no totalmostrando 81
A Case of Encephalocraniocutaneous Lipomatosis (ECCL) With Atypical Clinical Presentation Diagnosed on Molecular Testing: FGFR1 ECCL Tumor Risk.
American journal of medical genetics. Part AEncephalocraniocutaneous lipomatosis: a rare and sporadic phakomatosis.
Anais brasileiros de dermatologiaHistopathologic Features and Molecular Markers of Encephalocraniocutaneous Lipomatosis (ECCL).
Dermatopathology (Basel, Switzerland)Complex Epibulbar and Corneal Choristomas in Mosaic RASopathies.
CorneaSturge-Weber Syndrome Without Cutaneous Stigmata Versus Encephalocraniocutaneous Lipomatosis Without Craniocutaneous Lipomatosis: A Case Report.
WMJ : official publication of the State Medical Society of WisconsinA New Case Linking a Somatic NRAS Variant to Encephalocraniocutaneous Lipomatosis.
American journal of medical genetics. Part AEncephalocraniocutaneous lipomatosis-a neuroradiological perspective.
Pediatric radiologyRASopathies. Part II: Cutaneous and extracutaneous manifestations.
Journal of the American Academy of DermatologyRASopathies. Part I: Genetics and therapeutic considerations.
Journal of the American Academy of DermatologyFunctional hemispherectomy for seizure control in encephalocraniocutaneous lipomatosis: illustrative case.
Journal of neurosurgery. Case lessonsMetachronous tumour (DNET and haemorrhagic chiasmal tumour) in a patient with encephalocraniocutaneous syndrome (ECCL).
BMJ case reportsEncephalocraniocutaneous Lipomatosis - A Rare Neurophakomatoses.
Neurology IndiaHaberland Syndrome (Encephalocraniocutaneous Lipomatosis): A Case Report and Review of Literature.
Iranian journal of child neurologyMosaic KRAS Mutation in Schimmelpenning-Feuerstein-Mims Syndrome With Overlapping Oculoectodermal Syndrome and Encephalocraniocutaneous Lipomatosis Features.
Pediatric dermatologyReview of encephalocraniocutaneous lipomatosis.
Seminars in pediatric neurologyA Hemorrhagic Brain Mass in a Child With Encephalocraniocutaneous Lipomatosis.
Journal of pediatric hematology/oncologyEncephalocraniocutaneous lipomatosis phenotype associated with mosaic biallelic pathogenic variants in the NF1 gene.
Journal of medical geneticsEncephalocraniocutaneous Lipomatosis: A Case Report.
Annals of plastic surgeryEmerging insights into cephalic neural crest disorders: A single center experience.
Journal of clinical imaging scienceHaberland Syndrome (Encephalocraniocutaneous Lipomatosis) with Development of Diffuse Leptomeningeal Glioneural Tumor (DL-GNT) during Adolescence.
Clinical neuroradiologyCalcified Sclero-Choroidal Choristomas in Mosaic RASopathies: A Description of a New Imaging Sign.
Ophthalmology. RetinaMosaic RASopathies concept: different skin lesions, same systemic manifestations?
Journal of medical geneticsNavigating the complexities of encephalocraniocutaneous lipomatosis: a case series and review.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryTeaching Neuroimage: A Rare Case of Encephalocraniocutaneous Lipomatosis: A Clinico-Radiological Diagnosis.
Neurology IndiaNext generation sequencing aids diagnosis and management in a case of encephalocraniocutaneous lipomatosis.
Pediatric dermatologyEncephalocraniocutaneous Lipomatosis: A Case Report and Literature Review.
CureusEncephalocraniocutaneous Lipomatosis, a Radiological Challenge: Two Atypical Case Reports and Literature Review.
Brain sciencesA primary DICER1-sarcoma with KRAS and TP53 mutations in a child with suspected ECCL.
Brain tumor pathologyToward clinical and molecular dissection of frontonasal dysplasia with facial skin polyps: From Pai syndrome to differential diagnosis through a series of 27 patients.
American journal of medical genetics. Part AIdentification of Codon 146 KRAS Variants in Isolated Epidermal Nevus and Multiple Lesions in Oculoectodermal Syndrome: Confirmation of the Phenotypic Continuum of Mosaic RASopathies.
International journal of molecular sciencesExpending the Phenotypic Spectrum of Encephalocraniocutaneous Lipomatosis: About a Prenatal Case With Complete Autopsy.
Pediatric and developmental pathology : the official journal of the Society for Pediatric Pathology and the Paediatric Pathology SocietyClinical and Neuroimaging Features of Encephalocraniocutaneous Lipomatosis.
NeurologyUtility of Neonatal Findings in Early Diagnosis of a Case of Haberland Syndrome.
Journal of pediatric geneticsSomatic KRAS mutation affecting codon 146 in linear sebaceous nevus syndrome.
American journal of medical genetics. Part AOphthalmic Manifestation and Pathological Features in a Cohort of Patients With Linear Nevus Sebaceous Syndrome and Encephalocraniocutaneous Lipomatosis.
Frontiers in pediatricsCase Report: A Case of Glioblastoma in a Patient With Haberland Syndrome.
Frontiers in pediatricsEncephalocraniocutaneous lipomatosıs (Haberland syndrome) in a newborn baby: a case report with review of literature.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryEncephalocraniocutaneous Lipomatosis Associated with Orbital Cyst: A Variant or New Entity?
Turkish journal of ophthalmologyIntroduction to phacomatoses (neurocutaneous disorders) in childhood.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryFibrous Meningioma in a Patient with Encephalocraniocutaneous Lipomatosis: A Rare Case with Unique Features.
International medical case reports journalHaberland syndrome with bilateral ocular involvement.
Archivos de la Sociedad Espanola de Oftalmologia[Segmental overgrowth syndromes and therapeutic strategies].
Medecine sciences : M/SEncephalocraniocutaneous lipomatosis: A rare congenital neurocutaneous syndrome.
Radiology case reportsNevus psiloliparus: Newly described histopathological features from transverse sections.
Journal of cutaneous pathologyBilateral Alopecia in a Six-year-old Boy: A Quiz.
Acta dermato-venereologicaGiant Ocular Lipodermoid Cyst in Encephalocraniocutaneous Lipomatosis: Surgical Treatment and Genetic Analysis.
The American journal of case reportsOculoectodermal Syndrome - Encephalocraniocutaneous Lipomatosis Associated with NRAS Mutation.
Acta dermato-venereologicaAnaesthetic management of a case of Haberland's syndrome (encephalocraniocutaneous lipomatosis).
Indian journal of anaesthesiaSensitive detection of FGFR1 N546K mosaic mutation in patient with encephalocraniocutaneous lipomatosis and pilocytic astrocytoma.
American journal of medical genetics. Part A18F-Fludeoxyglucose Positron-emission Tomography/Computed Tomography in Encephalocraniocutaneous Lipomatosis/Haberland Syndrome.
Indian journal of nuclear medicine : IJNM : the official journal of the Society of Nuclear Medicine, IndiaExpansion of the phenotypic spectrum and description of molecular findings in a cohort of patients with oculocutaneous mosaic RASopathies.
Molecular genetics & genomic medicineUp-regulation of fibroblast growth factor receptor 1 due to prenatal tobacco exposure can lead to developmental defects in new born.
The journal of maternal-fetal & neonatal medicine : the official journal of the European Association of Perinatal Medicine, the Federation of Asia and Oceania Perinatal Societies, the International Society of Perinatal ObstetriciansMosaic KRAS mutation in a patient with encephalocraniocutaneous lipomatosis and renovascular hypertension.
American journal of medical genetics. Part AEye and appearance characteristics of encephalocraniocutaneous lipomatosis.
Eye (London, England)Pseudodidymosis: nevus psiloliparus with aplasia cutis congenita, an initial manifestation of Haberland syndrome.
International journal of dermatologyThe impact of marine recreational fishing on key fish stocks in European waters.
PloS oneMethylome analysis and whole-exome sequencing reveal that brain tumors associated with encephalocraniocutaneous lipomatosis are midline pilocytic astrocytomas.
Acta neuropathologicaEncephalocraniocutaneous Lipomatosis.
Journal of pediatric hematology/oncologyLipomatosis encefalocraneocutánea: reporte de caso.
Gaceta medica de MexicoEncephalocraniocutaneous Lipomatosis: Haberland Syndrome.
The American journal of case reportsEncephalocraniocutaneous lipomatosis: A case report with review of literature.
The neuroradiology journalEncephalocraniocutaneous lipomatosis with Wilms' tumor.
Pediatrics international : official journal of the Japan Pediatric SocietyPartial Encephalocraniocutaneous Lipomatosis Syndrome.
Journal of pediatric neurosciencesShort stature and growth hormone deficiency in a girl with encephalocraniocutaneous lipomatosis and Jaffe-Campanacci syndrome: a case report.
Annals of pediatric endocrinology & metabolismA rare case of dysembryoplastic neuroepithelial tumor combined with encephalocraniocutaneous lipomatosis and intractable seizures.
Korean journal of pediatricsEncephalocraniocutaneous lipomatosis (Haberland syndrome): A rare case report.
Indian dermatology online journalTip of an Iceberg: Skull Fracture as an Adult Presentation of Encephalocraniocutaneous Lipomatosis.
Case reports in neurological medicineSignificant antitumor response of disseminated glioblastoma to bevacizumab resulting in long-term clinical remission in a patient with encephalocraniocutaneous lipomatosis: A case report.
Molecular and clinical oncologyEncephalocraniocutaneous lipomatosis (Fishman syndrome): A rare neurocutaneous syndrome.
Journal of current ophthalmologyHaberland syndrome: Clinical and neuroimaging findings leading to diagnosis.
NeurologiaEncephalocraniocutaneous lipomatosis (Haberland syndrome): A mild case with bilateral cutaneous and ocular involvement.
JAAD case reportsEncephalocraniocutaneous Lipomatosis Without Ocular Malformations.
Pediatric neurologySpecific mosaic KRAS mutations affecting codon 146 cause oculoectodermal syndrome and encephalocraniocutaneous lipomatosis.
Clinical geneticsMosaic Activating Mutations in FGFR1 Cause Encephalocraniocutaneous Lipomatosis.
American journal of human geneticsMosaic Neurocutaneous Disorders and Their Causes.
Seminars in pediatric neurologyNeuroimaging Findings in Encephalocraniocutaneous Lipomatosis.
Pediatric neurologyEncephalocraniocutaneous lipomatosis, a rare neurocutaneous disorder: report of additional three cases.
Child's nervous system : ChNS : official journal of the International Society for Pediatric NeurosurgeryOssifying Fibroma in a Patient With Oculocerebrocutaneous (Delleman) Syndrome.
Journal of oral and maxillofacial surgery : official journal of the American Association of Oral and Maxillofacial SurgeonsCharacteristic imaging findings in encephalocraniocutaneous lipomatosis.
NeurologyGrade II pilocytic astrocytoma in a 3-month-old patient with encephalocraniocutaneous lipomatosis (ECCL): case report and literature review of low grade gliomas in ECCL.
American journal of medical genetics. Part AEncephalocraniocutaneous Lipomatosis: A Rare Association With Tethered Spinal Cord Syndrome With Review of Literature.
Child neurology openAssociações
Organizações que acompanham esta doença — pra ter apoio e orientação
Ainda não temos associações cadastradas para Lipomatose encéfalo-cranio-cutânea.
É de uma associação que acompanha esta doença? Fale com a gente →
Comunidades
Grupos ativos de quem convive com esta doença aqui no Raras
Ainda não existe comunidade no Raras para Lipomatose encéfalo-cranio-cutânea
Pacientes, familiares e cuidadores se organizam em comunidades pra compartilhar experiências, fazer perguntas e se apoiar. Você pode ser o primeiro.
Tire suas dúvidas
Perguntas, dicas e experiências compartilhadas aqui na página
Participe da discussão
Faça login para postar dúvidas, compartilhar experiências e interagir com especialistas.
Fazer loginDoenças relacionadas
Doenças com sintomas parecidos — ajudam quem ainda está buscando diagnóstico
Referências e fontes
Bases de dados externas citadas neste artigo
Publicações científicas
Artigos indexados no PubMed ligados a esta doença no grafo RarasNet — título, periódico e PMID direto da fonte, sem intermediação de IA.
- A Case of Encephalocraniocutaneous Lipomatosis (ECCL) With Atypical Clinical Presentation Diagnosed on Molecular Testing: FGFR1 ECCL Tumor Risk.
- Complex Epibulbar and Corneal Choristomas in Mosaic RASopathies.
- Encephalocraniocutaneous lipomatosis: a rare and sporadic phakomatosis.
- Metachronous tumour (DNET and haemorrhagic chiasmal tumour) in a patient with encephalocraniocutaneous syndrome (ECCL).
- Haberland Syndrome (Encephalocraniocutaneous Lipomatosis): A Case Report and Review of Literature.
- A 2-month-old infant with an alopecic plaque.
- Histopathologic Features and Molecular Markers of Encephalocraniocutaneous Lipomatosis (ECCL).
Bases de dados e fontes oficiais
Identificadores e referências canônicas usadas para montar este verbete.
- ORPHA:2396(Orphanet)
- OMIM OMIM:613001(OMIM)
- MONDO:0013074(MONDO)
- GARD:2108(GARD (NIH))
- Variantes catalogadas(ClinVar)
- Busca completa no PubMed(PubMed)
- Q17540092(Wikidata)
Dados compilados pelo RarasNet a partir de fontes abertas (Orphanet, OMIM, MONDO, PubMed/EuropePMC, ClinicalTrials.gov, DATASUS, PCDT/MS). Este conteúdo é informativo e não substitui avaliação médica.
Conteúdo mantido por Agente Raras · Médicos e pesquisadores podem colaborar